Enhanced Recovery After Surgery (ERAS)

On this page
🚀 ERAS Revolution: The Surgical Recovery Transformation
Enhanced Recovery After Surgery protocols represent one of modern medicine's most successful paradigm shifts, transforming surgical care from tradition-based practices into evidence-driven pathways that cut complications by half and send patients home days earlier. You'll master the architecture behind ERAS implementation, from preoperative optimization through discharge planning, learning how multidisciplinary coordination and specific interventions create measurable improvements in outcomes. This lesson equips you with the clinical algorithms, evidence frameworks, and system integration strategies to champion recovery protocols that simultaneously improve patient experience and institutional efficiency.
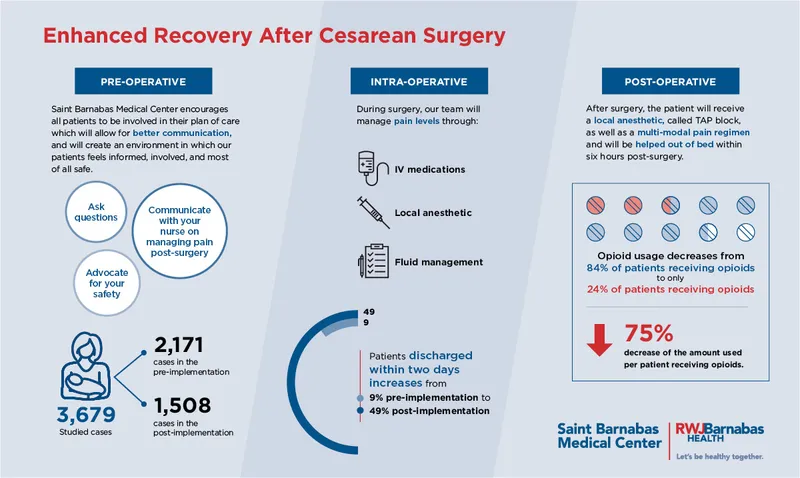
📌 Remember: ERAS = Evidence-based Recovery Acceleration System - Every intervention must have Level 1 evidence supporting faster recovery, reduced complications, or improved patient satisfaction
The foundation of ERAS rests on 4 core principles that challenge traditional surgical dogma:
-
Physiological Optimization
- Minimize surgical stress response through multimodal interventions
- Maintain homeostasis with goal-directed therapy
- Preserve organ function through evidence-based protocols
- Cardiac output optimization: >2.5 L/min/m²
- Fluid balance: Zero to negative 1L by POD 1
- Glycemic control: <180 mg/dL perioperatively
-
Patient Engagement & Education
- Structured preoperative counseling reduces anxiety by 25-40%
- Written protocols improve compliance by 60-80%
- Shared decision-making enhances satisfaction scores by 15-30%
-
Multidisciplinary Coordination
- Surgeon-anesthesiologist-nursing collaboration
- Standardized order sets reduce variation by 70%
- Daily huddles improve protocol adherence to >90%
-
Continuous Quality Improvement
- Real-time outcome tracking with monthly audits
- Benchmark comparisons against international databases
- Protocol refinement based on institution-specific data
⭐ Clinical Pearl: ERAS protocols demonstrate dose-response relationships - institutions implementing >70% of recommended elements achieve maximum benefit, while partial implementation yields proportionally reduced outcomes
| ERAS Component | Traditional Approach | ERAS Protocol | Evidence Level | Outcome Improvement |
|---|---|---|---|---|
| Preoperative Fasting | 12+ hours NPO | 2 hours clear fluids | Level 1A | ↓30% insulin resistance |
| Fluid Management | Liberal crystalloids | Goal-directed therapy | Level 1A | ↓40% complications |
| Pain Control | Opioid-centric | Multimodal analgesia | Level 1A | ↓50% opioid consumption |
| Mobilization | Bed rest 3-5 days | 6-24 hours ambulation | Level 1A | ↓60% thromboembolism |
| Nutrition | NPO until flatus | 4-6 hours feeding | Level 1A | ↓25% length of stay |
The physiological rationale underlying ERAS interventions targets the surgical stress response cascade. Traditional perioperative care inadvertently amplifies this response through prolonged fasting, excessive fluid administration, and delayed mobilization. ERAS protocols systematically attenuate each component:
- Neuroendocrine Response: Reduced by 40-60% through regional anesthesia and multimodal analgesia
- Inflammatory Cascade: Minimized via early feeding and goal-directed fluid therapy
- Metabolic Dysfunction: Prevented through carbohydrate loading and glycemic optimization
- Organ System Deconditioning: Avoided via early mobilization and functional preservation
Understanding these foundational principles sets the stage for exploring the specific implementation strategies that transform surgical outcomes across diverse patient populations.
🚀 ERAS Revolution: The Surgical Recovery Transformation
⚙️ Implementation Architecture: Building the ERAS Engine
📌 Remember: TEAM = Together Everyone Achieves More - Successful ERAS requires Surgeon champions, Anesthesia leaders, Nursing coordinators, Pharmacy specialists, Physical therapy, and Administrative support
The multidisciplinary team structure forms the operational backbone of ERAS success:
-
ERAS Steering Committee
- Executive sponsor with budget authority
- Department chiefs from surgery, anesthesia, nursing
- Quality improvement director
- Meets monthly for strategic oversight
- Reviews compliance metrics: target >85%
- Addresses implementation barriers
- Approves protocol modifications
-
ERAS Working Groups (Service-Specific)
- Colorectal surgery: 15-20 protocol elements
- Orthopedic surgery: 12-18 protocol elements
- Gynecologic surgery: 10-15 protocol elements
- Each group develops specialty-specific pathways
- Adapts core ERAS principles to surgical requirements
- Creates standardized order sets
- Establishes outcome benchmarks
-
ERAS Coordinators (Dedicated Personnel)
- 1.0 FTE coordinator per 200-300 ERAS cases annually
- Responsibilities include patient education, protocol monitoring, data collection
- Achieves 15-25% improvement in adherence rates
⭐ Clinical Pearl: Institutions with dedicated ERAS coordinators achieve 92% average protocol adherence compared to 67% in programs relying solely on existing staff
| Implementation Phase | Duration | Key Activities | Success Metrics | Common Barriers |
|---|---|---|---|---|
| Leadership Commitment | 1-2 months | Executive buy-in, resource allocation | Budget approval, champion identification | Competing priorities, cost concerns |
| Team Formation | 2-3 months | Recruit multidisciplinary members | >80% attendance at meetings | Scheduling conflicts, role clarity |
| Protocol Development | 3-4 months | Adapt evidence to local context | Consensus on >90% elements | Specialty-specific disagreements |
| Staff Education | 2-3 months | Training programs, competency validation | >85% staff completion rates | Time constraints, resistance to change |
| Pilot Implementation | 3-6 months | Limited rollout, rapid cycle improvement | >70% adherence in pilot group | Workflow disruptions, communication gaps |
| Full Rollout | 6-12 months | System-wide implementation | >80% adherence across all services | Resource limitations, sustainability |
-
Physician Engagement
- Champion identification: Early adopters with peer credibility
- Data transparency: Monthly scorecards showing individual and group performance
- Incentive alignment: Quality metrics tied to compensation models
- Length of stay reduction: target 20-30%
- Complication rates: target 15-25% reduction
- Patient satisfaction: target >90th percentile
-
Nursing Integration
- Workflow redesign: Eliminate non-value-added activities
- Competency-based training: 8-12 hour ERAS certification programs
- Decision support tools: Electronic reminders for time-sensitive interventions
-
Patient Preparation
- Preoperative education classes: 60-90 minute sessions
- Written materials: 6th grade reading level for accessibility
- Digital platforms: Mobile apps for real-time guidance
💡 Master This: ERAS implementation success correlates directly with leadership engagement intensity - programs with weekly executive rounds and monthly performance reviews achieve 2-3x higher adherence rates than those with quarterly oversight
The technology infrastructure enables real-time monitoring and continuous improvement:
-
Electronic Health Record Integration
- Automated order sets reduce ordering errors by 60-80%
- Clinical decision support provides point-of-care reminders
- Outcome tracking enables risk-adjusted benchmarking
-
Data Analytics Platforms
- Real-time dashboards showing protocol adherence
- Predictive modeling for complication risk stratification
- Comparative effectiveness analysis across patient populations
This systematic approach to implementation creates the foundation for exploring the specific clinical protocols that drive superior patient outcomes.
⚙️ Implementation Architecture: Building the ERAS Engine
🎯 Protocol Mastery: The Clinical Decision Framework
The preoperative optimization framework establishes the foundation for accelerated recovery:
-
Risk Stratification Patterns
- ASA I-II patients: Standard ERAS protocol with full intervention suite
- ASA III patients: Modified protocol with enhanced monitoring
- ASA IV patients: Selective ERAS elements with individualized approach
- Cardiac optimization: >50% ejection fraction target
- Pulmonary function: >60% predicted FEV1 threshold
- Nutritional status: >18.5 BMI and albumin >3.0 g/dL
-
Intervention Timing Patterns
- 2-4 weeks preoperatively: Prehabilitation, smoking cessation, nutritional optimization
- 24-48 hours preoperatively: Carbohydrate loading, medication adjustments
- 2-6 hours preoperatively: Clear fluid intake, anxiolysis, antibiotic prophylaxis
- Carbohydrate drink: 400 mL at bedtime, 200 mL 2 hours before surgery
- Clear fluids: Unlimited until 2 hours before anesthesia
- Antiemetic prophylaxis: 2-3 agents for high-risk patients
📌 Remember: PREP = Prehab, Risk-assess, Educate, Prepare - Every preoperative intervention must target specific physiological optimization with measurable endpoints
The intraoperative management patterns focus on physiological preservation:
-
Anesthetic Approach Recognition
- Regional anesthesia preferred: Reduces opioid requirements by 60-80%
- Goal-directed fluid therapy: Maintains stroke volume optimization
- Multimodal analgesia: Combines 3-4 analgesic modalities
- Neuraxial blocks: Duration 12-24 hours for major procedures
- Peripheral nerve blocks: Single-shot or continuous based on surgery
- Systemic adjuvants: Acetaminophen 1g q6h, ketorolac 30mg q6h
-
Fluid Management Patterns
- Restrictive approach: 4-6 mL/kg/hour maintenance
- Goal-directed therapy: Stroke volume variation <13%
- Balanced crystalloids: Lactated Ringer's or Plasma-Lyte
- Avoid >2L positive balance intraoperatively
- Target mean arterial pressure >65 mmHg
- Maintain urine output >0.5 mL/kg/hour
-
Surgical Technique Integration
- Minimally invasive approaches: Laparoscopic or robotic when feasible
- Tissue handling optimization: Gentle manipulation, minimal retraction
- Drain avoidance: Selective placement based on evidence-based criteria
⭐ Clinical Pearl: Intraoperative goal-directed fluid therapy combined with regional anesthesia reduces postoperative complications by 35-45% compared to traditional management, with greatest benefit in major abdominal and orthopedic procedures
| Surgical Specialty | Key ERAS Elements | Adherence Targets | Outcome Benchmarks |
|---|---|---|---|
| Colorectal Surgery | 18-22 interventions | >85% compliance | LOS <4 days, <15% complications |
| Orthopedic Surgery | 15-18 interventions | >80% compliance | LOS <3 days, <10% readmissions |
| Gynecologic Surgery | 12-16 interventions | >85% compliance | LOS <2 days, >95% same-day discharge |
| Cardiac Surgery | 20-25 interventions | >75% compliance | LOS <5 days, <20% complications |
| Urologic Surgery | 14-18 interventions | >80% compliance | LOS <2 days, <8% complications |
-
Early Recovery Milestones
- 0-4 hours: Awake, alert, minimal nausea, pain <4/10
- 4-8 hours: Sitting up, sipping fluids, urinating spontaneously
- 8-24 hours: Walking >100 feet, tolerating clear liquids
- Mobilization: Out of bed within 6 hours for most procedures
- Nutrition: Clear liquids within 4 hours, regular diet within 24 hours
- Catheter removal: Within 24-48 hours unless contraindicated
-
Complication Prevention Patterns
- Nausea/vomiting: <20% incidence with multimodal prophylaxis
- Ileus prevention: Early feeding plus prokinetic agents
- Thromboembolism: Sequential compression plus early ambulation
- PONV prophylaxis: 2-3 agents for moderate risk, 3-4 agents for high risk
- VTE prevention: Mechanical prophylaxis within 6 hours, chemical prophylaxis per guidelines
- Infection prevention: Appropriate antibiotics, normothermia, glycemic control
💡 Master This: ERAS protocol success requires real-time pattern recognition - when patients deviate from expected recovery milestones, immediate root cause analysis and protocol adjustment prevent cascade complications
This systematic approach to protocol execution creates the foundation for analyzing the comparative effectiveness of different ERAS strategies across diverse patient populations.
🎯 Protocol Mastery: The Clinical Decision Framework
🔬 Evidence Integration: The Comparative Effectiveness Matrix
The intervention-specific evidence hierarchy guides protocol prioritization:
-
Tier 1 Interventions (Strongest Evidence)
- Preoperative carbohydrate loading: RR 0.69 for insulin resistance
- Goal-directed fluid therapy: RR 0.61 for complications
- Regional anesthesia: RR 0.55 for opioid consumption
- Early mobilization: RR 0.48 for thromboembolism
- Number needed to treat: 4-8 patients for major benefit
- Effect size: Cohen's d >0.8 (large effect)
- Consistency: I² <25% across meta-analyses
-
Tier 2 Interventions (Moderate Evidence)
- Multimodal analgesia: RR 0.72 for chronic pain
- Minimally invasive surgery: RR 0.78 for complications
- Early feeding: RR 0.81 for length of stay
- Drain avoidance: RR 0.85 for infections
- Number needed to treat: 8-15 patients for benefit
- Effect size: Cohen's d 0.5-0.8 (moderate effect)
- Consistency: I² 25-50% across studies
-
Tier 3 Interventions (Emerging Evidence)
- Prehabilitation programs: RR 0.88 for complications
- Enhanced recovery education: RR 0.91 for satisfaction
- Standardized discharge criteria: RR 0.93 for readmissions
- Number needed to treat: 15-25 patients for benefit
- Effect size: Cohen's d 0.2-0.5 (small to moderate)
- Consistency: I² >50% across studies
📌 Remember: GRADE = Grading Recommendations Assessment Development Evaluation - ERAS interventions require High quality evidence (Grade A) for core elements, Moderate quality (Grade B) for supplementary elements
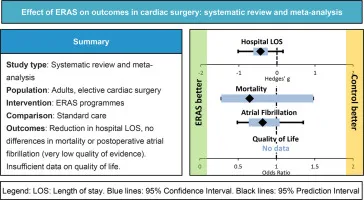
The specialty-specific effectiveness patterns reveal important treatment heterogeneity:
| Intervention | Colorectal Surgery | Orthopedic Surgery | Gynecologic Surgery | Cardiac Surgery | Urologic Surgery |
|---|---|---|---|---|---|
| Carbohydrate Loading | RR 0.65 (CI: 0.52-0.81) | RR 0.78 (CI: 0.61-0.99) | RR 0.72 (CI: 0.58-0.89) | RR 0.85 (CI: 0.69-1.05) | RR 0.71 (CI: 0.55-0.92) |
| Regional Anesthesia | RR 0.58 (CI: 0.45-0.75) | RR 0.42 (CI: 0.31-0.57) | RR 0.67 (CI: 0.51-0.88) | RR 0.89 (CI: 0.72-1.10) | RR 0.61 (CI: 0.46-0.81) |
| Early Mobilization | RR 0.51 (CI: 0.38-0.68) | RR 0.35 (CI: 0.24-0.51) | RR 0.72 (CI: 0.55-0.94) | RR 0.48 (CI: 0.33-0.70) | RR 0.68 (CI: 0.49-0.94) |
| Goal-Directed Fluids | RR 0.62 (CI: 0.47-0.82) | RR 0.71 (CI: 0.54-0.93) | RR 0.58 (CI: 0.41-0.82) | RR 0.55 (CI: 0.39-0.77) | RR 0.69 (CI: 0.51-0.93) |
| Early Feeding | RR 0.73 (CI: 0.59-0.90) | RR 0.91 (CI: 0.75-1.10) | RR 0.68 (CI: 0.52-0.89) | RR 0.82 (CI: 0.66-1.02) | RR 0.77 (CI: 0.61-0.97) |
-
Age-Related Patterns
- <65 years: Full ERAS protocol achieves maximum benefit
- 65-80 years: Modified protocol with enhanced monitoring
- >80 years: Selective interventions based on frailty assessment
- Young patients: 30-40% LOS reduction with complete ERAS
- Elderly patients: 15-25% LOS reduction with tailored approach
- Frail patients: Focus on safety over speed of recovery
-
Comorbidity-Specific Modifications
- Diabetes mellitus: Enhanced glycemic monitoring, modified carbohydrate loading
- Cardiac disease: Fluid restriction, cardiac output monitoring
- Renal impairment: Medication dosing, fluid balance optimization
- Diabetic patients: Target glucose <180 mg/dL perioperatively
- Cardiac patients: CVP monitoring with fluid challenges
- Renal patients: Creatinine-based dosing for nephrotoxic medications
-
Surgical Complexity Adjustments
- Minor procedures: Ambulatory ERAS with same-day discharge
- Major procedures: Inpatient ERAS with 23-hour observation
- Complex procedures: ICU-modified ERAS with extended monitoring
⭐ Clinical Pearl: Dose-response relationships exist for ERAS interventions - implementing >80% of protocol elements yields exponential benefits, while <60% implementation provides minimal improvement over traditional care
The economic effectiveness analysis demonstrates cost-benefit optimization:
-
Direct Cost Savings
- Length of stay reduction: $1,200-2,400 per day saved
- Complication prevention: $3,000-15,000 per complication avoided
- Readmission reduction: $8,000-12,000 per readmission prevented
- ROI calculation: $3-5 saved for every $1 invested in ERAS
- Break-even point: 50-75 cases for most surgical services
- Maximum benefit: >500 cases annually per service line
-
Quality-Adjusted Outcomes
- Patient satisfaction: 15-25 point improvement on HCAHPS scores
- Functional recovery: 7-14 days faster return to baseline
- Quality of life: 0.1-0.2 QALY improvement at 6 months
💡 Master This: Evidence-based ERAS implementation requires continuous outcome monitoring with risk-adjusted benchmarking - successful programs achieve top decile performance through systematic quality improvement and protocol refinement
This comprehensive evidence framework establishes the foundation for developing advanced treatment algorithms that optimize outcomes across diverse clinical scenarios.
🔬 Evidence Integration: The Comparative Effectiveness Matrix
⚡ Treatment Optimization: The Clinical Algorithm Engine
The dynamic risk stratification algorithm continuously recalibrates treatment intensity:
Risk Stratification Scoring System:
- Age >75 years: +2 points
- ASA ≥3: +2 points
- Major comorbidities: +1 point each (diabetes, cardiac disease, COPD)
- Complex surgery: +2 points (>4 hours, multiple organs)
- Emergency surgery: +3 points
- Frailty indicators: +1-3 points based on assessment
📌 Remember: ADAPT = Assess, Decide, Act, Plan, Track - ERAS algorithms must continuously monitor patient status and automatically trigger appropriate intervention escalations or de-escalations
The intervention intensity algorithms match treatment to patient needs:
-
Standard Protocol (Low Risk: 0-2 points)
- Full ERAS implementation: 18-22 interventions
- Routine monitoring: Q4-6 hour assessments
- Expected outcomes: LOS 1-3 days, <10% complications
- Discharge criteria: Pain <4/10, tolerating diet, ambulating independently
- Monitoring frequency: Standard nursing assessments
- Intervention thresholds: Protocol-driven care
-
Enhanced Protocol (Moderate Risk: 3-5 points)
- Modified ERAS: 15-18 interventions with safety modifications
- Increased monitoring: Q2-4 hour assessments
- Expected outcomes: LOS 2-4 days, 10-20% complications
- Additional monitoring: Cardiac telemetry, hourly I/O
- Modified goals: Pain <5/10, assisted ambulation acceptable
- Escalation triggers: Deviation from milestones >12 hours
-
Intensive Protocol (High Risk: 6+ points)
- Selective ERAS: 10-15 interventions prioritizing safety over speed
- Continuous monitoring: ICU-level surveillance
- Expected outcomes: LOS 3-7 days, 20-35% complications
- Monitoring requirements: Continuous vital signs, laboratory q6-8h
- Modified expectations: Slower recovery trajectory acceptable
- Safety priorities: Complication prevention over rapid discharge
The complication prevention algorithms provide early warning systems:
| Complication Risk | Early Indicators | Intervention Triggers | Prevention Protocol |
|---|---|---|---|
| Postoperative Ileus | No flatus >24h, distension, nausea | Nasogastric decompression, prokinetics | Gum chewing, early ambulation, fluid optimization |
| Respiratory Complications | SpO2 <95%, RR >24, decreased effort | Incentive spirometry, CPAP, chest PT | Lung expansion, pain control, early mobilization |
| Cardiac Events | HR >100, BP instability, chest pain | ECG monitoring, troponin levels, cardiology consult | Fluid optimization, beta-blockers, statin therapy |
| Thromboembolism | Leg swelling, chest pain, dyspnea | Duplex ultrasound, CT-PE, anticoagulation | Sequential compression, early ambulation, prophylaxis |
| Surgical Site Infection | Fever >38.5°C, wound erythema, drainage | Wound culture, imaging, antibiotic therapy | Normothermia, glycemic control, appropriate antibiotics |
The personalized recovery algorithms optimize individual patient trajectories:
-
Fast-Track Candidates (Optimal Response)
- Criteria: Pain <3/10, no nausea, ambulating >200 feet, tolerating diet
- Accelerated pathway: Discharge 12-24 hours earlier than standard
- Success rate: 75-85% of low-risk patients
- Same-day discharge: Appropriate for minor procedures in healthy patients
- 23-hour observation: Standard for moderate procedures
- Early discharge: 24-48 hours for major procedures
-
Standard Recovery (Expected Response)
- Criteria: Meeting 80% of milestones within expected timeframes
- Standard pathway: Protocol-driven care with routine monitoring
- Success rate: 85-95% of moderate-risk patients
-
Slow Recovery (Delayed Response)
- Criteria: Missing >20% of milestones or complication development
- Extended pathway: Root cause analysis and protocol modification
- Intervention rate: 10-20% of patients require pathway adjustment
- Barrier identification: Pain control, nausea, mobility limitations
- Targeted interventions: Multimodal analgesia, antiemetics, physical therapy
- Timeline adjustment: Realistic expectations based on individual factors
💡 Master This: Successful ERAS programs use real-time analytics to identify recovery trajectory deviations within 6-12 hours, enabling immediate intervention that prevents cascade complications and prolonged stays
The quality improvement algorithms drive continuous optimization:
-
Outcome Monitoring Dashboard
- Real-time metrics: Length of stay, complication rates, readmissions
- Benchmark comparisons: National databases, peer institutions
- Trend analysis: Monthly performance with statistical process control
-
Protocol Refinement Cycles
- Quarterly reviews: Adherence rates, outcome analysis, barrier identification
- Rapid cycle improvement: PDSA methodology for protocol modifications
- Evidence integration: New research incorporated into existing protocols
This systematic approach to treatment optimization creates the foundation for exploring advanced integration strategies that maximize ERAS effectiveness across complex healthcare systems.
⚡ Treatment Optimization: The Clinical Algorithm Engine
🌐 System Integration: The Healthcare Ecosystem Orchestration
The multi-setting care coordination model ensures continuity across transitions:
-
Preoperative Optimization Centers
- 2-4 week lead time for comprehensive assessment
- Multidisciplinary clinics: Surgery, anesthesia, nursing, pharmacy
- Standardized protocols: Risk stratification, optimization plans, patient education
- Prehabilitation programs: Exercise, nutrition, smoking cessation
- Medical optimization: Cardiac clearance, glycemic control, medication management
- Patient preparation: Education classes, expectation setting, discharge planning
-
Perioperative Care Units
- Dedicated ERAS beds: Specialized nursing, protocol adherence, outcome tracking
- Technology integration: Electronic order sets, clinical decision support, real-time monitoring
- Team coordination: Daily huddles, multidisciplinary rounds, communication protocols
- Nursing ratios: 1:3-4 patients for enhanced monitoring
- Physician coverage: 24/7 availability with ERAS expertise
- Support services: Physical therapy, nutrition, case management
-
Post-Acute Care Networks
- Home health integration: ERAS-trained providers, standardized assessments, communication protocols
- Outpatient follow-up: Telemedicine platforms, remote monitoring, early intervention
- Rehabilitation services: Physical therapy, occupational therapy, nutritional counseling
📌 Remember: SEAMLESS = Systematic Engagement Across Multiple Locations Ensuring Smooth Surgical recovery - Integration success requires standardized protocols that transcend organizational boundaries
The technology integration architecture enables real-time coordination:
-
Electronic Health Record Optimization
- Interoperable systems: Data sharing across care settings
- Clinical decision support: Automated reminders, protocol guidance, outcome prediction
- Quality metrics: Real-time dashboards, performance tracking, benchmark comparisons
- Order set standardization: >95% utilization of ERAS-specific orders
- Documentation templates: Structured data capture for outcome analysis
- Alert systems: Protocol deviations, milestone delays, complication risks
-
Communication Platforms
- Secure messaging: HIPAA-compliant communication between care teams
- Patient portals: Education materials, recovery tracking, provider communication
- Mobile applications: Real-time updates, symptom reporting, medication reminders
-
Analytics and Reporting Systems
- Predictive modeling: Risk stratification, outcome prediction, resource planning
- Performance dashboards: Individual, department, and system-level metrics
- Benchmarking tools: National comparisons, best practice identification, improvement opportunities
| Integration Component | Implementation Timeline | Resource Requirements | Success Metrics |
|---|---|---|---|
| EHR Optimization | 6-12 months | IT support, clinical champions, training programs | >90% order set utilization |
| Care Coordination | 3-6 months | Care coordinators, communication protocols, workflow redesign | <24 hour response times |
| Quality Monitoring | 2-4 months | Analytics platform, data analysts, reporting infrastructure | Real-time dashboards |
| Patient Engagement | 4-8 months | Portal development, mobile apps, patient education | >80% patient activation |
| Provider Training | 6-12 months | Education programs, competency validation, ongoing support | >85% staff certification |
-
Leadership Alignment
- Executive sponsorship: CEO/CMO commitment with resource allocation
- Physician champions: Early adopters with peer credibility and change management skills
- Department integration: Surgery, anesthesia, nursing working as unified team
- Governance structure: ERAS steering committee with decision-making authority
- Performance incentives: Quality metrics tied to compensation models
- Resource commitment: Dedicated FTEs for program coordination
-
Staff Engagement and Training
- Competency-based education: Role-specific training with certification requirements
- Workflow integration: Process redesign that eliminates non-value-added activities
- Feedback systems: Regular performance updates and recognition programs
-
Patient and Family Engagement
- Shared decision-making: Informed consent with realistic expectations
- Education programs: Preoperative classes, written materials, digital resources
- Support systems: Peer mentoring, family involvement, community resources
⭐ Clinical Pearl: Healthcare systems achieving >90% ERAS protocol adherence demonstrate strong executive leadership, physician engagement, and dedicated program coordination - these organizational factors predict success more than clinical factors
The financial integration model aligns economic incentives with quality outcomes:
-
Value-Based Contracting
- Bundled payments: Episode-based reimbursement that rewards efficiency
- Quality bonuses: Performance incentives for outcome achievement
- Risk sharing: Upside/downside arrangements that align provider incentives
- Target metrics: Length of stay, complication rates, readmissions, patient satisfaction
- Benchmark performance: Top quartile achievement for maximum reimbursement
- Continuous improvement: Annual target adjustments based on performance trends
-
Cost Management Strategies
- Resource optimization: Standardized supplies, efficient workflows, waste reduction
- Capacity management: Predictable throughput, reduced variability, improved utilization
- Outcome improvement: Complication prevention, readmission reduction, patient satisfaction
💡 Master This: Successful ERAS system integration requires 3-5 year strategic commitment with sustained leadership support - organizations achieving transformational results invest consistently in people, processes, and technology while maintaining focus on patient-centered outcomes
This comprehensive integration framework establishes the foundation for developing rapid mastery tools that enable immediate clinical application of ERAS principles.
🌐 System Integration: The Healthcare Ecosystem Orchestration
🎯 Clinical Mastery Arsenal: The Rapid Reference Toolkit
📌 Remember: MASTER = Monitor, Assess, Select, Treat, Evaluate, Refine - Clinical excellence requires systematic approaches that consistently deliver optimal outcomes across diverse patient populations
Essential ERAS Numbers - Commit to Memory:
- Carbohydrate loading: 400 mL at bedtime, 200 mL 2 hours preop
- Clear fluid cutoff: 2 hours before anesthesia induction
- Goal-directed fluid therapy: 4-6 mL/kg/hour maintenance
- Early mobilization: Within 6-24 hours postoperatively
- Pain target: <4/10 for optimal recovery
- Length of stay reduction: 30-50% with full ERAS implementation
- Complication reduction: 40-60% across major surgical procedures
- Protocol adherence target: >80% for maximum benefit
- Cost savings: $3-5 return for every $1 invested
- Patient satisfaction improvement: 15-25 points on HCAHPS scores
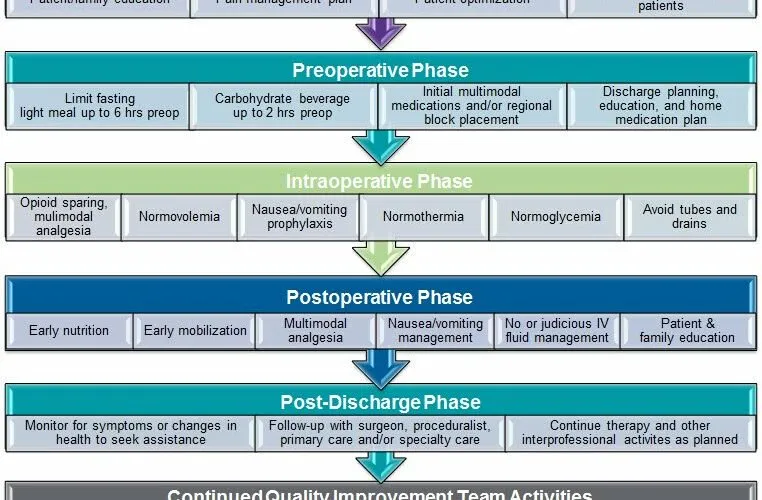
Rapid Risk Stratification Tool:
| Risk Factor | Points | Clinical Significance |
|---|---|---|
| Age >75 years | +2 | Increased frailty, slower recovery |
| ASA ≥3 | +2 | Multiple comorbidities, higher risk |
| Emergency surgery | +3 | Unprepared patient, acute illness |
| Complex procedure >4 hours | +2 | Greater physiological stress |
| Diabetes mellitus | +1 | Metabolic complications, infection risk |
| Cardiac disease | +1 | Hemodynamic instability risk |
| COPD/respiratory disease | +1 | Pulmonary complications |
| Obesity BMI >35 | +1 | Technical challenges, complications |
| Frailty indicators | +1-3 | Functional decline, poor reserves |
| Previous complications | +1 | Higher risk profile |
- 0-2 points: Low risk - Full ERAS protocol
- 3-5 points: Moderate risk - Enhanced monitoring
- 6+ points: High risk - Selective interventions
⭐ Clinical Pearl: Risk stratification should be dynamic - reassess every 12-24 hours and adjust protocols based on patient response and recovery milestones
ERAS Intervention Priority Matrix:
-
Must-Have Interventions (Evidence Grade A)
- Preoperative carbohydrate loading (unless contraindicated)
- Goal-directed fluid therapy with stroke volume optimization
- Regional anesthesia when anatomically feasible
- Early mobilization within 6-24 hours
- Multimodal analgesia with opioid-sparing approach
-
Should-Have Interventions (Evidence Grade B)
- Prehabilitation for high-risk patients
- Minimally invasive surgical techniques
- Early feeding within 4-6 hours
- Standardized antiemetic prophylaxis
- Thromboembolism prevention protocols
-
Could-Have Interventions (Evidence Grade C)
- Enhanced patient education programs
- Music therapy for anxiety reduction
- Chewing gum for ileus prevention
- Probiotics for infection prevention
- Acupuncture for nausea control
Complication Prevention Checklist:
💡 Master This: Prevention is exponentially more effective than treatment - systematic prevention protocols reduce complications by 40-60% while treatment protocols only minimize severity
-
Postoperative Nausea and Vomiting (PONV)
- Risk assessment: Apfel score or simplified risk factors
- Prophylaxis protocol: 2-4 agents based on risk level
- Rescue therapy: Different mechanism than prophylaxis
- Low risk (0-1 factors): 1-2 agents
- Moderate risk (2 factors): 2-3 agents
- High risk (3-4 factors): 3-4 agents
-
Postoperative Ileus
- Prevention bundle: Early feeding, gum chewing, mobilization, opioid minimization
- Monitoring: Flatus passage, bowel sounds, abdominal distension
- Intervention thresholds: No flatus >48 hours or clinical symptoms
-
Venous Thromboembolism
- Risk stratification: Caprini score or institutional protocol
- Mechanical prophylaxis: Sequential compression devices
- Chemical prophylaxis: Based on bleeding risk assessment
Recovery Milestone Tracking System:
| Time Point | Expected Milestones | Red Flags | Intervention Triggers |
|---|---|---|---|
| 0-4 hours | Awake, pain <4/10, minimal nausea | Uncontrolled pain, persistent nausea, hemodynamic instability | Analgesic adjustment, antiemetic therapy, fluid resuscitation |
| 4-12 hours | Sitting up, sipping fluids, voiding | Unable to sit, persistent NPO, urinary retention | Physical therapy, bladder scan, catheter consideration |
| 12-24 hours | Walking >100 feet, tolerating diet, pain controlled | Bedbound, unable to eat, severe pain | Mobility assessment, nutrition consult, pain team |
| 24-48 hours | Independent ambulation, regular diet, discharge planning | Assistance required, diet intolerance, new symptoms | Extended stay planning, complication workup |
| %%{init: {'flowchart': {'htmlLabels': true}}}%% | |||
| flowchart TD |
Assess["📋 Patient Assessment
• Initial evaluation• Pre-op screening"]
Score{"📋 Risk Score
• Stratify patient• Clinical metrics"}
Std["💊 Standard ERAS
• Routine pathway• Standard care"]
StdDetail["📋 Full Protocol
• 18-22 Elements• Comprehensive care"]
Enh["💊 Enhanced ERAS
• Moderate risk• Tailored approach"]
EnhDetail["📋 Selected Protocol
• 15-18 Elements• Targeted items"]
Mod["💊 Modified ERAS
• High risk cases• Limited protocol"]
ModDetail["📋 Safety Protocol
• 10-15 Elements• Safety focused"]
Mile{"📋 24h Milestones
• Check progress• Post-op day 1"}
Cont["💊 Continue Protocol
• Maintain course• Stable recovery"]
Esc["⚠️ Escalate Care
• Clinical review• High intensity"]
Disc["✅ Discharge Planning
• Home preparation• Final review"]
RCA["👁️ Root Cause Analysis
• Identify gaps• Process review"]
Assess --> Score Score -->|0-2 Low| Std Score -->|3-5 Moderate| Enh Score -->|6+ High| Mod
Std --> StdDetail Enh --> EnhDetail Mod --> ModDetail
StdDetail --> Mile EnhDetail --> Mile ModDetail --> Mile
Mile -->|Met| Cont Mile -->|Missed| Esc
Cont --> Disc Esc --> RCA
style Assess fill:#FEF8EC, stroke:#FBECCA, stroke-width:1.5px, rx:12, ry:12, color:#854D0E style Score fill:#FEF8EC, stroke:#FBECCA, stroke-width:1.5px, rx:12, ry:12, color:#854D0E style Mile fill:#FEF8EC, stroke:#FBECCA, stroke-width:1.5px, rx:12, ry:12, color:#854D0E
style Std fill:#F1FCF5, stroke:#BEF4D8, stroke-width:1.5px, rx:12, ry:12, color:#166534 style Enh fill:#F1FCF5, stroke:#BEF4D8, stroke-width:1.5px, rx:12, ry:12, color:#166534 style Mod fill:#F1FCF5, stroke:#BEF4D8, stroke-width:1.5px, rx:12, ry:12, color:#166534 style Cont fill:#F1FCF5, stroke:#BEF4D8, stroke-width:1.5px, rx:12, ry:12, color:#166534
style StdDetail fill:#FEF8EC, stroke:#FBECCA, stroke-width:1.5px, rx:12, ry:12, color:#854D0E style EnhDetail fill:#FEF8EC, stroke:#FBECCA, stroke-width:1.5px, rx:12, ry:12, color:#854D0E style ModDetail fill:#FEF8EC, stroke:#FBECCA, stroke-width:1.5px, rx:12, ry:12, color:#854D0E
style Esc fill:#FDF4F3, stroke:#FCE6E4, stroke-width:1.5px, rx:12, ry:12, color:#B91C1C style Disc fill:#F6F5F5, stroke:#E7E6E6, stroke-width:1.5px, rx:12, ry:12, color:#525252 style RCA fill:#EEFAFF, stroke:#DAF3FF, stroke-width:1.5px, rx:12, ry:12, color:#0369A1
**ERAS Quality Metrics Dashboard**:
- **Protocol adherence**: **Target >85%** across all elements
- **Length of stay**: **Benchmark against historical** and **peer data**
- **Complication rates**: **Track major** and **minor complications**
- **Readmission rates**: **30-day unplanned** returns
- **Patient satisfaction**: **HCAHPS scores** and **ERAS-specific surveys**
- **Cost per case**: **Direct** and **indirect** cost analysis
- **Staff satisfaction**: **Workflow efficiency** and **job satisfaction**
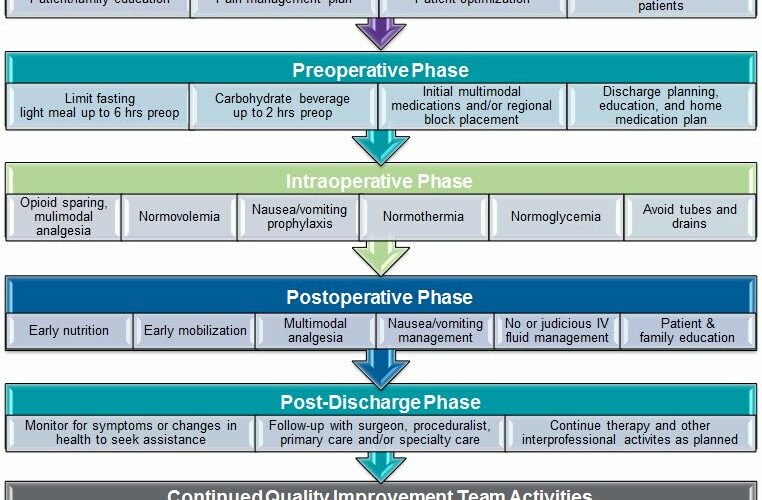
This comprehensive mastery toolkit provides the essential framework for immediate implementation of evidence-based ERAS protocols that consistently deliver superior patient outcomes across diverse surgical populations.
🎯 Clinical Mastery Arsenal: The Rapid Reference Toolkit
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for NEET-PG prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app
























