Nutritional Strategies: Preoperative - Carb Load & Clear Rules
- Overall Goal: Minimize surgical stress, ↓ insulin resistance, improve patient comfort & outcomes.
- Preoperative Carbohydrate Loading:
- Rationale:
- Shifts patient from fasted (catabolic) to fed (anabolic-like) state.
- Reduces postoperative insulin resistance.
- ↓ Postoperative Nausea & Vomiting (PONV), anxiety, thirst; preserves lean body mass.
- Regimen (Maltodextrin-based drink):
- Evening before surgery: 50-100g carbohydrates (e.g., 400-800 ml).
- Up to 2 hours before anesthesia induction: 25-50g carbohydrates (e.g., 200-400 ml).
- Caution: Gastroparesis, severe Gastroesophageal Reflux Disease (GERD) with aspiration risk, emergency surgery. Diabetes requires careful assessment.
- Rationale:
- Preoperative Fasting Guidelines (NPO):
- Clear fluids: Permitted up to 2 hours pre-anesthesia.
- Examples: Water, clear fruit juices (no pulp), black tea/coffee (no milk), ERAS carbohydrate drinks.
- Solids (light meal): Stop 6 hours pre-anesthesia.
- Breast milk: Stop 4 hours pre-anesthesia.
- Infant formula / Non-human milk: Stop 6 hours pre-anesthesia.
- Chewing gum: Remove 2 hours pre-anesthesia.

- Clear fluids: Permitted up to 2 hours pre-anesthesia.
⭐ The primary benefit of preoperative carbohydrate loading is mitigating the surgical stress response and reducing postoperative insulin resistance, which can improve glycemic control and potentially shorten recovery times and hospital stay.
Nutritional Strategies: Postoperative & Gut Revival - Eat Early, Move Gut
- Early Oral Nutrition (EON):
- Initiate: Within <24 hours postoperatively, even after major gastrointestinal surgery, unless contraindicated (e.g., shock, obstruction).
- Dietary Advancement: Start with clear liquids, progress rapidly to soft then normal diet as tolerated by the patient.
- Advantages: ↓ infectious complications, ↓ length of hospital stay (LOS), preserves gut mucosal integrity, ↓ incidence of postoperative ileus.
- Strategies to Stimulate Gut Function:
- Chewing Gum: 📌 "Chew to Churn!" Acts as sham feeding, stimulating cephalic-vagal pathways to promote gut motility. Recommended 3-4 times daily for 15-30 minutes.
- Alvimopan (Entereg®): A peripherally acting mu-opioid receptor antagonist (PAMORA).
- Indication: To accelerate GI recovery (time to first bowel movement/flatus) following partial large or small bowel resection with primary anastomosis.
- Dosing: 12 mg orally 30 min to 5 hours pre-surgery, then 12 mg BID post-operatively for up to 7 days or until discharge (maximum 15 doses).
- Prokinetics (e.g., metoclopramide): Limited role; not routinely advised in most ERAS protocols. Consider for select high-risk patients.
- Supportive Measures for Gut Revival:
- Opioid Sparing: Critical, as opioids significantly delay gut recovery. Prioritize multimodal, non-opioid analgesia.
- Early Mobilization: Encourages return of bowel function and is synergistic with nutritional strategies.
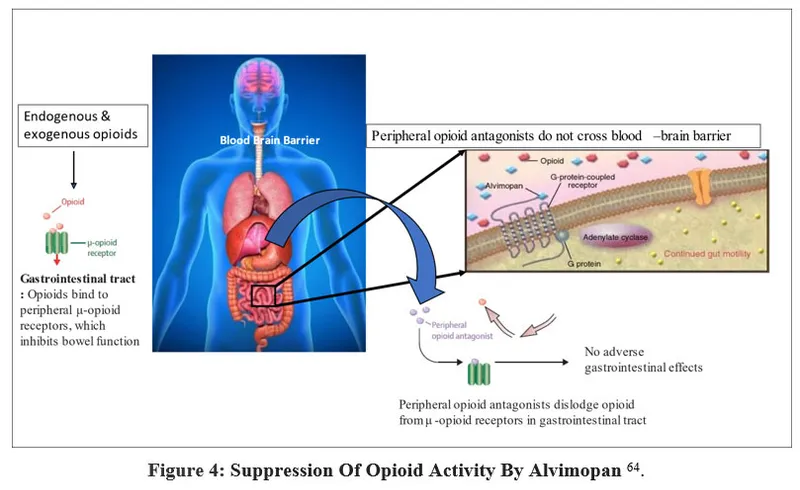
⭐ Alvimopan selectively antagonizes mu-opioid receptors in the gastrointestinal tract, thereby reducing opioid-induced constipation and postoperative ileus without affecting central analgesia or precipitating withdrawal.
Nutritional Strategies: Fluids & Special Needs - Balancing Act & Tailored Care
Fluid Management: The Balancing Act
- Goal: Maintain euovolemia; avoid both overload & deficit.
- ERAS Approach: Goal-Directed Fluid Therapy (GDFT).
- Restrictive crystalloid use intraoperatively.
- Monitor: Urine output > 0.5 mL/kg/hr, lactate, hemodynamics.
- Post-op: Rapid transition to oral fluids.
Tailored Care for Special Needs:
- Malnutrition:
- Screen (e.g., NRS-2002, MUST).
- Pre-op: Oral Nutritional Supplements (ONS); consider immunonutrition for 7-14 days if severe.
- Diabetes Mellitus:
- Perioperative glycemic control: Target 140-180 mg/dL. Avoid hypoglycemia.
- Obesity:
- Protein needs may be higher; calculate based on ideal/adjusted body weight.
- Organ Dysfunction (Renal/Hepatic):
- Individualize: Modify fluid, electrolytes, and protein based on specific limitations.
⭐ > Early initiation of oral clear liquids, often within hours after surgery, is a key ERAS principle that significantly reduces reliance on IV fluids and promotes faster gut function recovery.
High‑Yield Points - ⚡ Biggest Takeaways
- Preoperative carbohydrate loading (clear, non-particulate) 2-3 hours before surgery reduces insulin resistance.
- Avoid prolonged fasting: Clear fluids up to 2 hours, solids up to 6 hours preoperatively.
- Initiate early oral nutrition (within 24 hours post-op) to stimulate gut function.
- Avoid routine NG tubes; remove early if placed.
- Screen for malnutrition preoperatively and optimize if needed.
- Consider oral nutritional supplements (ONS) if postoperative intake is <60% of needs.
- Maintain perioperative glycemic control.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

