Gait Cycle & Parameters - Steppin' Smart
- Gait Cycle: Initial contact (IC) of one foot to the next IC of the same foot.
- Stance Phase (~60%): Foot on ground. Sub-phases: IC (Heel Strike) → Loading Response (Foot Flat) → Midstance → Terminal Stance (Heel Off) → Preswing (Toe Off).
- Swing Phase (~40%): Foot in air. Sub-phases: Initial Swing → Midswing → Terminal Swing.
- Parameters:
- Stride Length: Distance of 1 gait cycle (avg. 1.4 m).
- Step Length: IC of one foot to IC of other foot (avg. 0.7 m).
- Cadence: Steps/minute (avg. 90-120).
- Walking Velocity: Speed (avg. 1.2-1.4 m/s).
- Base of Support: Lateral distance between feet (avg. 5-10 cm).
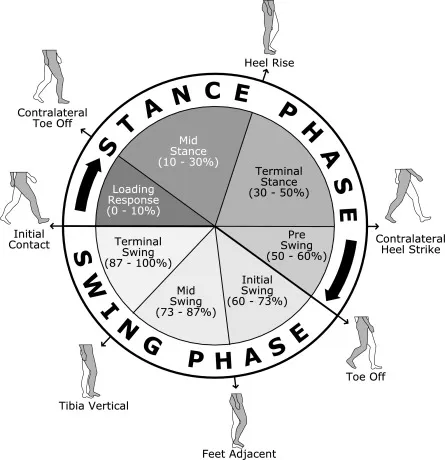
⭐ Double support (both feet on ground) occurs twice per gait cycle (start & end of stance), comprising ~20% of the cycle. It is absent in running.
Gait Kinematics & Kinetics - Joint Jive & Force Flow
- Kinematics (Motion): Joint angles & Center of Mass (COM) path.
- Hip: Sagittal range ~40° (Flexion 30° at IC, Extension 10° at TSt).
- Knee: Max flexion ~60° (ISw); near full extension at IC & MSt.
- Ankle: Dorsiflexion at IC; Plantarflexion for push-off (TSt).
- COM: Vertical displacement ~5 cm; Lateral ~4 cm.
- Kinetics (Forces): GRF, joint moments & power.
- Ground Reaction Force (GRF):
- Vertical: "M"-shape, peaks ~120% Body Weight (BW).
- Anterior-Posterior (AP): Braking (LR) then propulsive (TSt/PSw).
- Joint Moments: Internal muscle/ligament forces. e.g., Ankle plantarflexor moment.
- Joint Power: $P = M \cdot \omega$. Muscle work (generation/absorption).
- Ground Reaction Force (GRF):
⭐ The ankle plantarflexors (gastrocnemius, soleus) are the primary power generators for propulsion during late stance.
 oka
oka
Pathological Gaits - Wobble Wisdom
- Antalgic Gait: Pain-induced; ↓ stance phase on affected side. "Limping."
- Trendelenburg Gait: Gluteus medius weakness; pelvis drops on contralateral (swing) side.
- Positive Trendelenburg sign.
- Waddling Gait: Bilateral gluteus medius weakness; "duck-like" walk, lateral trunk sway.
- Steppage/Foot Drop Gait: Dorsiflexor weakness (e.g., common peroneal nerve palsy); high step to clear foot. Foot slap.
- Ataxic Gait: Cerebellar lesion; wide-based, unsteady, irregular steps. "Drunken" gait.
- Spastic (Hemiplegic) Gait: UMN lesion; affected leg stiff, extended; circumduction.
- Parkinsonian (Festinating) Gait: Stooped, short, shuffling steps (marche à petits pas), festination.
- Scissoring Gait: Bilateral spasticity (e.g., cerebral palsy); thighs cross, legs swing across midline.
⭐ Trendelenburg gait: weakness of hip abductors (gluteus medius/minimus) on the stance leg causes the pelvis to drop on the swing leg side.
Clinical Gait Assessment - Stride Sleuthing
- Observational Gait Analysis (OGA): Systematic visual check (anterior, posterior, lateral views).
- Parameters: Symmetry, step/stride length, cadence, base of support (BOS), arm swing, pelvic motion.
- Note deviations in stance (heel strike to toe-off) & swing phases.
- Key Standardized Tests:
- Timed Up and Go (TUG): Mobility & fall risk. >12-14 sec = ↑fall risk.
- Gait Speed: "6th vital sign". Normal: 1.2-1.4 m/s. <1.0 m/s = poor outcomes.
- 6-Minute Walk Test (6MWT): Functional capacity.
⭐ Trendelenburg gait (gluteus medius weakness): Pelvis drops on contralateral (swinging) side during stance phase of affected limb.
High‑Yield Points - ⚡ Biggest Takeaways
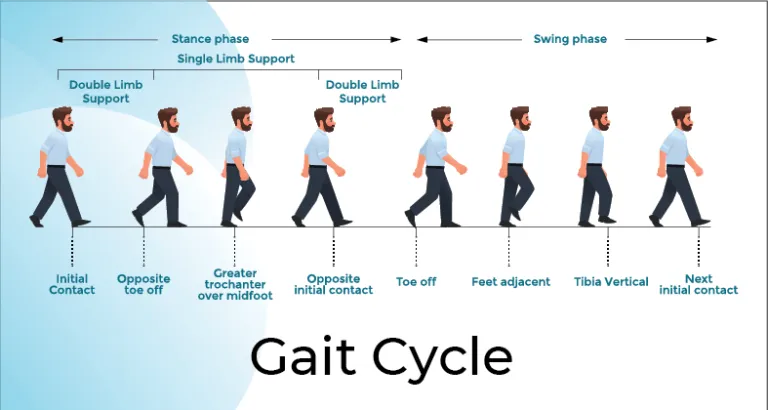
- Gait cycle comprises Stance phase (60%) and Swing phase (40%).
- Critical events: Heel strike, Foot flat, Midstance, Heel off, Toe off.
- Trendelenburg gait indicates gluteus medius weakness, causing contralateral pelvic drop.
- Foot drop (steppage gait) results from common peroneal nerve palsy.
- Center of Gravity (COG) shows ~5cm vertical and ~5cm lateral displacement.
- Double support (both feet on ground) occurs twice, crucial for stability.
- Antalgic gait is characterized by a shortened stance phase due to pain.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

