Functional Anatomy

On this page
🧠 Deep Brain Directors - The Inner Circle
Your brain orchestrates every thought, movement, and breath through an elegant hierarchy of structures working in concert. This lesson takes you from the deep limbic regulators and brainstem life-support centers, through the commanding cerebral cortex, down the spinal superhighways that relay signals to your body. You'll learn how each region contributes its specialized function, how they integrate across systems, and which clinical pearls will sharpen your diagnostic eye at the bedside.
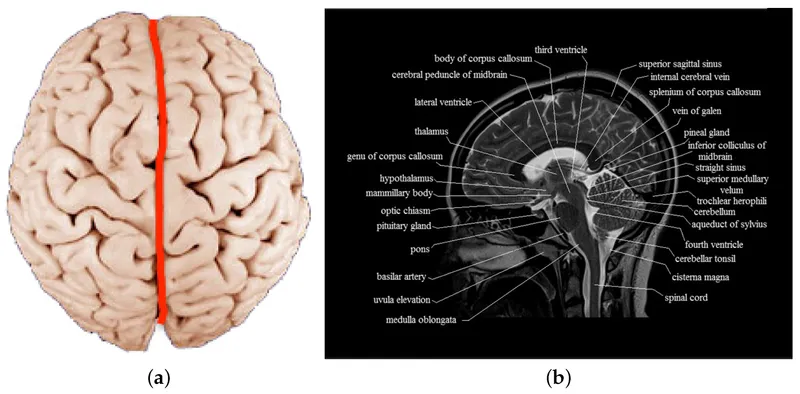
Thalamic Relay Architecture
The thalamus functions as the brain's central switching station, processing 95% of sensory information before cortical distribution. This bilateral ovoid structure measures 4cm anteroposteriorly and 1.5cm mediolaterally, containing over 50 distinct nuclei organized into functional territories.
-
Anterior Nuclear Group
- Anterior nucleus: limbic circuit integration (memory consolidation)
- Connects mammillary bodies → hippocampus via fornix pathway
- Lesions cause anterograde amnesia in 85% of cases
- Papez circuit disruption: emotion-memory interface
- Korsakoff syndrome correlation: thiamine deficiency
-
Medial Nuclear Group
- Mediodorsal nucleus: executive function and working memory
- Prefrontal cortex connectivity: areas 9, 10, 46
- Damage produces frontal lobe syndrome in 70% of patients
- Personality changes: disinhibition, poor judgment
- Wisconsin Card Sort deficits: cognitive flexibility loss
-
Lateral Nuclear Group
- Ventral posterior lateral (VPL): body sensation relay
- Ventral posterior medial (VPM): facial sensation relay
- Ventral lateral (VL): motor control coordination
- Receives cerebellar and basal ganglia input
- Projects to primary motor cortex (area 4)
📌 Remember: LAMP for thalamic nuclei - Lateral (sensation/motor), Anterior (memory), Medial (executive), Posterior (vision/hearing)
| Thalamic Nucleus | Primary Input | Cortical Target | Function | Lesion Effect | Clinical Correlation |
|---|---|---|---|---|---|
| VPL | Medial lemniscus, spinothalamic | S1 (areas 3,1,2) | Body sensation | Hemianesthesia | Thalamic pain syndrome |
| VPM | Trigeminal, gustatory | S1 face area | Facial sensation | Facial numbness | Trigeminal neuralgia |
| VL | Cerebellum, globus pallidus | M1 (area 4) | Motor control | Hemiparesis | Thalamic hand |
| Mediodorsal | Amygdala, orbitofrontal | Prefrontal cortex | Executive function | Personality change | Frontal dementia |
| Anterior | Mammillary bodies | Cingulate cortex | Memory processing | Anterograde amnesia | Korsakoff syndrome |
Hypothalamic Command Centers
The hypothalamus weighs only 4 grams yet controls autonomic, endocrine, and behavioral homeostasis through 11 major nuclei organized into 3 functional zones. This almond-sized structure maintains life-critical parameters within narrow physiological ranges.
-
Periventricular Zone (medial)
- Paraventricular nucleus (PVN): stress response headquarters
- CRH production: cortisol cascade initiation
- ADH synthesis: water balance regulation (280-295 mOsm/kg)
- Suprachiasmatic nucleus: circadian pacemaker
- 24.2-hour endogenous rhythm generation
- Melatonin suppression: light exposure at >1000 lux
- Paraventricular nucleus (PVN): stress response headquarters
-
Medial Zone (tuberal region)
- Arcuate nucleus: metabolic control center
- POMC neurons: appetite suppression (α-MSH release)
- NPY/AgRP neurons: feeding stimulation (ghrelin responsive)
- Ventromedial nucleus: satiety center
- Glucose sensing: 2.5-5.0 mmol/L normal range
- Lesions cause hyperphagia and obesity in 90% of cases
- Arcuate nucleus: metabolic control center
-
Lateral Zone
- Lateral hypothalamic area: feeding center
- Orexin/hypocretin neurons: arousal and appetite
- Damage produces aphagia and adipsia (starvation syndrome)
- Supraoptic nucleus: ADH and oxytocin production
- Magnocellular neurons: posterior pituitary hormone storage
- Lateral hypothalamic area: feeding center
💡 Master This: Hypothalamic lesions follow the "4 F's" - Feeding, Fighting, Fleeing, Fornication (reproduction) - representing the core survival behaviors controlled by this region
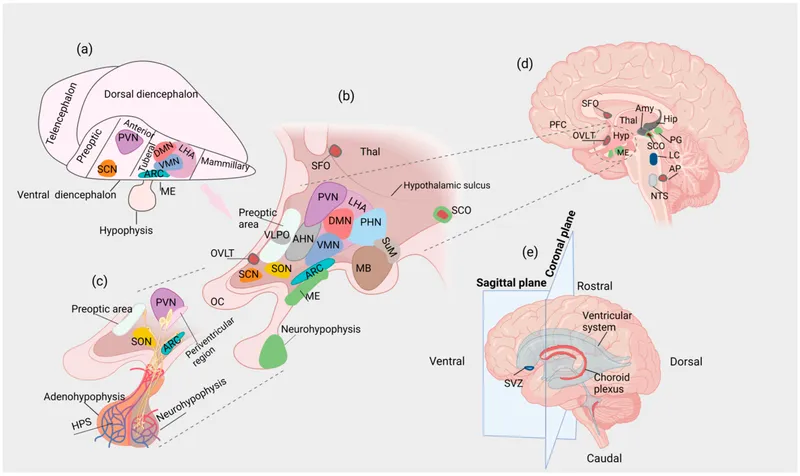
Basal Ganglia Movement Circuits
The basal ganglia comprise 5 interconnected nuclei forming parallel processing loops that modulate voluntary movement, procedural learning, and habit formation. These circuits process motor, cognitive, and limbic information through direct and indirect pathways.
-
Striatal Input Processing
- Caudate nucleus: cognitive and oculomotor control
- Head: executive function and working memory
- Body/tail: associative learning and habit formation
- Putamen: motor and somatosensory integration
- Dorsal: skilled movement execution
- Ventral: limbic-motor interface (motivation)
- Caudate nucleus: cognitive and oculomotor control
-
Pallidal Output Control
- Globus pallidus externa (GPe): indirect pathway modulation
- GABAergic inhibition: subthalamic nucleus regulation
- Firing rate: 60-80 Hz baseline activity
- Globus pallidus interna (GPi): direct pathway output
- Thalamic projection: VL/VA nuclei targeting
- Substantia nigra coordination: dopamine modulation
- Globus pallidus externa (GPe): indirect pathway modulation
📌 Remember: CLIPS for basal ganglia - Caudate (cognitive), Lentiform (putamen+pallidum), Internal capsule, Putamen (motor), Substantia nigra (dopamine)
The direct pathway facilitates movement through disinhibition: Cortex → Striatum → GPi/SNr → Thalamus → Cortex (net excitation). The indirect pathway suppresses movement through increased inhibition: Cortex → Striatum → GPe → STN → GPi/SNr → Thalamus → Cortex (net inhibition).
⭐ Clinical Pearl: Parkinson's disease results from >80% dopaminergic neuron loss in substantia nigra pars compacta, disrupting the direct/indirect pathway balance and producing the classic bradykinesia-rigidity-tremor triad
Understanding these deep brain directors reveals how millimeter-scale structures orchestrate whole-body functions, setting the foundation for comprehending how brainstem and cerebellar circuits execute these commands through life's little controllers.
🧠 Deep Brain Directors — The Inner Circle
🎛️ Brainstem & Cerebellum - Life's Little Controllers
Midbrain Command Architecture
The midbrain spans 2cm and houses critical motor and sensory integration centers, including the substantia nigra, red nucleus, and superior/inferior colliculi. This region processes visual-auditory reflexes and dopaminergic motor control with millisecond response times.
-
Tectum (Dorsal Midbrain)
- Superior colliculus: visual-spatial attention and saccadic eye movements
- 7-layer organization: superficial (visual), deep (motor)
- Saccade generation: 15-20 degree maximum amplitude
- Reaction time: 150-200 milliseconds for visually-guided movements
- Inferior colliculus: auditory processing and sound localization
- Tonotopic organization: frequency mapping (20 Hz - 20 kHz)
- Binaural integration: interaural time differences (<1 millisecond)
- Superior colliculus: visual-spatial attention and saccadic eye movements
-
Tegmentum (Ventral Midbrain)
- Red nucleus: rubrospinal tract origin and motor coordination
- Magnocellular portion: limb movement control
- Parvocellular portion: cerebellar input integration
- Substantia nigra: dopamine production and movement facilitation
- Pars compacta: dopaminergic neurons (A9 cell group)
- Pars reticulata: GABAergic output to thalamus
- Dopamine concentration: 8-10 μg/g tissue (highest in brain)
- Red nucleus: rubrospinal tract origin and motor coordination
-
Periaqueductal Gray (PAG)
- Pain modulation: descending inhibition via raphe nuclei
- Defensive behaviors: fight-or-flight response coordination
- Opioid sensitivity: μ-receptor dense regions
- Stimulation produces analgesia in 80% of chronic pain patients
📌 Remember: SIRS for midbrain - Superior colliculus (vision), Inferior colliculus (hearing), Red nucleus (motor), Substantia nigra (dopamine)
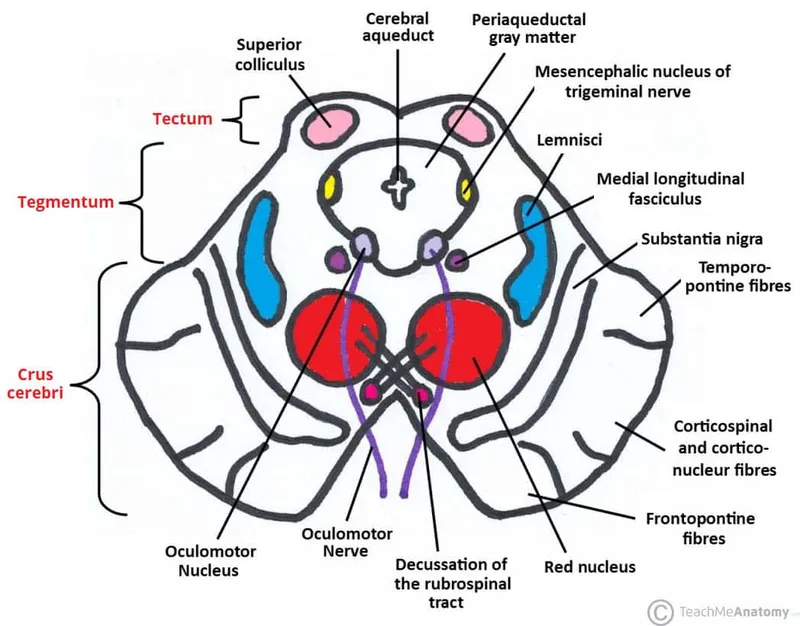
| Midbrain Structure | Primary Function | Input Sources | Output Targets | Clinical Correlation | Lesion Effects |
|---|---|---|---|---|---|
| Superior colliculus | Saccadic eye movements | Retina, visual cortex | Brainstem gaze centers | Parinaud syndrome | Vertical gaze palsy |
| Inferior colliculus | Auditory processing | Cochlear nuclei, SOC | Medial geniculate | Acoustic neuroma | Hearing loss |
| Red nucleus | Motor coordination | Motor cortex, cerebellum | Spinal cord, olive | Benedikt syndrome | Tremor, ataxia |
| Substantia nigra | Movement facilitation | Striatum, cortex | Striatum, thalamus | Parkinson disease | Bradykinesia |
| PAG | Pain modulation | Hypothalamus, amygdala | Raphe, locus coeruleus | Chronic pain | Hyperalgesia |
The pons measures 2.5cm in length and serves as the neural crossroads connecting cerebrum, cerebellum, and spinal cord. This region contains 4 cranial nerve nuclei (CN V-VIII) and critical respiratory centers maintaining breathing rhythm and sleep-wake cycles.
-
Pontine Nuclei Complex
- Pontine respiratory group: breathing rhythm modification
- Pneumotaxic center: inspiratory termination (apneustic prevention)
- Normal respiratory rate: 12-16 breaths/minute
- Tidal volume regulation: 500mL at rest
- Locus coeruleus: norepinephrine production and arousal
- A6 cell group: vigilance and attention control
- REM sleep suppression: muscle atonia prevention
- Stress response: fight-or-flight preparation
- Pontine respiratory group: breathing rhythm modification
-
Cranial Nerve Nuclear Organization
- Trigeminal complex (CN V): facial sensation and mastication
- Motor nucleus: jaw muscles (masseter, temporalis)
- Sensory nuclei: touch, pain, temperature processing
- Facial nucleus (CN VII): facial expression and taste
- Upper motor neuron lesions: forehead sparing
- Lower motor neuron lesions: complete facial paralysis
- Vestibulocochlear nuclei (CN VIII): hearing and balance
- 4 vestibular nuclei: spatial orientation processing
- 2 cochlear nuclei: auditory signal relay
- Trigeminal complex (CN V): facial sensation and mastication
💡 Master This: Pontine lesions create crossed deficits - ipsilateral cranial nerve signs with contralateral motor/sensory deficits due to corticospinal and medial lemniscal tract involvement before decussation
Medullary Vital Centers
The medulla oblongata extends 3cm from foramen magnum to pontomedullary junction, containing life-critical centers controlling cardiovascular, respiratory, and digestive functions. Damage to these regions proves rapidly fatal without mechanical support.
-
Cardiovascular Control Centers
- Vasomotor center: blood pressure regulation
- Pressor area: sympathetic activation (vasoconstriction)
- Depressor area: parasympathetic activation (vasodilation)
- Baroreceptor integration: carotid sinus and aortic arch
- Cardiac center: heart rate and contractility control
- Cardioacceleratory center: sympathetic stimulation
- Cardioinhibitory center: vagal stimulation
- Normal heart rate: 60-100 bpm at rest
- Vasomotor center: blood pressure regulation
-
Respiratory Control Centers
- Medullary rhythmicity center: automatic breathing generation
- Pre-Bötzinger complex: inspiratory rhythm generation
- Bötzinger complex: expiratory neuron coordination
- CO2 sensitivity: pH changes trigger ventilation increase
- Chemoreceptor integration: central and peripheral inputs
- Central: medullary CO2/pH sensing (80% of drive)
- Peripheral: carotid body O2 sensing (20% of drive)
- Medullary rhythmicity center: automatic breathing generation
⭐ Clinical Pearl: Ondine's curse (central hypoventilation) results from medullary damage, requiring mechanical ventilation during sleep when voluntary respiratory control ceases
Cerebellar Precision Engineering
The cerebellum occupies 10% of brain volume yet contains 75% of all neurons (150 billion), organized into 3 functional zones processing motor learning, balance, and cognitive functions with extraordinary precision. This structure enables error correction and movement refinement through feed-forward and feedback mechanisms.
-
Cerebellar Cortex Organization
- 3-layer architecture: molecular, Purkinje, granular
- Purkinje cells: sole cortical output (GABAergic inhibition)
- Parallel fibers: granule cell axons (200,000 per Purkinje cell)
- Climbing fibers: olivary input (1:1 ratio with Purkinje cells)
-
Functional Zonation
- Vestibulocerebellum (flocculonodular lobe): balance and eye movements
- Vestibular input integration: semicircular canals and otoliths
- VOR (vestibulo-ocular reflex): gaze stabilization during head movement
- Spinocerebellum (vermis + paravermis): posture and locomotion
- Somatotopic organization: body map representation
- Spinal input: proprioception and motor commands
- Cerebrocerebellum (lateral hemispheres): motor planning and cognition
- Cortical input: association areas and motor cortex
- Motor learning: adaptation and skill acquisition
- Vestibulocerebellum (flocculonodular lobe): balance and eye movements
📌 Remember: VeSPiCe for cerebellar zones - Vestibulo (balance), SPino (posture), Cerebro (planning)
| Cerebellar Zone | Primary Input | Deep Nuclei | Output Target | Function | Lesion Signs |
|---|---|---|---|---|---|
| Vestibulocerebellum | Vestibular organs | Vestibular nuclei | Brainstem, spinal cord | Balance, VOR | Ataxia, nystagmus |
| Spinocerebellum | Spinal cord, brainstem | Fastigial, interposed | Brainstem, red nucleus | Posture, locomotion | Truncal ataxia |
| Cerebrocerebellum | Cerebral cortex | Dentate | Thalamus, cortex | Motor planning | Limb ataxia |
⭐ Clinical Pearl: Cerebellar cognitive affective syndrome affects executive function, language, and emotion following posterior lobe lesions, demonstrating cerebellar involvement beyond motor control
These brainstem and cerebellar controllers establish the neural infrastructure supporting higher cortical functions, preparing the foundation for understanding how the cerebral cortex orchestrates complex behaviors as the brain's big boss.
🎛️ Brainstem & Cerebellum — Life's Little Controllers
🏛️ Cerebral Cortex - Brain's Big Boss
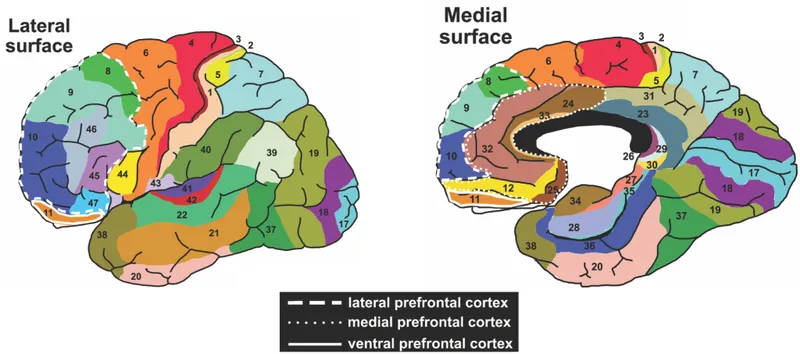
Cortical Architectural Principles
The cerebral cortex exhibits laminar organization with 6 horizontal layers and vertical columnar processing units spanning cortical thickness. Each cortical column measures 0.5mm diameter and contains ~100,000 neurons sharing similar receptive fields and response properties.
-
Laminar Organization (Layers I-VI)
- Layer I (molecular): apical dendrites and horizontal connections
- Sparse cell bodies (<5% of cortical neurons)
- Long-range connectivity between distant cortical areas
- Layers II-III (external granular/pyramidal): cortico-cortical connections
- Pyramidal neurons: excitatory output (glutamate)
- Association and commissural projections
- Layer IV (internal granular): thalamic input reception
- Stellate cells: local processing and distribution
- Highest density in primary sensory areas
- Layer V (internal pyramidal): subcortical output
- Large pyramidal neurons: corticospinal, corticobulbar tracts
- Betz cells: giant motor neurons (up to 100μm diameter)
- Layer VI (multiform): thalamic feedback and local modulation
- Layer I (molecular): apical dendrites and horizontal connections
-
Columnar Organization
- Minicolumns: 80-100 neurons in 30μm diameter units
- Macrocolumns: 300-600μm diameter functional units
- Ocular dominance columns: 400-500μm spacing in V1
- Orientation columns: 50μm spacing for 10-degree increments
📌 Remember: MEGA-BM for cortical layers - Molecular, External granular, External pyramidal, Granular, Association (internal pyramidal), Big cells, Multiform
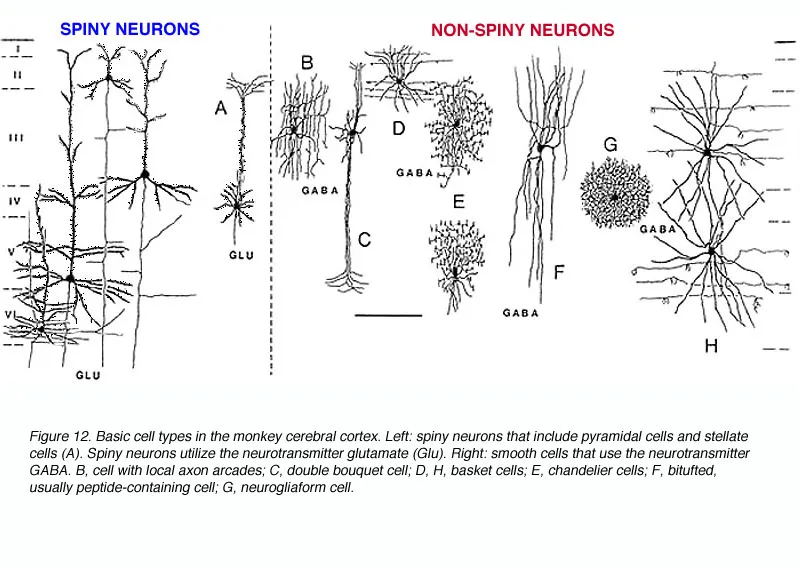
| Cortical Layer | Primary Cell Type | Main Connections | Neurotransmitter | Function | Pathology |
|---|---|---|---|---|---|
| I | Horizontal cells | Long-range cortical | GABA | Integration | Alzheimer tangles |
| II-III | Pyramidal neurons | Cortico-cortical | Glutamate | Association | Schizophrenia |
| IV | Stellate cells | Thalamo-cortical | Glutamate | Input processing | Stroke |
| V | Large pyramidal | Subcortical output | Glutamate | Motor output | ALS |
| VI | Multiform cells | Cortico-thalamic | Glutamate/GABA | Feedback | Epilepsy |
Primary sensory areas receive direct thalamic input and exhibit precise topographic organization reflecting peripheral receptor distributions. These areas process basic features before hierarchical elaboration in secondary and association cortices.
-
Primary Somatosensory Cortex (S1, Areas 3a, 3b, 1, 2)
- Postcentral gyrus location: Brodmann areas 3, 1, 2
- Somatotopic organization: sensory homunculus representation
- Lips/hands: disproportionate representation (40% of S1)
- Two-point discrimination: 2-3mm (fingertips), 40mm (back)
- Modality segregation: area 3a (proprioception), 3b (touch), 1 (texture), 2 (shape)
- Receptive field sizes: 2-5mm (area 3b), 10-30mm (area 2)
-
Primary Visual Cortex (V1, Area 17)
- Calcarine fissure location: striate cortex
- Retinotopic organization: visual field mapping
- Foveal representation: 50% of V1 (central 10 degrees)
- Peripheral compression: logarithmic scaling
- Ocular dominance columns: left/right eye segregation
- Orientation selectivity: simple and complex cell responses
- Spatial resolution: 1 arcminute (foveal), 30 arcminutes (peripheral)
-
Primary Auditory Cortex (A1, Areas 41, 42)
- Heschl's gyrus location: superior temporal plane
- Tonotopic organization: frequency mapping
- Low frequencies (250-500 Hz): anterolateral
- High frequencies (8-16 kHz): posteromedial
- Binaural processing: interaural time and intensity differences
- Frequency resolution: 1-3% discrimination threshold
💡 Master This: Primary sensory areas exhibit columnar organization where vertical electrode penetrations encounter neurons with similar receptive field properties, while horizontal movements reveal systematic changes in preferred stimuli
Motor Control Hierarchies
Motor cortical areas organize movement planning and execution through hierarchical processing from abstract intentions to specific muscle commands. The primary motor cortex provides direct corticospinal output, while premotor and supplementary areas contribute movement preparation and sequencing.
-
Primary Motor Cortex (M1, Area 4)
- Precentral gyrus location: anterior to central sulcus
- Somatotopic organization: motor homunculus
- Hand/face areas: disproportionate representation (60% of M1)
- Betz cells: 3-5% of corticospinal neurons (largest diameter)
- Movement parameters: force, direction, velocity encoding
- Plasticity: use-dependent reorganization within hours-days
-
Premotor Cortex (PM, Area 6)
- Lateral premotor: externally-guided movements
- Visual-motor transformations: reaching to targets
- Mirror neurons: action observation and imitation
- Dorsal premotor: conditional motor learning
- Arbitrary stimulus-response associations
- Rule-based movement selection
- Lateral premotor: externally-guided movements
-
Supplementary Motor Area (SMA, Medial Area 6)
- Self-initiated movement preparation
- Motor sequence learning and execution
- Bimanual coordination and timing
- Bereitschaftspotential: movement-related potential (1-2 seconds before action)
⭐ Clinical Pearl: Apraxia results from left parietal or premotor lesions, disrupting learned motor programs while preserving basic strength and coordination - patients cannot pantomime tool use despite understanding the task
Association Cortex Integration
Association areas comprise 75% of human cortex and integrate multimodal information for higher-order cognitive functions including language, spatial processing, executive control, and social cognition. These regions exhibit extensive interconnectivity and prolonged developmental maturation.
-
Parietal Association Areas
- Superior parietal lobule (areas 5, 7): spatial attention and visuomotor integration
- Spatial neglect: right hemisphere lesions (40% of strokes)
- Reaching and grasping: visual-proprioceptive coordination
- Inferior parietal lobule: language and numerical processing
- Angular gyrus: reading comprehension and mathematical concepts
- Supramarginal gyrus: phonological processing and working memory
- Superior parietal lobule (areas 5, 7): spatial attention and visuomotor integration
-
Temporal Association Areas
- Superior temporal sulcus: social cognition and biological motion
- Face processing: fusiform face area specialization
- Theory of mind: mental state attribution
- Inferior temporal cortex: object recognition and semantic memory
- Grandmother cells: highly selective neuronal responses
- Category selectivity: faces, places, tools, words
- Superior temporal sulcus: social cognition and biological motion
-
Frontal Association Areas
- Dorsolateral prefrontal (areas 9, 46): working memory and cognitive control
- N-back tasks: 2-3 item capacity in healthy adults
- Wisconsin Card Sort: set-shifting and rule learning
- Orbitofrontal cortex: decision-making and emotional regulation
- Iowa Gambling Task: advantageous choice learning
- Social behavior: empathy and moral reasoning
- Dorsolateral prefrontal (areas 9, 46): working memory and cognitive control
📌 Remember: STEP for association cortex - Spatial (parietal), Temporal (object/face), Executive (frontal), Phonological (left hemisphere)
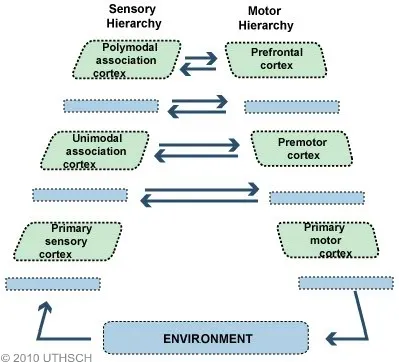
| Association Area | Brodmann Areas | Primary Function | Lesion Syndrome | Lateralization | Development |
|---|---|---|---|---|---|
| Superior parietal | 5, 7 | Spatial attention | Neglect syndrome | Right dominant | Age 12-15 |
| Angular gyrus | 39 | Reading, math | Gerstmann syndrome | Left dominant | Age 8-12 |
| Superior temporal | 22 | Social cognition | Autism spectrum | Bilateral | Age 15-20 |
| Dorsolateral PFC | 9, 46 | Working memory | Dysexecutive syndrome | Bilateral | Age 20-25 |
| Orbitofrontal | 11, 47 | Decision-making | Acquired sociopathy | Right dominant | Age 25-30 |
Understanding cortical organization connects structural anatomy to functional capabilities, revealing how localized damage produces specific deficits and how targeted interventions can promote neural recovery through experience-dependent plasticity.
🏛️ Cerebral Cortex — Brain's Big Boss
🧭 Spinal Cord & Tracts - Neural Superhighway
Spinal Cord Segmental Architecture
The spinal cord exhibits metameric organization with 31 segments (8 cervical, 12 thoracic, 5 lumbar, 5 sacral, 1 coccygeal) corresponding to vertebral levels with predictable offset patterns. Each segment contains gray matter processing centers surrounded by white matter tracts.
-
Gray Matter Organization
- Anterior horn: motor neurons and interneurons
- Alpha motor neurons: extrafusal muscle innervation (30-120 μm diameter)
- Gamma motor neurons: intrafusal muscle spindle control (2-8 μm)
- Renshaw cells: recurrent inhibition via acetylcholine
- Posterior horn: sensory processing and integration
- Substantia gelatinosa (Lamina II): pain and temperature modulation
- Nucleus proprius (Laminae III-IV): touch and pressure relay
- Clarke's column (C8-L2): unconscious proprioception to cerebellum
- Lateral horn (T1-L2): sympathetic preganglionic neurons
- Intermediolateral cell column: autonomic control center
- Sacral parasympathetic (S2-S4): pelvic organ innervation
- Anterior horn: motor neurons and interneurons
-
Segmental Levels and Clinical Correlations
- Cervical enlargement (C5-T1): upper limb innervation
- C5-C6: deltoid, biceps (axillary, musculocutaneous nerves)
- C8-T1: hand intrinsics (ulnar, median nerves)
- Lumbar enlargement (L1-S2): lower limb innervation
- L2-L4: quadriceps (femoral nerve)
- L5-S1: foot dorsiflexors (peroneal nerve)
- Cervical enlargement (C5-T1): upper limb innervation
📌 Remember: SAME for spinal cord levels - Sensory (posterior), Autonomic (lateral), Motor (anterior), Enlargements (cervical C5-T1, lumbar L1-S2)
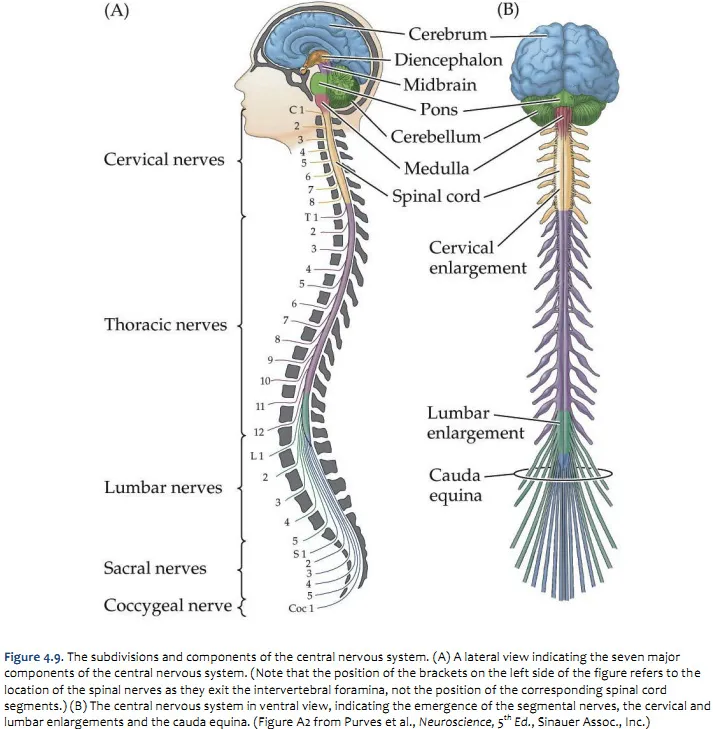
| Spinal Level | Vertebral Level | Key Muscles | Reflexes | Sensory Landmarks | Clinical Tests |
|---|---|---|---|---|---|
| C5 | C4-C5 | Deltoid, biceps | Biceps (C5-C6) | Lateral arm | Shoulder abduction |
| C6 | C5-C6 | Wrist extensors | Brachioradialis | Thumb, index | Wrist extension |
| C7 | C6-C7 | Triceps, finger extensors | Triceps (C7-C8) | Middle finger | Elbow extension |
| C8 | C7-T1 | Hand intrinsics | Finger flexors | Ring, little finger | Finger abduction |
| L4 | L2-L3 | Quadriceps, tibialis anterior | Patellar (L2-L4) | Medial leg | Knee extension |
| S1 | L5-S1 | Gastrocnemius, gluteus maximus | Achilles (S1-S2) | Lateral foot | Plantar flexion |
Ascending tracts convey sensory information from peripheral receptors to brain centers through three-neuron pathways with specific decussation patterns and somatotopic organization. Understanding these pathways enables precise localization of sensory deficits.
-
Dorsal Column-Medial Lemniscal Pathway
- Function: fine touch, vibration, proprioception, two-point discrimination
- First-order neurons: dorsal root ganglia → dorsal columns
- Fasciculus gracilis: lower body (T6 and below)
- Fasciculus cuneatus: upper body (above T6)
- Second-order neurons: nucleus gracilis/cuneatus → medial lemniscus
- Decussation: internal arcuate fibers at medulla
- Third-order neurons: VPL thalamus → primary somatosensory cortex
- Clinical testing: vibration (128 Hz tuning fork), position sense
-
Spinothalamic Pathway
- Function: pain, temperature, crude touch
- First-order neurons: dorsal root ganglia → posterior horn
- Second-order neurons: substantia gelatinosa → anterior white commissure
- Decussation: 1-2 segments above entry level
- Lateral spinothalamic: pain and temperature
- Anterior spinothalamic: crude touch and pressure
- Third-order neurons: VPL thalamus → somatosensory cortex
- Clinical testing: pinprick, temperature discrimination
-
Spinocerebellar Pathways
- Function: unconscious proprioception for movement coordination
- Posterior spinocerebellar: muscle spindle and Golgi tendon organ input
- Clarke's column (C8-L2) → ipsilateral cerebellar cortex
- Inferior cerebellar peduncle entry
- Anterior spinocerebellar: interneuron activity and central commands
- Spinal border cells → contralateral then recross in cerebellum
- Superior cerebellar peduncle entry
💡 Master This: DCML carries discriminative touch that can localize stimuli precisely, while spinothalamic carries protective sensations that motivate withdrawal - this explains why syringomyelia causes dissociated sensory loss with preserved touch but lost pain/temperature
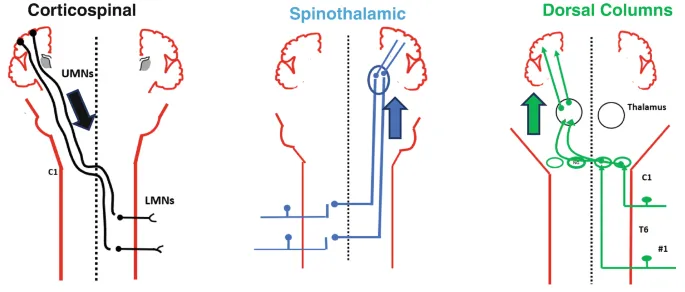
Descending Motor Pathways
Descending tracts transmit motor commands from brain centers to spinal motor neurons through direct and indirect pathways. These systems control voluntary movement, posture, and muscle tone with distinct anatomical and functional characteristics.
-
Corticospinal Tract (Pyramidal System)
- Function: voluntary, skilled movements, especially distal muscles
- Origin: primary motor cortex (30%), premotor (30%), somatosensory (40%)
- Pathway organization:
- Lateral corticospinal (85%): decussates at pyramids
- Anterior corticospinal (15%): uncrossed, bilateral innervation
- Termination: interneurons (90%) and motor neurons (10%)
- Somatotopy: cervical (lateral), lumbar (medial) in lateral funiculus
-
Extrapyramidal Motor Systems
- Rubrospinal tract: red nucleus → cervical spinal cord
- Flexor bias in upper extremities
- Decussates in ventral tegmental decussation
- Reticulospinal tracts: brainstem → axial and proximal muscles
- Pontine reticulospinal: extensor facilitation
- Medullary reticulospinal: flexor facilitation
- Vestibulospinal tracts: vestibular nuclei → antigravity muscles
- Lateral vestibulospinal: ipsilateral extensor facilitation
- Medial vestibulospinal: neck and upper trunk control
- Rubrospinal tract: red nucleus → cervical spinal cord
-
Autonomic Descending Control
- Hypothalamospinal tract: hypothalamus → sympathetic preganglionic neurons
- Descending pain modulation: periaqueductal gray → raphe → dorsal horn
- Respiratory control: medullary centers → phrenic motor neurons (C3-C5)
⭐ Clinical Pearl: Upper motor neuron lesions cause spastic paralysis with hyperreflexia and Babinski signs, while lower motor neuron lesions produce flaccid paralysis with areflexia and fasciculations - this distinction localizes lesions above or below the anterior horn
| Descending Tract | Origin | Decussation | Target | Function | Lesion Effect |
|---|---|---|---|---|---|
| Lateral corticospinal | Motor cortex | Pyramidal | Lateral motor neurons | Skilled movement | Spastic hemiparesis |
| Anterior corticospinal | Motor cortex | Segmental | Medial motor neurons | Bilateral control | Axial weakness |
| Rubrospinal | Red nucleus | Ventral tegmental | Cervical interneurons | Upper limb flexion | Decerebrate posture |
| Reticulospinal | Brainstem | Partial | Axial motor neurons | Posture, tone | Postural instability |
| Vestibulospinal | Vestibular nuclei | None | Extensor motor neurons | Balance, antigravity | Ataxia, falls |
Spinal reflexes represent hardwired neural circuits that produce stereotyped responses to specific stimuli without conscious control. These circuits provide protective responses, postural adjustments, and movement coordination with millisecond latencies.
-
Monosynaptic Stretch Reflex
- Pathway: muscle spindle → Ia afferent → alpha motor neuron
- Latency: 15-30 milliseconds (fastest reflex)
- Function: muscle length regulation and postural maintenance
- Clinical testing: deep tendon reflexes (biceps, triceps, patellar, Achilles)
- Grading: 0 (absent) to 4+ (hyperactive with clonus)
-
Polysynaptic Flexor Reflex
- Pathway: nociceptor → interneurons → flexor motor neurons
- Latency: 50-200 milliseconds
- Function: withdrawal from harmful stimuli
- Crossed extension: contralateral extensor activation for support
-
Reciprocal Inhibition
- Ia inhibitory interneurons: antagonist muscle relaxation
- Recurrent inhibition: Renshaw cells limit motor neuron firing
- Presynaptic inhibition: primary afferent modulation
📌 Remember: MARS for reflex testing - Monosynaptic (stretch), Antagonist (reciprocal), Recurrent (Renshaw), Segmental (withdrawal)
The spinal cord's segmental organization and tract anatomy provide the neural infrastructure connecting peripheral sensation and movement with brain control centers. This superhighway architecture enables rapid and precise information transfer while maintaining local reflex capabilities for immediate responses to environmental challenges.
Understanding spinal anatomy transforms neurological examination findings into precise anatomical localization, enabling targeted diagnostic approaches and evidence-based treatment strategies for spinal cord pathology.
🧭 Spinal Cord & Tracts — Neural Superhighway
🎯 High‑Yield Points - ⚡ Biggest Takeaways
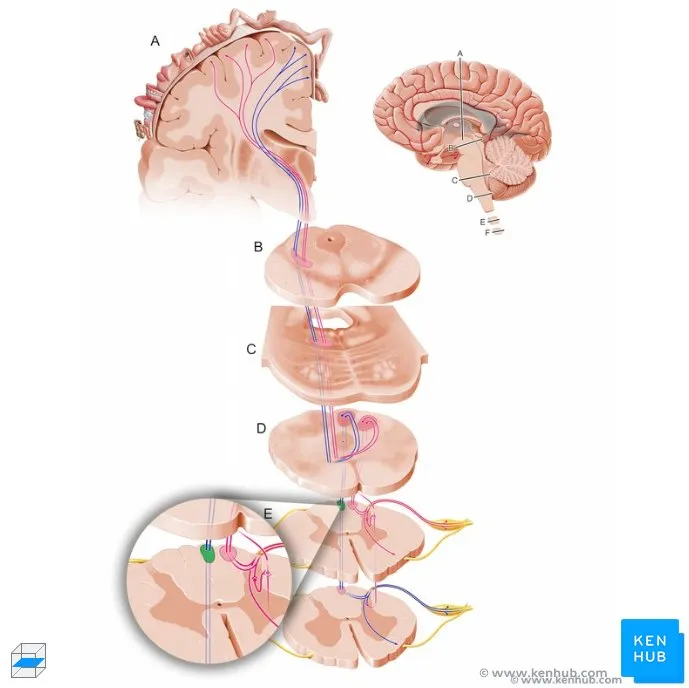
Deep Brain Localization Matrix
Master anatomical-clinical correlations through systematic pattern recognition connecting structure to function to pathology with quantitative precision.
-
Thalamic Syndrome Recognition
- VPL lesions: contralateral hemianesthesia with thalamic pain (8% incidence)
- Mediodorsal damage: executive dysfunction and personality changes
- Anterior nuclear: anterograde amnesia (Korsakoff-like syndrome)
- Pulvinar involvement: hemispatial neglect (right-sided lesions)
-
Hypothalamic Dysfunction Patterns
- Paraventricular: diabetes insipidus (ADH deficiency, >3L/day urine)
- Suprachiasmatic: circadian disruption (sleep-wake cycle loss)
- Arcuate: metabolic syndrome (obesity, diabetes)
- Lateral: aphagia/adipsia (starvation syndrome)
-
Basal Ganglia Movement Disorders
- Substantia nigra: Parkinson disease (>80% dopamine neuron loss)
- Subthalamic nucleus: hemiballismus (violent limb movements)
- Caudate: Huntington disease (CAG repeat expansion)
- Globus pallidus: dystonia (sustained muscle contractions)
📌 Remember: TVH-BG for deep brain - Thalamus (relay), Ventricles (CSF), Hypothalamus (homeostasis), Basal Ganglia (movement)
| Structure | Key Function | Lesion Syndrome | Diagnostic Test | Treatment | Prognosis |
|---|---|---|---|---|---|
| VPL thalamus | Sensory relay | Thalamic pain | MRI, sensory testing | Anticonvulsants | Chronic pain |
| Hypothalamus | Homeostasis | Diabetes insipidus | Water deprivation test | Desmopressin | Good with treatment |
| Substantia nigra | Dopamine production | Parkinson disease | DaTscan | Levodopa | Progressive |
| Subthalamic nucleus | Movement inhibition | Hemiballismus | MRI | Haloperidol | Variable |
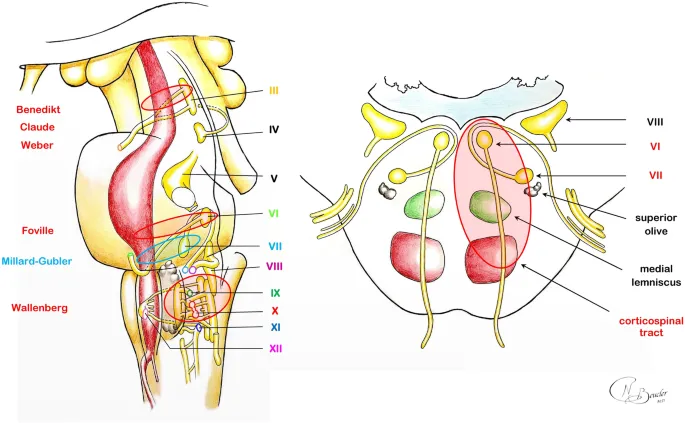
Develop systematic approaches to brainstem lesion localization using cranial nerve combinations and tract involvement patterns.
-
Midbrain Syndromes
- Weber syndrome: CN III + contralateral hemiparesis (cerebral peduncle)
- Benedikt syndrome: CN III + contralateral tremor (red nucleus)
- Parinaud syndrome: vertical gaze palsy (superior colliculus)
- Claude syndrome: CN III + contralateral ataxia (superior cerebellar peduncle)
-
Pontine Syndromes
- Millard-Gubler: CN VI + CN VII + contralateral hemiparesis
- Foville syndrome: CN VI + horizontal gaze palsy + contralateral hemiparesis
- Locked-in syndrome: bilateral ventral pons (preserved consciousness)
-
Medullary Syndromes
- Wallenberg syndrome: lateral medulla (PICA territory)
- Ipsilateral: facial pain/temperature loss, Horner syndrome
- Contralateral: body pain/temperature loss
- Medial medullary: CN XII + contralateral hemiparesis (pyramid)
- Wallenberg syndrome: lateral medulla (PICA territory)
💡 Master This: Crossed deficits (ipsilateral cranial nerve + contralateral motor/sensory) localize to brainstem - the anatomical level depends on which cranial nerves are involved
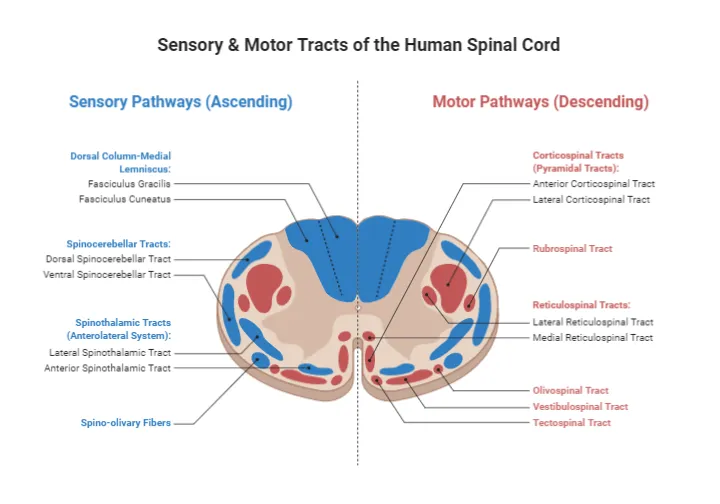
Spinal Tract Integration Mastery
Build rapid recognition patterns for spinal cord syndromes based on tract involvement and segmental anatomy.
-
Complete Cord Syndromes
- Complete transection: bilateral loss of all modalities below lesion
- Anterior cord: motor + pain/temperature loss, preserved vibration/position
- Central cord: upper extremity > lower extremity weakness (cervical)
- Brown-Séquard: ipsilateral motor + contralateral pain/temperature
-
Tract-Specific Patterns
- Dorsal column: vibration/position loss, preserved pain/temperature
- Spinothalamic: pain/temperature loss, preserved touch/vibration
- Corticospinal: spastic paralysis, hyperreflexia, Babinski positive
- Anterior horn: flaccid paralysis, areflexia, fasciculations
-
Segmental Localization Keys
- C5-C6: deltoid/biceps weakness, lateral arm numbness
- C8-T1: hand intrinsic weakness, medial arm numbness
- L4: quadriceps weakness, medial leg numbness
- S1: plantar flexor weakness, lateral foot numbness
⭐ Clinical Pearl: Syringomyelia causes dissociated sensory loss (lost pain/temperature, preserved touch/vibration) due to central cavity disrupting decussating spinothalamic fibers while sparing dorsal columns
| Syndrome | Tract Involvement | Motor Pattern | Sensory Pattern | Reflexes | Key Sign |
|---|---|---|---|---|---|
| Complete cord | All tracts | Bilateral paralysis | All modalities lost | Absent below | Sensory level |
| Brown-Séquard | Hemicord | Ipsilateral weakness | Crossed sensory | Ipsilateral ↑ | Dissociated loss |
| Central cord | Central gray | Arms > legs | Suspended sensory | Variable | Cape distribution |
| Anterior cord | Anterior 2/3 | Bilateral paralysis | Pain/temp lost | Absent | Preserved position |
Transform anatomical knowledge into clinical mastery through systematic assessment and evidence-based correlation patterns.
-
Rapid Neurological Localization
- Cortical: aphasia, neglect, seizures (focal deficits)
- Subcortical: movement disorders, memory loss (deep structures)
- Brainstem: cranial nerve + crossed motor/sensory deficits
- Spinal: sensory level, bladder/bowel, reflexes
-
Emergency Recognition Patterns
- Stroke: FAST assessment (Face, Arms, Speech, Time)
- Increased ICP: headache, vomiting, papilledema (Cushing triad)
- Spinal shock: flaccid paralysis, areflexia (temporary)
- Herniation: pupillary changes, posturing, vital sign changes
-
Rehabilitation Potential Predictors
- Motor recovery: voluntary movement within 72 hours (good prognosis)
- Sensory recovery: light touch return predicts functional improvement
- Cognitive recovery: attention and memory improvements within weeks
- Plasticity factors: age (<65 better), lesion size (<30cc better)
📌 Remember: CLBS for localization - Cortical (language/cognition), Limbic (memory/emotion), Brainstem (consciousness/cranial nerves), Spinal (motor/sensory levels)
This neuroanatomical mastery framework transforms complex neural networks into systematic clinical tools, enabling rapid localization, accurate diagnosis, and targeted therapeutic interventions based on precise anatomical understanding.
🎯 High‑Yield Points — ⚡ Biggest Takeaways
🔗 Multi-System Integration - The Neural Network Convergence
Cortico-Basal Ganglia-Thalamic Loops
Five parallel circuits connect cortical areas through basal ganglia and thalamus in closed loops that process motor, cognitive, and limbic information with distinct but overlapping functions.
-
Motor Loop Architecture
- Primary motor cortex → putamen → GPi/SNr → VL thalamus → motor cortex
- Function: movement selection and execution refinement
- Dopamine modulation: D1 receptors (direct pathway), D2 receptors (indirect)
- Pathology: Parkinson (bradykinesia), Huntington (chorea)
-
Cognitive Loops
- Dorsolateral prefrontal → caudate → GPi/SNr → VA/MD thalamus → DLPFC
- Function: working memory, executive control, cognitive flexibility
- Anterior cingulate → ventral striatum → ventral pallidum → MD thalamus
- Function: attention, conflict monitoring, error detection
-
Limbic Loop Integration
- Orbitofrontal/anterior cingulate → nucleus accumbens → ventral pallidum → MD thalamus
- Function: motivation, reward processing, addiction susceptibility
- Dopamine release: prediction error signaling (unexpected rewards)
💡 Master This: Basal ganglia disorders affect all loop functions - Parkinson patients show cognitive and emotional symptoms alongside motor deficits because dopamine depletion impacts multiple parallel circuits
Cerebellar-Cerebral Integration Networks
The cerebellum forms closed loops with cerebral cortex through pontine and thalamic relays, providing predictive control and error correction for motor, cognitive, and emotional functions.
-
Motor Cerebellum Connections
- Primary motor cortex → pontine nuclei → cerebellar cortex → dentate → VL thalamus → motor cortex
- Function: movement timing, coordination, motor learning
- Purkinje cell output: inhibitory modulation of deep nuclei
- Climbing fiber input: error signals for synaptic plasticity
-
Cognitive Cerebellum Networks
- Prefrontal cortex → pontine nuclei → lateral cerebellum → dentate → thalamus → prefrontal
- Function: working memory, language, executive control
- Cerebellar cognitive affective syndrome: posterior lobe lesions
- Autism spectrum: cerebellar developmental abnormalities (30% of cases)
-
Limbic Cerebellum Circuits
- Limbic cortex → pontine nuclei → vermis/flocculonodular → fastigial → brainstem → limbic
- Function: emotional regulation, social cognition
- Vermis lesions: autism-like behaviors, emotional dysregulation
⭐ Clinical Pearl: Cerebellar lesions cause ipsilateral deficits because double decussation (pontine + superior cerebellar peduncle) returns control to the same side - this explains why right cerebellar strokes cause right-sided ataxia
| Cerebellar Region | Cortical Partner | Function | Lesion Effect | Development | Pathology |
|---|---|---|---|---|---|
| Lateral hemispheres | Prefrontal cortex | Cognitive control | Executive dysfunction | Postnatal | Autism |
| Intermediate zone | Motor cortex | Limb coordination | Appendicular ataxia | Perinatal | Stroke |
| Vermis | Limbic cortex | Emotional regulation | Affective symptoms | Prenatal | Alcoholism |
| Flocculonodular | Vestibular cortex | Balance control | Truncal ataxia | Early prenatal | Medulloepithelioma |
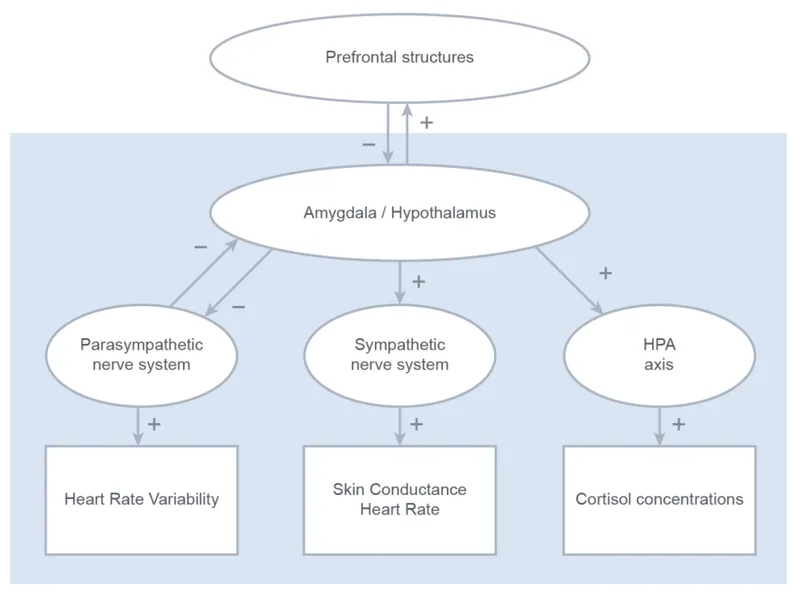
The hypothalamic-pituitary axis integrates neural and hormonal control through direct neural connections and neuroendocrine signaling, coordinating homeostasis across multiple organ systems.
-
Hypothalamic-Pituitary-Adrenal (HPA) Axis
- Stress activation: CRH → ACTH → cortisol (within minutes)
- Negative feedback: cortisol inhibits CRH and ACTH (circadian rhythm)
- Circadian control: suprachiasmatic → paraventricular → adrenal
- Pathology: Cushing (excess), Addison (deficiency)
-
Sympathetic-Adrenal Medulla System
- Sympathetic preganglionic → adrenal medulla → epinephrine/norepinephrine
- Fight-or-flight: cardiovascular, metabolic, respiratory activation
- Response time: seconds (neural) vs minutes (hormonal)
- Integration: hypothalamus coordinates both systems
-
Parasympathetic-Enteric Coordination
- Vagal control: brainstem → enteric nervous system
- Rest-and-digest: digestion, absorption, elimination
- Enteric autonomy: 500 million neurons (independent function)
- Gut-brain axis: bidirectional communication via vagus
📌 Remember: SHAPE for autonomic integration - Sympathetic (fight/flight), Hypothalamic (control), Adrenal (hormones), Parasympathetic (rest/digest), Enteric (gut brain)
Pain Processing Networks
Pain represents a complex integration of sensory, emotional, and cognitive processing across multiple brain regions, demonstrating how simple stimuli activate distributed neural networks.
-
Ascending Pain Pathways
- Spinothalamic → VPL thalamus → S1 (sensory-discriminative)
- Spinoreticular → brainstem → intralaminar thalamus → cingulate (affective)
- Spinomesencephalic → PAG → limbic structures (emotional)
-
Descending Pain Modulation
- PAG → rostral ventromedial medulla → spinal dorsal horn
- Opioid system: endorphins, enkephalins, dynorphins
- Monoamine system: serotonin, norepinephrine (antidepressant targets)
-
Chronic Pain Networks
- Default mode network alterations: persistent pain states
- Salience network hyperactivity: attention to pain signals
- Prefrontal dysfunction: cognitive control loss
💡 Master This: Chronic pain involves network reorganization rather than simple pathway activation - this explains why multimodal treatments (pharmacological + psychological + physical) prove more effective than single interventions
The nervous system's integration capabilities transform individual anatomical components into coordinated networks that enable complex behaviors, adaptive responses, and conscious experience through emergent properties arising from network interactions rather than isolated neural circuits.
🔗 Multi-System Integration — The Neural Network Convergence
🎯 Clinical Mastery Arsenal - Rapid Reference Framework
Emergency Localization Protocol
Deploy systematic assessment algorithms that rapidly distinguish cortical, subcortical, brainstem, and spinal pathology through key discriminating features.
-
60-Second Neurological Triage
- Consciousness level: GCS assessment (<8 = severe, 9-12 = moderate, 13-15 = mild)
- Pupillary responses: size, reactivity, symmetry (brainstem function)
- Motor responses: spontaneous, purposeful, posturing (cortical vs subcortical)
- Breathing pattern: regular, Cheyne-Stokes, ataxic (medullary function)
-
Rapid Localization Matrix
- Cortical signs: aphasia, neglect, seizures, focal weakness
- Subcortical signs: movement disorders, memory loss, personality change
- Brainstem signs: cranial nerve deficits + crossed motor/sensory
- Spinal signs: sensory level, bladder/bowel, reflex changes
📌 Remember: COPS for emergency localization - Cortical (language/cognition), Other subcortical (movement/memory), Pontine/brainstem (cranial nerves), Spinal (sensory levels)
Systematic Examination Framework
Execute comprehensive yet efficient neurological assessment through anatomically-organized protocols that maximize diagnostic yield while minimizing examination time.
-
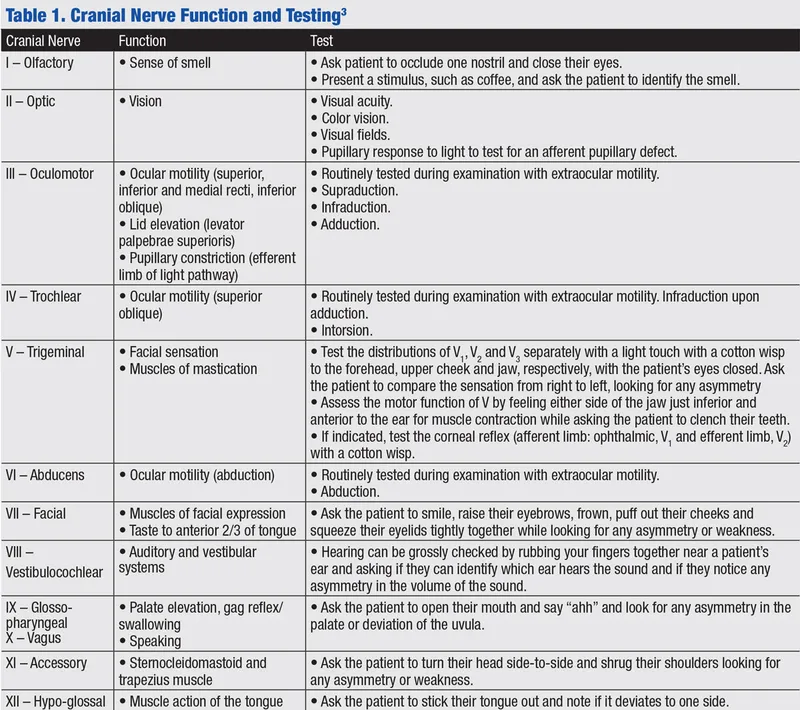
Cranial Nerve Rapid Screen
- CN I: smell identification (coffee, peppermint)
- CN II: visual acuity, fields, fundoscopy (papilledema)
- CN III, IV, VI: extraocular movements, pupils, ptosis
- CN V: facial sensation (3 divisions), jaw strength
- CN VII: facial expression (forehead sparing = UMN)
- CN VIII: hearing (Weber, Rinne), balance
- CN IX, X: gag reflex, palate elevation, voice
- CN XI: shoulder shrug, head turn (SCM, trapezius)
- CN XII: tongue protrusion (deviation toward lesion)
-
Motor System Assessment
- Inspection: atrophy, fasciculations, involuntary movements
- Tone: spasticity (UMN), rigidity (extrapyramidal), flaccidity (LMN)
- Strength: MRC scale (0-5), proximal vs distal patterns
- Reflexes: deep tendon (0-4+), pathological (Babinski, Hoffman)
- Coordination: finger-nose, heel-shin, rapid alternating movements
-
Sensory System Evaluation
- Primary modalities: light touch, pinprick, vibration, position
- Cortical sensations: two-point discrimination, stereognosis, graphesthesia
- Sensory levels: dermatomal mapping for spinal localization
- Dissociated loss: syringomyelia (pain/temperature vs touch/vibration)
⭐ Clinical Pearl: Functional neurological disorders show inconsistent examination findings - give-way weakness, non-anatomical sensory loss, and distractible symptoms that improve with suggestion or distraction
| System | Key Tests | Normal Findings | Abnormal Patterns | Localization | Time Required |
|---|---|---|---|---|---|
| Cranial nerves | Pupils, EOM, facial | Reactive, full, symmetric | Fixed, limited, asymmetric | Brainstem level | 2-3 minutes |
| Motor | Strength, tone, reflexes | 5/5, normal, 2+ | Weakness, spasticity, hyperreflexia | UMN vs LMN | 3-4 minutes |
| Sensory | Touch, pinprick, vibration | Intact, symmetric | Level, dissociated | Spinal vs cortical | 2-3 minutes |
| Coordination | Finger-nose, gait | Smooth, accurate | Dysmetria, ataxia | Cerebellar | 1-2 minutes |
| Cognitive | Orientation, memory | Alert, oriented x3 | Confusion, amnesia | Cortical/subcortical | 2-3 minutes |
Identify quantitative parameters that trigger immediate intervention or specialist consultation based on evidence-based thresholds and outcome data.
-
Intracranial Pressure Thresholds
- Normal ICP: 5-15 mmHg (adults), 3-7 mmHg (children)
- Treatment threshold: >20 mmHg for >5 minutes
- Critical threshold: >30 mmHg (herniation risk)
- CPP target: >60 mmHg (CPP = MAP - ICP)
-
Stroke Intervention Windows
- IV tPA: <4.5 hours from symptom onset
- Mechanical thrombectomy: <6 hours (anterior circulation), <24 hours (selected cases)
- NIHSS thresholds: <4 (minor), 5-15 (moderate), >15 (severe)
- Blood pressure: <185/110 for tPA eligibility
-
Spinal Cord Injury Priorities
- Methylprednisolone: <8 hours (controversial, limited evidence)
- Surgical decompression: <24 hours for incomplete injuries
- Mean arterial pressure: >85 mmHg for 7 days (spinal perfusion)
- Neurogenic shock: bradycardia + hypotension (high cervical)
💡 Master This: Time-sensitive interventions require immediate recognition - "time is brain" for stroke, "time is spine" for cord injury, and "time is pressure" for increased ICP
Evidence-Based Treatment Algorithms
Apply systematic treatment protocols based on anatomical localization and evidence-based guidelines that optimize outcomes through standardized care pathways.
-
Acute Stroke Management
- Large vessel occlusion: mechanical thrombectomy (85% recanalization)
- Small vessel disease: antiplatelet therapy (aspirin 75-100mg)
- Hemorrhagic stroke: blood pressure control (<140 systolic)
- Secondary prevention: statin (high-intensity), ACE inhibitor
-
Status Epilepticus Protocol
- First-line: lorazepam 4mg IV or diazepam 10mg IV
- Second-line: phenytoin 20mg/kg or levetiracetam 60mg/kg
- Third-line: anesthetic agents (propofol, midazolam)
- Refractory: continuous EEG monitoring, burst suppression
-
Increased ICP Management
- Head elevation: 30 degrees, midline positioning
- Osmotic therapy: mannitol 0.25-1g/kg or hypertonic saline 3%
- Hyperventilation: target PCO2 30-35 mmHg (temporary measure)
- Surgical: decompressive craniectomy for refractory cases
📌 Remember: SLIM for acute management - Stroke (thrombolysis), Lorazepam (seizures), ICP (osmotic therapy), Mannitol (brain swelling)
This clinical mastery arsenal transforms anatomical knowledge into actionable clinical tools, enabling rapid assessment, accurate localization, and evidence-based interventions that optimize patient outcomes through systematic application of neuroanatomical principles in high-stakes clinical scenarios.
🎯 Clinical Mastery Arsenal — Rapid Reference Framework
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for NEET-PG prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app







