OSA Fundamentals - Snore Wars Saga
- OSA: Recurrent upper airway obstruction during sleep, causing intermittent hypoxemia & sleep fragmentation.
- Pathophysiology: Anatomical compromise (e.g., macroglossia, tonsillar hypertrophy, obesity) & ↓ pharyngeal dilator muscle activity.
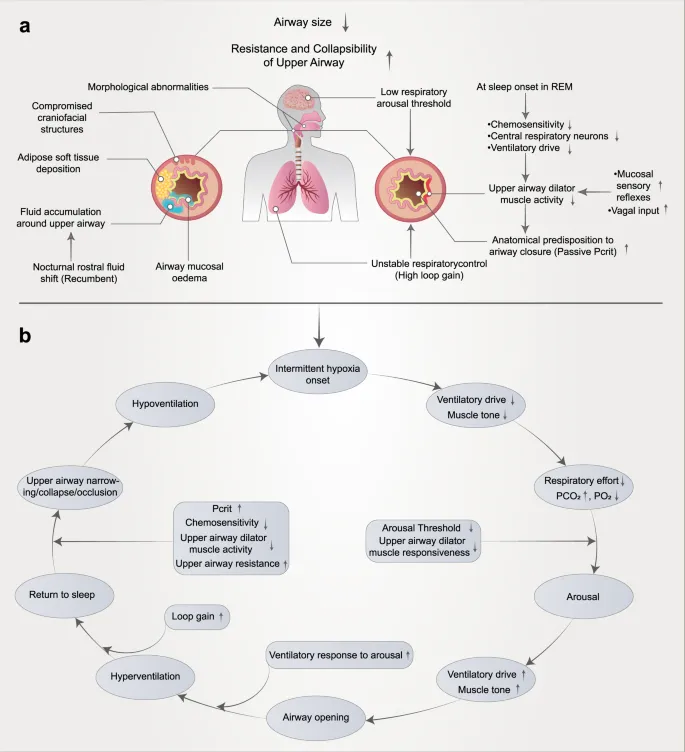
- Pathophysiology: Anatomical compromise (e.g., macroglossia, tonsillar hypertrophy, obesity) & ↓ pharyngeal dilator muscle activity.
- Key Metrics & Severity (AHI events/hr):
- Mild: 5-15
- Moderate: 15-30
- Severe: >30
⭐ Apnea: Cessation of airflow ≥10s. Hypopnea: ↓ airflow ≥30% for ≥10s with ≥3% O2 desaturation or arousal.
- Clinical: Loud snoring, witnessed apneas, daytime somnolence. ↑ Perioperative risks (difficult airway, hypoxemia).
Preoperative Screening - Spot the Sleeper
- Identify undiagnosed Obstructive Sleep Apnea (OSA) to reduce perioperative adverse events.
- 📌 STOP-BANG Questionnaire:
- Snoring, Tiredness, Observed apnea, high Pressure (BP)
- BMI > 35 kg/m², Age > 50 yrs, Neck circumference > 40cm, Gender Male.
- Risk Stratification:
- Score 0-2: Low risk. Proceed with standard perioperative care.
- Score 3-4: Intermediate risk. Increased vigilance; consider possibility of OSA.
- Score 5-8: High risk. High likelihood of OSA. For elective surgery, refer for Polysomnography (PSG) or Home Sleep Apnea Test (HSAT). For urgent surgery, manage as presumed OSA.
⭐ A high STOP-BANG score (≥3) indicates increased risk of moderate to severe OSA.
Intraoperative Management - Airway Vigilance
- Anticipate Difficult Airway: Thorough pre-op assessment (e.g., STOP-BANG).
- Equipment Ready: Standard + Difficult Airway Trolley.
- Laryngeal Mask Airway (LMA), Video Laryngoscope, Fiberoptic Bronchoscope.

- Laryngeal Mask Airway (LMA), Video Laryngoscope, Fiberoptic Bronchoscope.
- Induction & Maintenance:
- Rapid Sequence Intubation (RSI) if aspiration risk.
- Prefer volatile anesthetics; minimize long-acting opioids.
- Cautious opioid dosing; prioritize multimodal analgesia (e.g., NSAIDs, paracetamol).
- Positioning: Non-supine when feasible, especially post-extubation.
- Monitoring: Standard ASA monitors, continuous capnography, neuromuscular monitoring.
- Extubation Criteria: Fully awake, adequate muscle tone (TOF ratio > 0.9), follows commands, good respiratory effort.
⭐ Regional anesthesia is preferred whenever possible to minimize airway manipulation and respiratory depression in OSA patients during ambulatory surgery.
Postoperative Care - Recovery & Risks
- PACU Focus: Continuous SpO2, ECG. Non-supine positioning (lateral/semi-Fowler's).
- Oxygen & PAP: Maintain SpO2 >92%. Resume pre-op CPAP/BiPAP ASAP.
- Analgesia: Multimodal, opioid-sparing (e.g., regional, NSAIDs). Caution with systemic opioids.
- Key Risks: Postoperative desaturation, apnea/hypopnea, respiratory acidosis.
- Discharge Criteria (e.g., Aldrete ≥9): Stable vitals, pain controlled, no significant desaturation (<90%) for >1 hour (extended monitoring may be needed).
⭐ Patients with OSA are at high risk for postoperative desaturation and respiratory events; continuous monitoring and non-supine positioning are crucial.
Postoperative algorithm:
High‑Yield Points - ⚡ Biggest Takeaways
- STOP-BANG score (≥3) is vital for preoperative OSA risk assessment.
- OSA significantly ↑ risk of postoperative respiratory compromise (hypoxemia, apnea).
- Regional anesthesia is preferred; minimizes airway manipulation and opioid use.
- For GA: prioritize short-acting agents; avoid/minimize long-acting opioids and sedatives.
- Extubate fully awake, in a non-supine position; ensure adequate PACU recovery.
- Resume patient's home CPAP/BiPAP as early as possible postoperatively.
- Strict discharge criteria: stable oxygenation on room air, no recent desaturation/apnea events before discharge from ambulatory facility.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

