Fast-Track Fundamentals - Speedy Recovery Roadmap
Fast-Track Recovery, or Enhanced Recovery After Surgery (ERAS), applies evidence-based, multimodal strategies in ambulatory surgery. It's a patient-centered, interdisciplinary team approach optimizing the perioperative journey.
- Primary Objective: Expedite recovery, reduce physiological stress, improve patient experience.
- Key Goals Achieved:
- Significantly ↓ Length Of Stay (LOS)
- ↓ Postoperative morbidity & complications
- ↓ Healthcare costs
- ↑ Patient satisfaction scores
- Quicker return to normal daily activities
- 📌 ERAS: Early feeding, Removing drains/catheters, Analgesia (multimodal), Structured discharge.
⭐ Fast-track protocols aim to attenuate the surgical stress response.
Pre-Op Prep - Setting the Stage
- Patient Selection Criteria:
- ASA physical status I or II.
- Motivated patient with good understanding.
- Surgical procedure suitable for ambulatory setting.
- Adequate post-discharge home support.
- Body Mass Index (BMI) < 35-40 kg/m².
- Core Pre-Op Interventions:
- Comprehensive preoperative patient education and counseling.
- Optimized Nutrition: Carbohydrate loading 2-3 hours pre-op (e.g., 400ml of 12.5% CHO drink).
- Fasting Guidelines: Clear fluids up to 2 hours pre-op, solids 6 hours pre-op (📌 '2-6 rule').
- Smoking and alcohol cessation advice.
- Anxiolysis: Short-acting benzodiazepines if clinically indicated, or non-pharmacological methods.
- Pre-emptive Multimodal Analgesia: E.g., paracetamol, NSAIDs (celecoxib), gabapentinoids.
⭐ Preoperative carbohydrate loading is a key ERAS component; it reduces postoperative insulin resistance and improves overall patient well-being.
In-Theatre Tactics - Smooth Sailing Surgery
- Anesthesia Choice:
- Preference: Regional (PNBs, neuraxial) for ↓opioids.
- GA (if required): Short-acting agents (Propofol, Desflurane, Sevoflurane, Remifentanil).
- Analgesia Strategy: Opioid-sparing or opioid-free.
- Multimodal: Combine non-opioid analgesics.
- Key adjuncts: Ketamine, Lidocaine IV, Dexmedetomidine.
- PONV Prophylaxis (📌 APFEL score for risk assessment):
- Moderate-high risk: Minimum 2 antiemetics.
- Examples: Dexamethasone 4-8mg (after induction), Ondansetron 4mg (at surgery end), Aprepitant.
- Fluid Therapy: Restrictive or goal-directed.
- Aim: <2-3L crystalloids; avoid overload.
- Normothermia: Crucial; use active warming measures.
⭐ Regional anesthesia is key in fast-track protocols, significantly cutting opioid use and side effects.
Post-Op & Parting - Swift Send-Off
- Analgesia: Effective multimodal, opioid-sparing strategies.
- Utilize: Paracetamol, NSAIDs, COX-2 inhibitors.
- Consider: Local anesthetic wound infiltration, peripheral nerve block catheters.
- Key Recovery Milestones:
- Early mobilization: Within hours of surgery.
- Early oral intake: Fluids as soon as tolerated, then light diet.
- Prompt urinary catheter removal.
- Manage PONV if it occurs effectively.
- Discharge Criteria: Standardized for patient safety.
- Post Anesthetic Discharge Scoring System (PADSS) score ≥9. 📌 VAP-S: Vital signs, Activity, Nausea/vomiting, Pain, Surgical bleeding.
- Aldrete score ≥9 also required.
- Patient Education: Essential for home care.
- Covering post-discharge care, home pain management, and follow-up instructions.
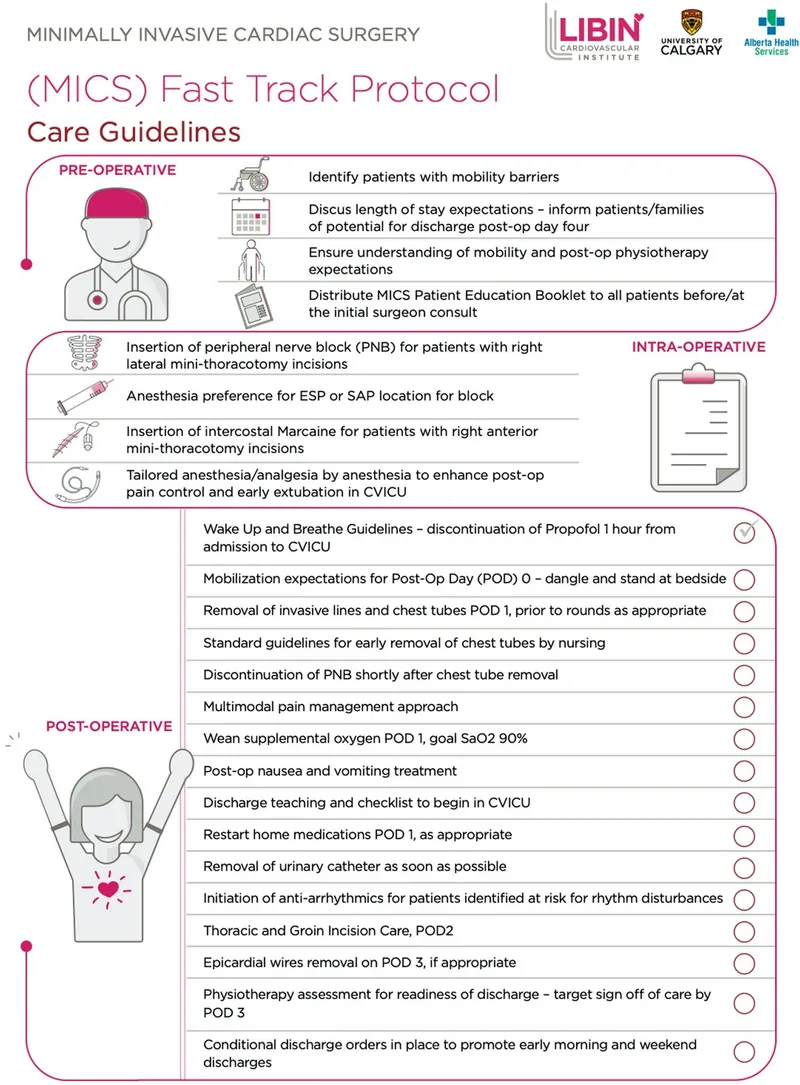
⭐ Early mobilization and early oral intake are pivotal in fast-track recovery, significantly reducing VTE risk and accelerating gut function restoration.
High‑Yield Points - ⚡ Biggest Takeaways
- Fast-track protocols aim for rapid recovery and early discharge in ambulatory surgery.
- Key components include multimodal analgesia, PONV prophylaxis, and early mobilization.
- Short-acting anesthetics (e.g., Propofol, Desflurane) and regional anesthesia are preferred.
- Opioid-sparing techniques are crucial to minimize side effects and hasten recovery.
- Discharge criteria are assessed using tools like the Post Anesthetic Discharge Scoring System (PADSS).
- Effective patient selection and preoperative education are vital for success.
- Benefits include reduced hospital stay, lower costs, and improved patient satisfaction.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

