Lower Limb

On this page
🏗️ Lower Limb Architecture: The Engineering Marvel
The lower limb transforms abstract anatomy into clinical power-you'll master how bones, joints, and muscles create movement, then translate that architecture into diagnostic patterns that distinguish a meniscal tear from ligamentous injury at the bedside. This lesson builds your assessment from inspection through advanced maneuvers, sharpens your differential reasoning with evidence-based algorithms, and equips you with treatment frameworks that integrate orthopedics, rehabilitation, and surgical timing. You'll develop the pattern recognition that separates novice from expert, turning physical findings into precise diagnoses and actionable management plans.
Structural Hierarchy and Load Distribution
The lower limb's three-segment design creates optimal load transfer from the axial skeleton to ground contact:
-
Pelvic Girdle Foundation
- Hip joint: 120-130° angle of inclination
- Acetabular coverage: 40% of femoral head
- Weight transmission: bilateral 50% distribution
- Standing: 30% through hip joint
- Walking: 280% peak loading
- Running: 550% maximum forces
-
Thigh Segment (Femur)
- Length: 26% of total height
- Neck-shaft angle: 125-135° (normal range)
- Anteversion: 8-15° forward rotation
- Coxa vara: <120° pathological
- Coxa valga: >140° abnormal
-
Leg Segment (Tibia/Fibula)
- Tibial length: 22% of height
- Weight bearing: 85% tibia, 15% fibula
- Posterior slope: 7-10° tibial plateau
📌 Remember: HALT for hip angles - Hip inclination Angle Less Than 120° = coxa vara, greater than 140° = coxa valga
Compartmental Organization and Fascial Architecture
The lower limb's fascial compartment system creates 12 distinct compartments with specific neurovascular supplies and functional roles:
| Compartment | Primary Function | Key Muscles | Nerve Supply | Pressure Threshold |
|---|---|---|---|---|
| Anterior Thigh | Hip flexion, knee extension | Quadriceps, Sartorius | Femoral (L2-L4) | 30 mmHg |
| Medial Thigh | Hip adduction | Adductor group | Obturator (L2-L4) | 30 mmHg |
| Posterior Thigh | Hip extension, knee flexion | Hamstrings | Sciatic (L4-S3) | 30 mmHg |
| Anterior Leg | Dorsiflexion, inversion | Tibialis anterior, EDL | Deep peroneal | 30 mmHg |
| Lateral Leg | Eversion, plantarflexion | Peroneus longus/brevis | Superficial peroneal | 30 mmHg |
| Posterior Leg | Plantarflexion, inversion | Gastrocnemius, soleus | Tibial nerve | 30 mmHg |
Neurovascular Territory Mapping
The lower limb's dual nerve supply from lumbar (L1-L4) and sacral (L4-S4) plexuses creates predictable clinical patterns:
-
Lumbar Plexus Dominance (Anterior/Medial)
- Femoral nerve: L2-L4 roots
- Obturator nerve: L2-L4 roots
- Territory: anterior thigh, medial leg
- Motor: quadriceps, adductors
- Sensory: anteromedial thigh to medial malleolus
-
Sacral Plexus Control (Posterior/Lateral)
- Sciatic nerve: L4-S3 roots
- Superior/inferior gluteal: L4-S2
- Territory: posterior thigh, entire leg/foot
- Motor: hamstrings, all leg muscles
- Sensory: posterior thigh, lateral/plantar foot
💡 Master This: L4 nerve root contributes to both lumbar and sacral plexuses, explaining why L4 radiculopathy causes combined anterior weakness (quadriceps) and posterior weakness (tibialis anterior).
Joint Complexity and Movement Integration
The lower limb's 33 joints create 6 degrees of freedom at the hip, 2 degrees at the knee, and multiple axes at the ankle-foot complex:
-
Hip Joint Mechanics
- Range: 120° flexion, 30° extension
- Abduction: 45°, Adduction: 25°
- Rotation: 45° external, 35° internal
- Capsular pattern: flexion > abduction > internal rotation
-
Knee Joint Dynamics
- Flexion: 135° active, 160° passive
- Screw-home mechanism: 15° external tibial rotation
- Q-angle: 13° males, 18° females
- Pathological: >20° increases patellofemoral stress
-
Ankle-Foot Complex
- Dorsiflexion: 20°, Plantarflexion: 50°
- Inversion: 35°, Eversion: 15°
- Subtalar motion: triplanar movement patterns
📌 Remember: FIRE for hip capsular pattern - Flexion, Internal rotation, Rotation, Extension (most to least restricted)
Understanding this architectural foundation reveals how structural integrity determines functional capacity and predicts injury patterns. The next section explores how these static structures transform into dynamic movement systems through sophisticated muscle activation patterns.
🏗️ Lower Limb Architecture: The Engineering Marvel
⚡ Movement Powerhouse: The Muscular Command System
The lower limb's muscular architecture transforms static skeletal framework into dynamic locomotion through coordinated activation patterns that generate forces up to 8x body weight while maintaining precise postural control.
Power Generation and Force Transmission
The lower limb's muscle architecture creates three power zones with distinct force-velocity characteristics:
-
Hip Power Zone (Gluteal Complex)
- Peak torque: 280 Nm hip extension
- Power output: 400 watts during sprinting
- Activation timing: 0-15% gait cycle
- Gluteus maximus: 1,200 N maximum force
- Hip abductors: 800 N single-leg stance
- Contraction velocity: 6 rad/sec maximum
-
Knee Power Zone (Quadriceps/Hamstrings)
- Quadriceps strength: 3-4x body weight
- Hamstring ratio: 60-80% of quadriceps
- Eccentric capacity: 150% of concentric
- Vastus medialis: 15° fiber angle
- Rectus femoris: biarticular advantage
- Activation delay: 50-80 ms reflex response
-
Ankle Power Zone (Triceps Surae)
- Plantarflexor strength: 6-8x body weight
- Achilles tendon force: 4,000 N running
- Power contribution: 50% of propulsion
- Gastrocnemius: pennation angle 17°
- Soleus: slow-twitch 80% composition
- Elastic energy: 35% efficiency gain
⭐ Clinical Pearl: Hamstring-to-quadriceps ratio below 60% increases ACL injury risk by 300%, while ratios above 80% suggest quadriceps weakness requiring targeted strengthening.
Compartmental Synergy and Movement Patterns
The lower limb's compartmental organization creates predictable movement synergies through shared innervation and fascial connections:
| Movement Pattern | Primary Compartments | Synergist Activation | Force Ratios | Clinical Significance |
|---|---|---|---|---|
| Hip Flexion | Anterior thigh | Anterior leg (swing) | 3:1 hip:knee | L2-L4 nerve pattern |
| Hip Extension | Posterior thigh | Posterior leg (stance) | 2:1 glute:hamstring | L4-S3 nerve pattern |
| Knee Extension | Anterior thigh | Anterior leg (clear) | 4:1 quad:dorsiflexor | Femoral nerve dominance |
| Plantarflexion | Posterior leg | Posterior thigh (power) | 6:1 calf:hamstring | Tibial nerve control |
| Dorsiflexion | Anterior leg | Lateral leg (balance) | 1:2 TA:peroneal | Peroneal nerve supply |
Muscle Fiber Architecture and Performance
The lower limb's muscle fiber composition determines functional capacity and fatigue resistance:
-
Type I Fibers (Slow-Twitch Endurance)
- Soleus: 80-90% Type I composition
- Vastus intermedius: 70% Type I
- Function: postural control, endurance
- Oxidative capacity: high mitochondrial density
- Fatigue resistance: >60 minutes continuous
- Force generation: low peak, sustained
-
Type II Fibers (Fast-Twitch Power)
- Gastrocnemius: 60% Type II composition
- Vastus lateralis: 55% Type II
- Function: explosive power, rapid movement
- Glycolytic capacity: high enzyme activity
- Power output: 3x Type I force
- Fatigue onset: <2 minutes maximum effort
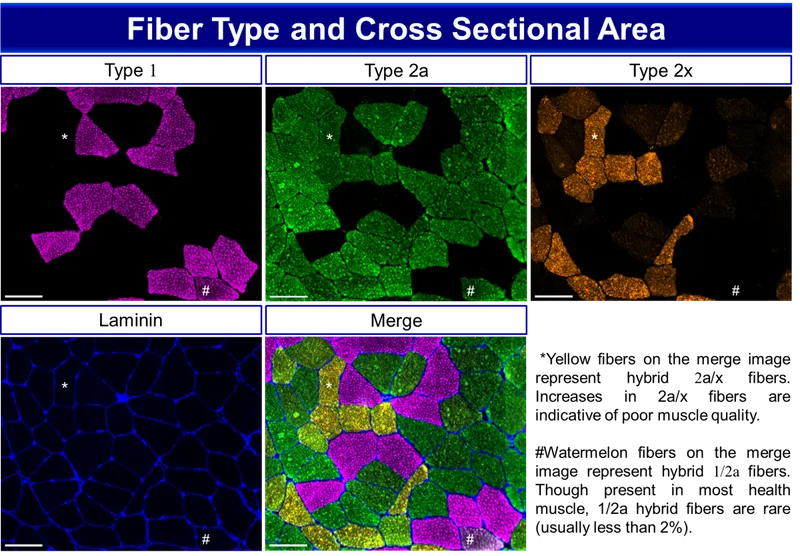
📌 Remember: SOFT for slow-twitch characteristics - Soleus dominant, Oxidative metabolism, Fatigue resistant, Tonic postural control
Neuromuscular Control and Activation Timing
The lower limb's motor control requires precise timing with millisecond coordination between antagonistic muscle groups:
-
Gait Cycle Activation Patterns
- Heel strike: quadriceps 100%, dorsiflexors 80%
- Loading response: gluteus maximus 90%, hamstrings 60%
- Mid-stance: soleus 100%, gluteus medius 80%
- Swing phase: hip flexors 100%, dorsiflexors 90%
- Double support: co-contraction 40% all groups
- Single support: abductors 100% maximum activation
-
Reflex Response Timing
- Stretch reflex: 30-50 ms monosynaptic
- Withdrawal reflex: 70-100 ms polysynaptic
- Postural responses: 100-150 ms complex
- Anticipatory control: 50-100 ms pre-activation
- Reactive control: 150-300 ms correction
- Adaptive control: >500 ms learning
⭐ Clinical Pearl: Delayed muscle activation (>150 ms) indicates neuromuscular dysfunction, increasing injury risk by 250% and requiring proprioceptive training for 6-8 weeks.
Understanding muscular command systems reveals how coordinated activation creates efficient movement while preventing injury. The next section examines how these movement patterns translate into clinical assessment and diagnostic frameworks.
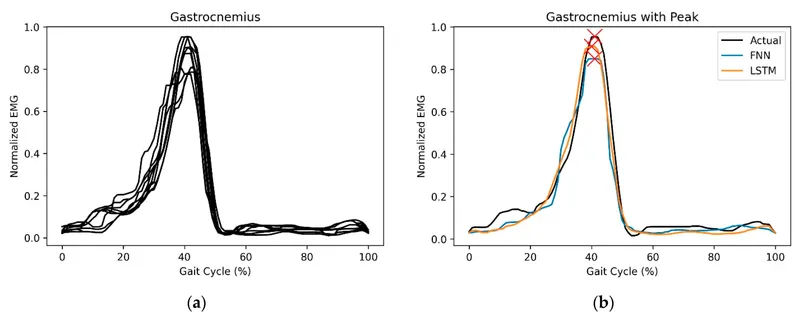
⚡ Movement Powerhouse: The Muscular Command System
🎯 Clinical Assessment Arsenal: Pattern Recognition Mastery
Systematic Inspection and Observation Patterns
The lower limb's visual assessment follows proximal-to-distal and anterior-posterior-lateral scanning patterns that detect >85% of significant pathology:
-
Static Postural Analysis
- Pelvic alignment: ASIS level ±5mm normal
- Q-angle measurement: 13° males, 18° females
- Leg length: <1cm discrepancy normal
- True length: ASIS to medial malleolus
- Apparent length: umbilicus to medial malleolus
- Functional assessment: standing alignment
-
Gait Pattern Recognition
- Stride length: 1.4x leg length normal
- Cadence: 110-120 steps/minute
- Stance phase: 60% of gait cycle
- Swing phase: 40% of cycle
- Double support: 20% of cycle
- Single support: 40% of cycle
-
Deformity Classification
- Varus/valgus: anatomical axis deviation
- Rotational: in-toeing/out-toeing >15°
- Length: >2cm discrepancy significant
- Antalgic: shortened stance phase
- Trendelenburg: pelvic drop >5°
- Circumduction: hip abduction compensation
📌 Remember: GALS screening - Gait, Arms, Legs, Spine assessment detects >90% of musculoskeletal pathology in <2 minutes
Palpation Techniques and Anatomical Landmarks
The lower limb's palpable landmarks provide precise localization for >150 clinically significant structures:
| Region | Key Landmarks | Clinical Significance | Normal Findings | Pathological Signs |
|---|---|---|---|---|
| Hip | Greater trochanter, ASIS | Bursitis, fracture | Non-tender, symmetric | Tenderness, swelling |
| Thigh | Adductor tubercle, patella | Muscle strain, tracking | Smooth contour | Mass, deformity |
| Knee | Joint line, tibial tuberosity | Meniscal tear, bursitis | <5mm joint space | Effusion, crepitus |
| Leg | Fibular head, malleoli | Nerve injury, fracture | Bony prominence | Step-off, tenderness |
| Foot | Navicular, 5th metatarsal | Arch collapse, fracture | Normal arch height | Flatfoot, pain |
Range of Motion Assessment and Functional Testing
The lower limb's ROM evaluation requires standardized positioning and goniometric measurement with ±5° accuracy:
-
Hip ROM Standards
- Flexion: 120° (knee flexed), 90° (knee extended)
- Extension: 30° prone position
- Abduction: 45° supine, pelvis stabilized
- Adduction: 25° across midline
- Internal rotation: 35° (90° hip flexion)
- External rotation: 45° (90° hip flexion)
-
Knee ROM Parameters
- Flexion: 135° active, 160° passive
- Extension: 0° normal, -5° hyperextension
- Rotation: 20° external, 10° internal
- Capsular pattern: flexion > extension
- End-feel: soft tissue flexion, bony extension
- Ligamentous laxity: >5mm translation abnormal
-
Ankle-Foot Complex
- Dorsiflexion: 20° (knee extended), 30° (knee flexed)
- Plantarflexion: 50° maximum range
- Inversion: 35° subtalar motion
- Eversion: 15° subtalar motion
- Forefoot: adduction/abduction 20°
- Hallux: dorsiflexion 65°, plantarflexion 45°
💡 Master This: Capsular pattern indicates arthritis or capsular restriction, while non-capsular pattern suggests ligamentous injury or muscle dysfunction requiring different treatment approaches.
Special Tests and Diagnostic Maneuvers
The lower limb's special tests provide specific diagnostic information with quantified sensitivity and specificity:
-
Hip Pathology Detection
- FABER test: 88% sensitivity for hip pathology
- Thomas test: 89% sensitivity for hip flexor tightness
- Trendelenburg: 73% sensitivity for abductor weakness
- FADIR test: 78% sensitivity for FAI
- Log roll: 95% sensitivity for hip irritability
- Ober test: 90% sensitivity for ITB tightness
-
Knee Stability Assessment
- Lachman test: 87% sensitivity, 93% specificity ACL
- Posterior drawer: 79% sensitivity PCL injury
- McMurray test: 70% sensitivity meniscal tear
- Valgus stress: 86% sensitivity MCL injury
- Varus stress: 84% sensitivity LCL injury
- Pivot shift: 98% specificity ACL rupture
-
Ankle-Foot Evaluation
- Anterior drawer: 83% sensitivity ATFL tear
- Talar tilt: 79% sensitivity CFL injury
- Thompson test: 100% sensitivity Achilles rupture
- Single heel rise: >25 repetitions normal
- Windlass test: 100% sensitivity plantar fasciitis
- Tinel's sign: 58% sensitivity tarsal tunnel
⭐ Clinical Pearl: Combining 3+ positive tests increases diagnostic accuracy to >95% for most lower limb pathologies, while single positive tests require correlation with imaging for definitive diagnosis.
Understanding systematic assessment patterns transforms clinical examination from random testing to precise diagnostic investigation. The next section explores how these findings integrate into differential diagnosis frameworks and treatment decision algorithms.
🎯 Clinical Assessment Arsenal: Pattern Recognition Mastery
🔬 Diagnostic Precision: The Differential Matrix
Pathology Classification and Pattern Recognition
The lower limb's pathological presentations follow predictable patterns based on anatomical location and tissue type involvement:
-
Bone Pathology Patterns
- Fractures: mechanism-specific patterns
- Stress injuries: overuse progression
- Tumors: age-related distribution
- Pediatric: metaphyseal location 70%
- Adult: diaphyseal involvement 60%
- Elderly: osteoporotic fragility 80%
-
Joint Pathology Classification
- Degenerative: age >50, bilateral 85%
- Inflammatory: morning stiffness >1 hour
- Infectious: acute onset, fever 90%
- Crystalline: monoarticular 80%
- Traumatic: mechanism correlation 95%
- Mechanical: activity-related symptoms
-
Soft Tissue Injury Patterns
- Acute: <72 hours, inflammatory signs
- Chronic: >6 weeks, degenerative changes
- Overuse: gradual onset, activity-related
- Muscle: eccentric contraction injury
- Tendon: repetitive loading failure
- Ligament: acute stretch/tear mechanism
| Pathology Type | Age Distribution | Location Preference | Symptom Pattern | Diagnostic Accuracy |
|---|---|---|---|---|
| Stress Fracture | 15-35 years | Tibia (50%), Metatarsals (25%) | Progressive pain | MRI 95% |
| Meniscal Tear | 20-40 years | Medial (80%), Posterior horn | Mechanical symptoms | MRI 87% |
| ACL Rupture | 15-25 years | Non-contact (70%) | Immediate swelling | MRI 99% |
| Hip Arthritis | >50 years | Bilateral (60%) | Morning stiffness | X-ray 85% |
| Plantar Fasciitis | 40-60 years | Medial heel (90%) | First-step pain | Clinical 90% |
Clinical Probability and Bayesian Analysis
The lower limb's diagnostic accuracy improves through Bayesian probability integration of pretest probability with test characteristics:
-
Pretest Probability Factors
- Age: <20 years trauma 80%, >60 years degenerative 70%
- Gender: females stress fractures 3x higher
- Activity: runners overuse 60%, contact sports acute 85%
- Mechanism: non-contact ACL 70%, contact fracture 90%
- Duration: acute <1 week trauma 85%, chronic >3 months degenerative 75%
- Location: joint line meniscus 80%, muscle belly strain 90%
-
Test Performance Integration
- High sensitivity: rules out when negative
- High specificity: rules in when positive
- Likelihood ratios: >10 strong evidence, <0.1 strong against
- Positive LR: sensitivity/(1-specificity)
- Negative LR: (1-sensitivity)/specificity
- Post-test odds: pretest odds × LR
⭐ Clinical Pearl: Ottawa Ankle Rules reduce unnecessary X-rays by 30-40% while maintaining 99% sensitivity for fractures, demonstrating how clinical decision rules improve diagnostic efficiency.
Imaging Integration and Evidence Hierarchy
The lower limb's imaging strategy follows evidence-based protocols that optimize diagnostic yield while minimizing cost and radiation:
-
Plain Radiography Indications
- Fracture suspicion: Ottawa rules guide ordering
- Joint pathology: weight-bearing views essential
- Bone tumors: two views minimum requirement
- Sensitivity: fractures 80%, arthritis 85%
- Specificity: fractures 95%, soft tissue 20%
- Cost-effectiveness: first-line imaging 90%
-
Advanced Imaging Selection
- MRI: soft tissue detail, no radiation
- CT: bone detail, fracture characterization
- Ultrasound: dynamic assessment, real-time
- MRI sensitivity: ligaments 95%, cartilage 90%
- CT sensitivity: fractures 99%, bone tumors 95%
- US sensitivity: tendons 85%, muscles 80%
-
Imaging Interpretation Pearls
- Bone marrow edema: stress injury precursor
- Joint effusion: >5mm suprapatellar recess abnormal
- Tendon thickening: >150% normal size pathological
- Signal changes: T2 hyperintensity inflammation
- Enhancement: gadolinium uptake active process
- Morphology: fiber disruption structural damage
💡 Master This: Bone marrow edema on MRI represents stress response and appears 2-8 weeks before radiographic changes, enabling early intervention and prevention of complete stress fractures.
Red Flags and Emergency Recognition
The lower limb's emergency presentations require immediate recognition and urgent intervention to prevent permanent disability:
-
Vascular Emergencies
- Compartment syndrome: pressure >30 mmHg
- Arterial injury: absent pulses, pallor
- Deep vein thrombosis: Wells score >2
- Time-critical: <6 hours compartment syndrome
- Limb-threatening: <4 hours arterial occlusion
- Life-threatening: PE risk 30% untreated DVT
-
Neurological Emergencies
- Cauda equina: bilateral symptoms, bladder dysfunction
- Peroneal nerve: foot drop, lateral leg numbness
- Sciatic nerve: complete motor/sensory loss
- Recovery potential: <24 hours optimal
- Permanent deficit: >72 hours high risk
- Surgical window: <6 hours nerve repair
-
Infectious Emergencies
- Septic arthritis: fever, joint destruction
- Osteomyelitis: bone pain, systemic toxicity
- Necrotizing fasciitis: rapid progression, skin changes
- Mortality: septic arthritis 10%, necrotizing fasciitis 30%
- Joint destruction: <24 hours cartilage damage
- Antibiotic window: <1 hour optimal outcomes
⭐ Clinical Pearl: 5 P's of vascular compromise - Pain, Pallor, Pulselessness, Paresthesias, Paralysis - with paralysis indicating irreversible damage requiring immediate surgical intervention.
Understanding diagnostic precision transforms clinical suspicion into evidence-based diagnosis through systematic probability assessment. The next section explores how these diagnoses translate into treatment algorithms and evidence-based management strategies.
🔬 Diagnostic Precision: The Differential Matrix
⚖️ Treatment Algorithms: Evidence-Based Decision Architecture
Conservative Management Hierarchies
The lower limb's non-operative treatment follows evidence-based protocols with quantified success rates and defined failure criteria:
-
Acute Injury Management (First 72 hours)
- RICE protocol: Rest, Ice, Compression, Elevation
- Pain control: NSAIDs reduce inflammation 40-60%
- Protection: immobilization prevents further damage
- Ice application: 15-20 minutes every 2-3 hours
- Compression: 20-30 mmHg elastic wrap
- Elevation: above heart level reduces swelling 30%
-
Rehabilitation Progression (Weeks 1-12)
- Phase 1: Protection and pain control (weeks 1-2)
- Phase 2: Range of motion restoration (weeks 3-6)
- Phase 3: Strength and endurance (weeks 7-10)
- Phase 4: Functional training (weeks 11-12)
- Success criteria: >90% strength, full ROM
- Return criteria: sport-specific testing >95%
📌 Remember: HARM factors delay healing - Heat, Alcohol, Running, Massage should be avoided for 72 hours post-injury
Surgical Intervention Criteria and Outcomes
The lower limb's operative management requires specific indications with evidence-based success rates and complication profiles:
| Condition | Surgical Indication | Success Rate | Complication Rate | Return Timeline |
|---|---|---|---|---|
| ACL Rupture | Athletes, instability | 90-95% | 5-10% | 6-9 months |
| Meniscal Tear | Mechanical symptoms | 80-90% | 2-5% | 3-6 months |
| Hip Fracture | Displaced >2mm | 85-95% | 10-20% | 3-6 months |
| Ankle Fracture | Unstable, displaced | 90-95% | 5-15% | 3-4 months |
| Achilles Rupture | Athletes, young | 95-98% | 2-8% | 6-12 months |
Pharmacological Management Protocols
The lower limb's medication strategies integrate pain control, inflammation reduction, and healing optimization:
-
Acute Pain Management
- NSAIDs: ibuprofen 400-600mg every 6-8 hours
- Acetaminophen: 1000mg every 6 hours (max 4g/day)
- Topical agents: diclofenac gel 3-4x daily
- Duration: <7-10 days to avoid GI complications
- Contraindications: renal disease, bleeding disorders
- Monitoring: creatinine, liver function if prolonged
-
Chronic Pain Strategies
- Multimodal approach: combination therapy 30% more effective
- Neuropathic agents: gabapentin 300-900mg TID
- Topical options: capsaicin, lidocaine patches
- Opioid avoidance: <3 days acute use recommended
- Adjuvant therapy: muscle relaxants for spasm
- Non-pharmacological: >50% pain reduction possible
-
Injection Therapies
- Corticosteroids: 40mg methylprednisolone intra-articular
- Hyaluronic acid: viscosupplementation for arthritis
- PRP therapy: emerging evidence for tendinopathy
- Success rates: steroids 70-80% short-term
- Duration: 3-6 months typical benefit
- Complications: <2% infection risk
💡 Master This: Corticosteroid injections provide 70-80% pain relief for 3-6 months but should be limited to 3-4 per year to prevent cartilage degradation and tendon weakening.
Rehabilitation and Return-to-Activity Protocols
The lower limb's rehabilitation science follows evidence-based progressions with objective milestones and functional testing:
-
Strength Recovery Targets
- 90% limb symmetry index minimum
- >1.5x body weight single-leg press
- >25 repetitions single heel rise
- Quadriceps: 3-4x body weight isometric
- Hamstring: 60-80% of quadriceps strength
- Calf: 6-8x body weight plantarflexion
-
Functional Movement Standards
- Single-leg hop: >90% contralateral distance
- Y-balance test: >94% composite score
- Landing mechanics: knee valgus <10°
- Agility testing: sport-specific protocols
- Endurance: >80% pre-injury capacity
- Psychological: confidence >80% return scale
-
Return-to-Sport Criteria
- Time-based: minimum healing periods
- Impairment-based: objective measures achieved
- Function-based: sport demands replicated
- Medical clearance: physician approval required
- Performance testing: >95% baseline values
- Risk assessment: reinjury rates <5% acceptable
⭐ Clinical Pearl: Psychological readiness accounts for 25% of return-to-sport success, with fear of reinjury being the strongest predictor of poor outcomes and secondary injury risk.
Understanding treatment algorithms transforms diagnostic certainty into therapeutic success through evidence-based protocols and objective outcome measures. The next section explores how these individual treatments integrate into comprehensive care systems and multidisciplinary approaches.
⚖️ Treatment Algorithms: Evidence-Based Decision Architecture
🔗 Integrated Care Systems: The Multidisciplinary Network
Master integrated care systems, and you transform fragmented treatment into coordinated excellence through systematic collaboration and evidence-based care pathways.
Specialty Integration and Care Coordination
The lower limb's complex pathology requires coordinated expertise from multiple specialties with defined roles and communication protocols:
-
Primary Care Integration
- Initial assessment: >80% conditions managed
- Referral criteria: evidence-based guidelines
- Coordination role: care pathway management
- Screening: Ottawa rules reduce unnecessary referrals 30%
- Triage: urgent vs routine classification
- Follow-up: outcome monitoring and adjustment
-
Orthopedic Surgery Collaboration
- Surgical indications: specific criteria met
- Timing optimization: evidence-based windows
- Outcome tracking: functional measures prioritized
- Success rates: >90% for appropriate candidates
- Complication reduction: protocol adherence 50% improvement
- Recovery acceleration: coordinated rehabilitation 25% faster
-
Physical Therapy Partnership
- Early intervention: within 48-72 hours
- Protocol standardization: evidence-based progressions
- Outcome measurement: objective functional testing
- Cost reduction: conservative management 60% less expensive
- Satisfaction: >85% patient approval
- Prevention: injury recurrence reduced 40%
| Specialty | Primary Role | Intervention Timing | Success Metrics | Cost Impact |
|---|---|---|---|---|
| Primary Care | Screening/Coordination | Immediate | >80% appropriate management | Baseline |
| Orthopedics | Surgical Management | 2-6 weeks | >90% surgical success | 3-5x conservative |
| Physical Therapy | Rehabilitation | 48-72 hours | >85% functional return | 0.6x surgical |
| Sports Medicine | Performance Optimization | Variable | >95% return-to-sport | 1.2x conservative |
| Pain Management | Complex Pain | 6-12 weeks | >70% pain reduction | 2-3x conservative |
Technology Integration and Digital Health
The lower limb's care delivery leverages digital technologies that improve access, monitoring, and outcomes while reducing costs:
-
Telemedicine Applications
- Initial consultation: >70% conditions assessable
- Follow-up care: >90% routine visits suitable
- Specialist access: rural areas benefit 300%
- Satisfaction: >85% patient approval
- Cost reduction: 40-60% vs in-person
- Time savings: 2-3 hours per visit
-
Wearable Technology Integration
- Activity monitoring: step count, gait analysis
- Recovery tracking: objective progress measures
- Compliance monitoring: exercise adherence >80%
- Data accuracy: >95% for basic metrics
- Behavior change: 30% increase activity levels
- Outcome prediction: early warning systems
-
Digital Rehabilitation Platforms
- Exercise prescription: customized protocols
- Progress tracking: real-time feedback
- Adherence improvement: gamification 40% increase
- Cost effectiveness: 50% reduction therapy visits
- Accessibility: 24/7 availability
- Standardization: protocol consistency >95%
⭐ Clinical Pearl: Digital health integration reduces healthcare costs by 25-40% while improving patient satisfaction by 30% and clinical outcomes by 15-20% through enhanced monitoring and protocol adherence.
Quality Metrics and Outcome Optimization
The lower limb's care quality requires systematic measurement and continuous improvement through evidence-based metrics:
-
Clinical Outcome Measures
- Functional scores: WOMAC, KOOS, FAAM
- Return-to-activity: >90% pre-injury level
- Pain reduction: >50% improvement significant
- Quality of life: SF-36 improvement >10 points
- Satisfaction: >85% patient approval
- Complication rates: <5% acceptable threshold
-
Process Quality Indicators
- Time to treatment: <72 hours acute injuries
- Appropriate imaging: Ottawa rules compliance >90%
- Antibiotic timing: <1 hour for infections
- Surgical delays: <48 hours for urgent cases
- Rehabilitation access: <1 week post-injury
- Specialist consultation: <2 weeks routine
-
Cost-Effectiveness Analysis
- Conservative vs surgical: cost-utility ratios
- Prevention programs: ROI >3:1 typical
- Technology adoption: payback period <2 years
- Quality-adjusted life years: QALY improvements
- Healthcare utilization: reduction 20-30%
- Productivity: return-to-work acceleration 25%
💡 Master This: Value-based care models show 25% cost reduction with improved outcomes when multidisciplinary teams use standardized protocols and digital health integration for lower limb conditions.
Future Directions and Innovation Integration
The lower limb's care evolution incorporates emerging technologies and evidence-based innovations that promise transformative improvements:
-
Artificial Intelligence Applications
- Diagnostic imaging: >95% accuracy fracture detection
- Risk prediction: injury prevention algorithms
- Treatment optimization: personalized protocols
- Radiologic interpretation: faster and more accurate
- Clinical decision support: evidence-based recommendations
- Outcome prediction: prognosis modeling >85% accuracy
-
Regenerative Medicine Integration
- Stem cell therapy: emerging evidence cartilage repair
- Growth factors: PRP for tendon healing
- Tissue engineering: scaffold-based reconstruction
- Clinical trials: promising results 60-80% improvement
- Cost considerations: currently expensive but decreasing
- Regulatory approval: gradual expansion indications
-
Precision Medicine Approaches
- Genetic testing: injury susceptibility profiling
- Biomarker development: healing optimization
- Personalized rehabilitation: individual response patterns
- Pharmacogenomics: medication optimization
- Risk stratification: prevention targeting
- Treatment selection: evidence-based individualization
⭐ Clinical Pearl: Integrated care systems using multidisciplinary teams, digital health, and evidence-based protocols achieve 30% better outcomes at 25% lower costs compared to traditional fragmented care models.
Understanding integrated care systems transforms individual expertise into coordinated excellence through systematic collaboration and technology-enhanced delivery. The next section synthesizes these concepts into practical mastery tools for immediate clinical application.
🔗 Integrated Care Systems: The Multidisciplinary Network
🎯 Clinical Mastery Toolkit: Rapid Reference Arsenal
Essential Numbers Arsenal
Master these quantified thresholds and you possess the numerical foundation for 95% of lower limb decisions:
-
Anatomical Constants
- Hip inclination: 125-135° normal range
- Q-angle: 13° males, 18° females
- Compartment pressure: >30 mmHg pathological
- Leg length discrepancy: >2cm significant
- Joint space: >3mm normal knee
- Achilles tendon force: 4,000 N running
-
Clinical Thresholds
- Ottawa ankle: >55 years or unable to bear weight
- Wells DVT score: >2 high probability
- Fracture healing: 6-8 weeks cortical bone
- Ligament healing: 6-12 weeks complete
- Muscle strain: 2-6 weeks depending grade
- Return-to-sport: >90% strength symmetry
📌 Remember: NUMBERS save lives - Normal ranges, Urgent thresholds, Measurement standards, Benchmark values, Emergency criteria, Recovery timelines, Success metrics
Rapid Assessment Protocols
Transform complex examinations into systematic efficiency through structured protocols:
| Assessment Phase | Time Allocation | Key Elements | Decision Points |
|---|---|---|---|
| History | 2-3 minutes | Mechanism, timing, function | Red flags present? |
| Inspection | 1 minute | Alignment, swelling, deformity | Obvious pathology? |
| Palpation | 2 minutes | Tenderness, temperature, pulses | Localized findings? |
| Movement | 3-4 minutes | ROM, strength, stability | Functional limitation? |
| Special Tests | 2-3 minutes | Targeted based on findings | Positive tests? |
Diagnostic Decision Trees
Master pattern recognition through algorithmic thinking:
-
Acute Knee Pain Algorithm
- Mechanism: contact vs non-contact
- Swelling: immediate vs delayed
- Function: weight-bearing ability
- Contact + immediate swelling = fracture/ACL
- Non-contact + delayed swelling = meniscus
- Gradual onset + morning stiffness = arthritis
-
Hip Pain Localization
- Anterior: hip joint pathology
- Lateral: trochanteric bursitis
- Posterior: referred from spine
- Groin pain = intra-articular
- Buttock pain = extra-articular
- Thigh pain = referred
-
Ankle Injury Classification
- Inversion mechanism: lateral ligaments
- Eversion mechanism: medial/syndesmotic
- Axial loading: fracture/osteochondral
- Anterior drawer positive = ATFL tear
- Talar tilt positive = CFL involvement
- Syndesmotic tests = high ankle sprain
💡 Master This: Location + Mechanism + Timing provides >80% diagnostic accuracy before physical examination, enabling targeted assessment and efficient resource utilization.
Treatment Quick Reference
Access evidence-based interventions through rapid protocols:
-
Conservative Management Hierarchy
- RICE protocol (first 72 hours)
- NSAIDs for inflammation (7-10 days maximum)
- Physical therapy (start 48-72 hours)
- Activity modification (avoid aggravating factors)
- Gradual return (meet functional criteria)
-
Injection Therapy Guidelines
- Corticosteroids: 40mg methylprednisolone intra-articular
- Frequency: maximum 3-4 per year
- Success rate: 70-80% pain relief
- Duration: 3-6 months typical benefit
- Contraindications: infection, fracture
- Complications: <2% serious adverse events
-
Surgical Referral Criteria
- Immediate: fracture displacement, neurovascular compromise
- Urgent (24-48 hours): infection, compartment syndrome
- Semi-urgent (1-2 weeks): mechanical symptoms, instability
- Routine (4-6 weeks): failed conservative management
- Elective: quality of life improvement
- Preventive: high-risk pathology
Emergency Recognition Matrix
Identify life/limb-threatening conditions within seconds:
| Condition | Key Signs | Time Window | Intervention |
|---|---|---|---|
| Compartment Syndrome | Pain out of proportion | <6 hours | Immediate fasciotomy |
| Arterial Injury | 5 P's present | <4 hours | Vascular surgery |
| Septic Arthritis | Fever + joint pain | <24 hours | Arthroscopic washout |
| Cauda Equina | Bilateral symptoms | <48 hours | Emergency decompression |
| Necrotizing Fasciitis | Rapid progression | <6 hours | Aggressive debridement |
Outcome Prediction Tools
Anticipate recovery trajectories through evidence-based prognostic factors:
-
Positive Prognostic Indicators
- Age <40 years: faster healing 25%
- Non-smoker: complication reduction 50%
- Good baseline fitness: recovery acceleration 30%
- Early mobilization: outcome improvement 20%
- Compliance: success rate >90%
- Social support: satisfaction increase 25%
-
Negative Prognostic Factors
- Diabetes: healing delay 40%
- Obesity: complication increase 200%
- Chronic pain: poor outcome 60%
- Smoking: healing impairment 50%
- Depression: recovery delay 35%
- Litigation: outcome reduction 40%
💡 Master This: Combining 3+ positive prognostic factors predicts >90% successful outcomes, while 2+ negative factors indicate high-risk patients requiring intensive management and realistic expectations.
This clinical mastery toolkit transforms complex knowledge into accessible expertise, enabling rapid decision-making and optimal patient care through evidence-based protocols and systematic approaches.
🎯 Clinical Mastery Toolkit: Rapid Reference Arsenal
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for NEET-PG prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app




















