Critical Care Medicine

On this page
🚨 Critical Care Medicine: The Life-Support Command Center
Critical care medicine transforms you into a physiologic detective and engineer, managing the razor-thin margin between life and death when multiple organ systems fail simultaneously. You'll master hemodynamic monitoring to decode cardiovascular collapse, engineer precise respiratory support when lungs can't sustain oxygenation, recognize the four shock patterns before irreversible damage occurs, and orchestrate fluid resuscitation and metabolic interventions that restore cellular function. This integrated command of life-support systems separates clinicians who react from those who anticipate, stabilize, and save lives in medicine's highest-stakes environment.
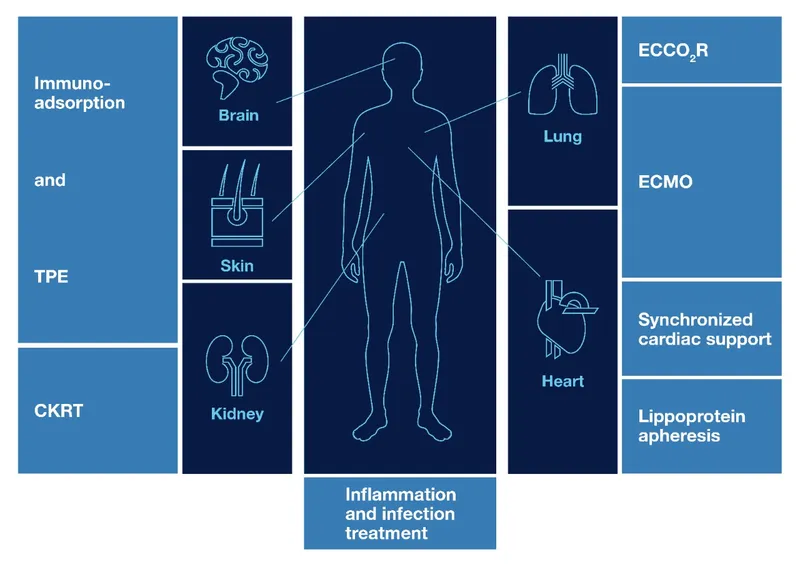
The Multi-System Integration Framework
Critical care medicine operates on the principle that organ systems are interconnected, and failure in one system rapidly cascades to others. The "golden hour" concept extends to "golden minutes" in ICU settings, where interventions must be initiated within 15-20 minutes of recognition.
-
Cardiovascular System
- Mean arterial pressure (MAP) target: 65-70 mmHg minimum
- Cardiac index normal range: 2.5-4.0 L/min/m²
- Central venous pressure: 8-12 mmHg optimal range
- Preload assessment through dynamic parameters
- Stroke volume variation <13% indicates adequate filling
- Pulse pressure variation <13% suggests euvolemia
-
Respiratory System
- Oxygen delivery (DO₂): 500-600 mL/min/m² normal
- Oxygen consumption (VO₂): 120-160 mL/min/m² baseline
- P/F ratio <300 indicates acute lung injury
- P/F ratio <200 defines ARDS
- Driving pressure <15 cmH₂O reduces mortality
- PEEP optimization maintains 90-95% oxygen saturation
📌 Remember: SOFA (Sequential Organ Failure Assessment) - Six systems, Organ dysfunction, Failure assessment, Acute scoring. Each point increase correlates with 15-20% mortality increase.
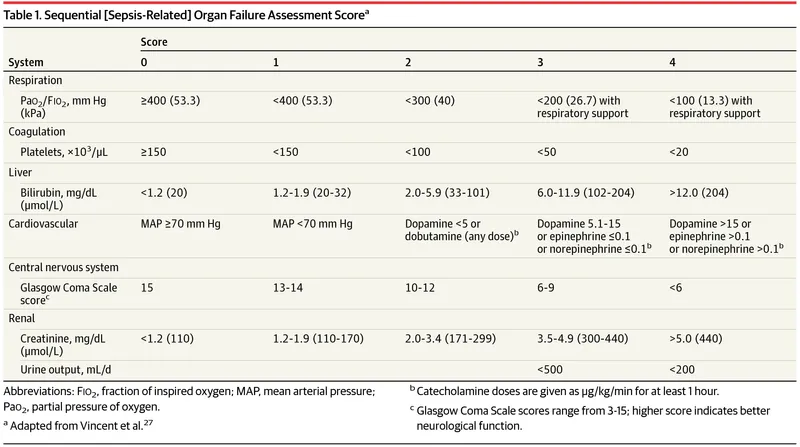
Hemodynamic Monitoring Hierarchy
| Parameter | Normal Range | Critical Threshold | Intervention Point | Mortality Risk |
|---|---|---|---|---|
| MAP | 70-100 mmHg | <65 mmHg | <60 mmHg | 25% increase |
| CVP | 2-8 mmHg | >15 mmHg | >20 mmHg | 40% increase |
| PCWP | 6-12 mmHg | >18 mmHg | >25 mmHg | 35% increase |
| Cardiac Index | 2.5-4.0 L/min/m² | <2.2 L/min/m² | <1.8 L/min/m² | 50% increase |
| SVR | 800-1200 dynes | >1500 dynes | >2000 dynes | 30% increase |
The Critical Care Cascade
💡 Master This: The "ABCDE" approach in critical care requires simultaneous assessment, not sequential. Cardiovascular collapse can occur within 2-3 minutes of respiratory failure, demanding parallel interventions.
Understanding these foundational principles establishes the framework for advanced hemodynamic monitoring techniques that enable precise cardiovascular assessment and intervention.
🚨 Critical Care Medicine: The Life-Support Command Center
🔄 Hemodynamic Monitoring: The Cardiovascular Detective System
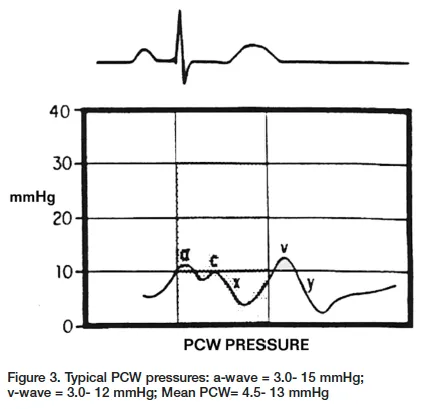
Advanced Hemodynamic Parameters
The evolution from basic vital signs to comprehensive hemodynamic profiling represents a paradigm shift in critical care. Functional hemodynamics assess cardiovascular reserve and fluid responsiveness, while static parameters provide baseline measurements.
-
Preload Assessment
- Central venous pressure: 8-12 mmHg target range
- Pulmonary capillary wedge pressure: 8-15 mmHg optimal
- Right ventricular end-diastolic volume index: 60-100 mL/m²
- Global end-diastolic volume index: 680-800 mL/m²
- Intrathoracic blood volume index: 850-1000 mL/m²
- Stroke volume variation: <13% indicates adequate preload
-
Afterload Quantification
- Systemic vascular resistance: 800-1200 dynes·sec/cm⁵
- Pulmonary vascular resistance: 150-250 dynes·sec/cm⁵
- Left ventricular stroke work index: 35-85 g·m/m²
- Right ventricular stroke work index: 4-8 g·m/m²
- Arterial elastance: 1.5-2.5 mmHg/mL
- Ventricular-arterial coupling ratio: 0.6-1.2 optimal
📌 Remember: FRANK-STARLING mechanism - Force increases, Range optimal, Afterload affects, Normal curve, Key preload, Stroke volume, Tension relationship, Augmented contractility, Reserve capacity, Length-tension, Inotropic state, Neurohormonal, Gradient pressure. Ventricular function curves shift with 15-20% contractility changes.
Dynamic Hemodynamic Assessment
| Monitoring Method | Parameter | Normal Value | Fluid Responsive | Accuracy |
|---|---|---|---|---|
| Arterial Line | SVV | <13% | >13% | 85% |
| Arterial Line | PPV | <13% | >13% | 84% |
| Echocardiography | IVC Variation | <50% | >50% | 82% |
| Thermodilution | GEDI | 680-800 mL/m² | <680 mL/m² | 78% |
| Pulse Contour | dPmax | <2 mmHg | >2 mmHg | 76% |
⭐ Clinical Pearl: Fluid responsiveness occurs in only 50% of critically ill patients. Passive leg raise test predicts fluid responsiveness with 89% sensitivity and 91% specificity, avoiding unnecessary fluid administration.
💡 Master This: Ventricular-arterial coupling optimization requires matching cardiac contractility to afterload. Optimal coupling ratio of 0.6-1.2 maximizes stroke work efficiency and reduces myocardial oxygen consumption by 20-30%.
These hemodynamic principles provide the foundation for understanding respiratory failure patterns and mechanical ventilation strategies that support cardiovascular function.
🔄 Hemodynamic Monitoring: The Cardiovascular Detective System
🫁 Respiratory Support: The Oxygenation Engineering System
Mechanical Ventilation Fundamentals
Modern mechanical ventilation balances adequate gas exchange with lung protection, utilizing low tidal volume strategies and optimal PEEP to minimize barotrauma and volutrauma. The "baby lung" concept in ARDS recognizes that only 20-30% of lung tissue remains functional.
-
Ventilation Parameters
- Tidal volume: 6-8 mL/kg predicted body weight
- Respiratory rate: 12-20 breaths/min baseline
- PEEP: 5-15 cmH₂O individualized optimization
- Driving pressure: <15 cmH₂O mortality benefit
- Plateau pressure: <30 cmH₂O safety threshold
- Mean airway pressure: <25 cmH₂O hemodynamic consideration
-
Oxygenation Targets
- PaO₂: 60-80 mmHg adequate range
- SpO₂: 88-95% conservative target
- P/F ratio: >200 normal, <200 ARDS definition
- Oxygenation index: <25 mild, >40 severe
- A-a gradient: <15 mmHg normal on room air
- Shunt fraction: <15% physiologic, >30% pathologic
📌 Remember: ARDS-NET protocol - Acute lung injury, Respiratory distress, Damage limitation, Six mL/kg tidal volume, Net benefit proven, Evidence-based, Tidal volume reduction. Mortality reduction of 22% with lung-protective ventilation.
Ventilator Mode Selection Strategy
| Clinical Scenario | Preferred Mode | Tidal Volume | PEEP | FiO₂ Strategy |
|---|---|---|---|---|
| ARDS | Volume Control | 6 mL/kg PBW | 10-15 cmH₂O | Minimize <60% |
| COPD Exacerbation | Pressure Support | 8-10 mL/kg | 5-8 cmH₂O | Target SpO₂ 88-92% |
| Cardiogenic Shock | SIMV + PS | 6-8 mL/kg | 8-12 cmH₂O | Optimize DO₂ |
| Neuromuscular | Volume Control | 8-10 mL/kg | 5-8 cmH₂O | Normal targets |
| Post-operative | Pressure Support | 8-10 mL/kg | 5-10 cmH₂O | Liberal oxygenation |
⭐ Clinical Pearl: Spontaneous breathing trials using T-piece or pressure support ≤7 cmH₂O for 30-120 minutes predict extubation success with 85% accuracy. Rapid shallow breathing index >105 predicts weaning failure.
💡 Master This: Ventilator-induced lung injury occurs through volutrauma (overdistension), barotrauma (pressure), atelectrauma (recruitment/derecruitment), and biotrauma (inflammatory mediators). Driving pressure <15 cmH₂O reduces mortality regardless of PEEP or tidal volume.
Understanding respiratory support principles enables recognition of shock states and implementation of appropriate hemodynamic interventions.
🫁 Respiratory Support: The Oxygenation Engineering System
🩸 Shock Recognition: The Circulatory Crisis Detection Matrix
Shock Classification Matrix
The four primary shock categories demonstrate distinct hemodynamic profiles, requiring different therapeutic approaches. Early recognition within 60 minutes of onset significantly improves survival, with each hour delay increasing mortality by 7-10%.
-
Hypovolemic Shock
- Cardiac output: ↓↓ (severely reduced)
- Systemic vascular resistance: ↑↑ (compensatory vasoconstriction)
- Central venous pressure: ↓ (<5 mmHg)
- Stroke volume variation: >15% fluid responsive
- Pulse pressure variation: >13% volume depletion
- Lactate elevation: >2 mmol/L tissue hypoperfusion
-
Cardiogenic Shock
- Cardiac output: ↓↓ (pump failure)
- Systemic vascular resistance: ↑ (compensatory)
- Central venous pressure: ↑↑ (>15 mmHg)
- Pulmonary capillary wedge pressure: >18 mmHg
- Cardiac index: <2.2 L/min/m²
- Mixed venous oxygen saturation: <65%
📌 Remember: SHOCK mnemonic - Systolic BP <90, Heart rate >100, Organ dysfunction, Cold extremities, Kidney injury (oliguria <0.5 mL/kg/h). Mortality increases 15% for each organ system involved.
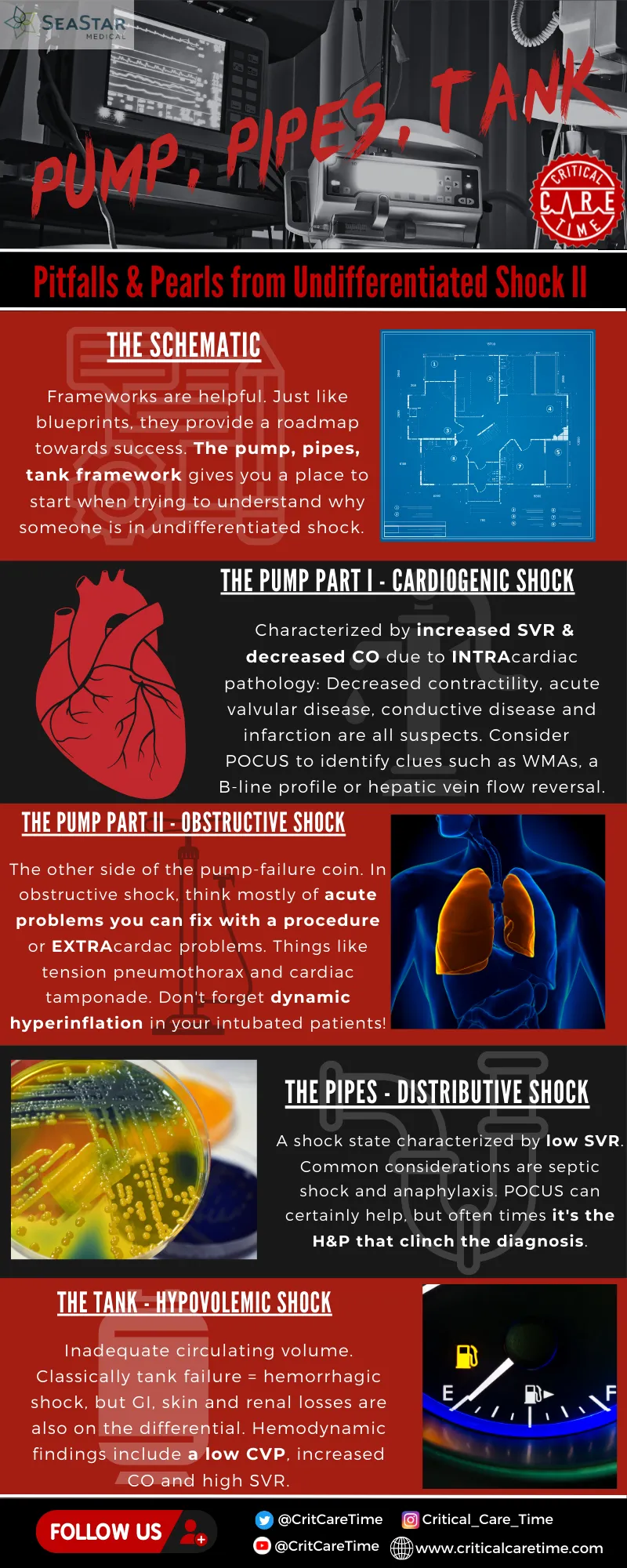
Advanced Shock Differentiation
| Shock Type | CO | SVR | CVP | PCWP | ScvO₂ | Lactate | Mortality |
|---|---|---|---|---|---|---|---|
| Hypovolemic | ↓↓ | ↑↑ | ↓ | ↓ | ↓ | ↑ | 20-30% |
| Cardiogenic | ↓↓ | ↑ | ↑↑ | ↑↑ | ↓↓ | ↑↑ | 40-50% |
| Distributive | ↑/N | ↓↓ | ↓/N | ↓/N | ↑/N | ↑ | 25-35% |
| Obstructive | ↓↓ | ↑ | ↑↑ | ↓/↑ | ↓ | ↑ | 30-60% |
| Mixed | Variable | Variable | Variable | Variable | ↓ | ↑↑ | 50-70% |
⭐ Clinical Pearl: Cryptic shock (elevated lactate >2 mmol/L with normal blood pressure) occurs in 8-10% of emergency department patients and carries 15% mortality if untreated. Early recognition and resuscitation reduce mortality to 5%.
💡 Master This: Distributive shock encompasses septic, anaphylactic, and neurogenic etiologies. Septic shock requires mean arterial pressure ≥65 mmHg and lactate >2 mmol/L despite adequate fluid resuscitation. Norepinephrine is first-line vasopressor with mortality benefit over dopamine.
These shock recognition principles integrate with fluid and electrolyte management strategies to optimize cellular perfusion and metabolic function.
🩸 Shock Recognition: The Circulatory Crisis Detection Matrix
⚖️ Fluid and Electrolyte Optimization: The Cellular Environment Control System
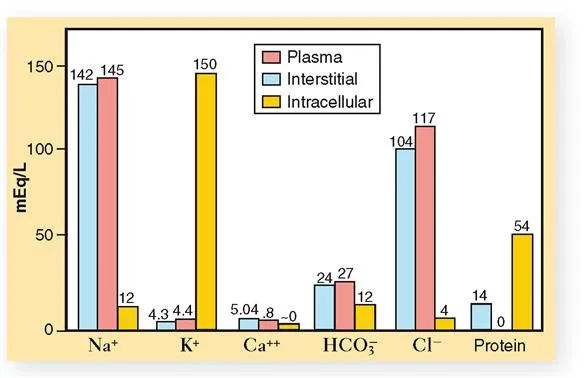
Fluid Compartment Physiology
The human body contains approximately 60% water by weight, distributed across intracellular (40%) and extracellular (20%) compartments. Critical illness disrupts normal fluid distribution through capillary leak, altered oncotic pressure, and hormonal dysregulation.
-
Intracellular Fluid (ICF)
- Volume: 28 L in 70-kg adult
- Primary cation: Potassium (140 mEq/L)
- Primary anion: Phosphate and proteins
- Osmolality: 280-295 mOsm/kg maintained
- Na⁺-K⁺-ATPase pump maintains gradients
- Cell membrane integrity crucial for distribution
-
Extracellular Fluid (ECF)
- Intravascular volume: 3.5 L (plasma)
- Interstitial volume: 10.5 L (tissue fluid)
- Primary cation: Sodium (140 mEq/L)
- Chloride: 100-105 mEq/L primary anion
- Albumin: 3.5-5.0 g/dL oncotic pressure
- Colloid osmotic pressure: 25-28 mmHg
📌 Remember: FLUID compartments - Forty percent ICF, Large interstitial space, Uniform osmolality, Intravascular 5%, Distribution depends on Starling forces. Capillary leak in sepsis increases interstitial volume by 30-50%.
Intravenous Fluid Selection Strategy
| Fluid Type | Osmolality | Na⁺ | Cl⁻ | K⁺ | Lactate | Clinical Use |
|---|---|---|---|---|---|---|
| Normal Saline | 308 | 154 | 154 | 0 | 0 | Volume expansion |
| Lactated Ringers | 273 | 130 | 109 | 4 | 28 | Balanced replacement |
| Plasmalyte | 294 | 140 | 98 | 5 | 0 | Physiologic balance |
| 5% Albumin | 290 | 145 | 145 | 0 | 0 | Oncotic support |
| Hypertonic Saline | 1026 | 513 | 513 | 0 | 0 | Cerebral edema |
⭐ Clinical Pearl: Balanced crystalloids (Lactated Ringers, Plasmalyte) reduce acute kidney injury by 15% and mortality by 11% compared to normal saline in critically ill patients. Chloride load from normal saline causes hyperchloremic acidosis.
💡 Master This: Stewart approach to acid-base disorders focuses on strong ion difference (SID), total weak acids (Atot), and PCO₂. Normal SID is 40-42 mEq/L. Decreased SID causes acidosis, increased SID causes alkalosis, independent of bicarbonate levels.
Understanding fluid and electrolyte principles enables integration with nutritional support strategies that optimize metabolic recovery and organ function.
⚖️ Fluid and Electrolyte Optimization: The Cellular Environment Control System
🧬 Metabolic Support Integration: The Cellular Fuel Optimization Network
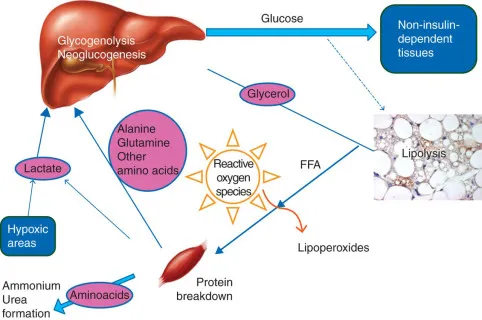
Critical Illness Metabolic Response
Critical illness triggers a hypermetabolic state with increased energy expenditure (25-50% above baseline), protein catabolism (1.5-2.0 g/kg/day muscle loss), and altered substrate utilization. The acute phase response prioritizes survival over growth and repair.
-
Metabolic Alterations
- Resting energy expenditure: ↑25-50% above predicted
- Protein catabolism: 1.5-2.0 g/kg/day muscle breakdown
- Glucose production: ↑200-300% hepatic gluconeogenesis
- Insulin resistance: 3-5 fold increase in requirements
- Lipolysis: ↑150-200% free fatty acid mobilization
- Negative nitrogen balance: 15-20 g/day protein loss
-
Nutritional Requirements
- Energy: 25-30 kcal/kg/day actual body weight
- Protein: 1.2-2.0 g/kg/day depending on severity
- Carbohydrate: 4-5 mg/kg/min glucose infusion rate
- Fat: 1.0-1.5 g/kg/day essential fatty acids
- Glutamine: 0.3-0.5 g/kg/day conditionally essential
- Arginine: 10-15 g/day immune function support
📌 Remember: NUTRITION priorities - Nitrogen balance, Utilization optimization, Timing early, Route enteral preferred, Immune function, Tolerance monitoring, Insulin management, Outcome improvement, Needs assessment. Early nutrition within 24-48 hours reduces complications by 30%.
Nutrition Delivery Strategy Matrix
| Clinical Scenario | Route | Timing | Energy Target | Protein Target | Special Considerations |
|---|---|---|---|---|---|
| Post-operative | Enteral | <24h | 25-30 kcal/kg | 1.2-1.5 g/kg | Early mobilization |
| ARDS/ECMO | Enteral | <48h | 15-20 kcal/kg | 1.3-1.8 g/kg | Hypocaloric feeding |
| Renal Failure | Mixed | <24h | 25-35 kcal/kg | 1.2-1.7 g/kg | Phosphorus restriction |
| Liver Failure | Enteral | <24h | 30-35 kcal/kg | 1.2-1.5 g/kg | BCAA supplementation |
| Burns >20% | Enteral | <6h | 35-40 kcal/kg | 2.0-2.5 g/kg | High calorie density |
⭐ Clinical Pearl: Enteral nutrition maintains gut barrier function and reduces infectious complications by 25-30% compared to parenteral nutrition. Trophic feeding (10-20 mL/h) provides gut protection even when full nutrition isn't tolerated.
💡 Master This: Refeeding syndrome occurs in malnourished patients when nutrition is restarted, causing phosphorus <2.5 mg/dL, potassium <3.5 mEq/L, and magnesium <1.8 mg/dL. Thiamine deficiency can cause cardiac dysfunction and neurologic complications. Start nutrition at 50% of goal in high-risk patients.
These metabolic support principles integrate with comprehensive critical care management to optimize patient outcomes and facilitate recovery from multi-organ dysfunction.
🧬 Metabolic Support Integration: The Cellular Fuel Optimization Network
🎯 Critical Care Mastery: The Life-Support Command Arsenal
The Critical Care Essential Arsenal
📌 Remember: CRITICAL assessment - Cardiovascular stability, Respiratory adequacy, Infection control, Tissue perfusion, Intracranial pressure, Coagulation status, Acid-base balance, Liver function. Systematic evaluation prevents missed diagnoses and guides prioritization.
| System | Key Parameter | Normal Range | Critical Threshold | Intervention |
|---|---|---|---|---|
| Cardiovascular | MAP | 70-100 mmHg | <65 mmHg | Vasopressors |
| Respiratory | P/F Ratio | >400 | <200 | Lung protection |
| Renal | Creatinine | 0.7-1.3 mg/dL | >2.0 mg/dL | RRT consideration |
| Neurologic | ICP | <15 mmHg | >20 mmHg | Neuroprotection |
| Metabolic | Lactate | <2 mmol/L | >4 mmol/L | Resuscitation |
⭐ Clinical Pearl: Goal-directed therapy targeting ScvO₂ >70%, lactate clearance >10%, and MAP ≥65 mmHg reduces sepsis mortality by 16%. Early recognition and protocol-driven care improve outcomes across all critical care conditions.
💡 Master This: Multi-organ dysfunction syndrome (MODS) develops when ≥2 organ systems fail simultaneously. Each additional organ failure increases mortality by 15-20%. Early intervention within the "golden hour" prevents cascade failure and improves survival.
Understanding these integrated critical care principles transforms theoretical knowledge into life-saving clinical expertise, enabling rapid recognition and management of complex multi-system pathophysiology.
🎯 Critical Care Mastery: The Life-Support Command Arsenal
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for NEET-PG prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app
























