Cerebral Localization - Brain's GPS Glitch
- Specific brain functions are linked to distinct anatomical regions. Damage to these areas results in predictable focal neurological deficits, akin to a GPS losing specific coordinates.
- Frontal Lobe: Motor control (Primary Motor Cortex), executive functions (Prefrontal Cortex), planning, personality.
- Broca's Area (Inferior Frontal Gyrus, dominant hemisphere): Expressive aphasia (difficulty producing speech). 📌 Broca = Broken speech.
- Parietal Lobe: Somatosensory perception (Primary Somatosensory Cortex), spatial orientation, language comprehension.
- Dominant (usually left): Gerstmann Syndrome (acalculia, agraphia, finger agnosia, R-L disorientation).
- Non-dominant: Contralateral hemispatial neglect.
- Temporal Lobe: Auditory processing (Primary Auditory Cortex), memory (Hippocampus), language comprehension.
- Wernicke's Area (Superior Temporal Gyrus, dominant hemisphere): Receptive aphasia (difficulty understanding speech). 📌 Wernicke's = Word salad.
- Occipital Lobe: Visual processing (Primary Visual Cortex).

⭐ A lesion in the angular gyrus of the dominant parietal lobe can cause alexia (inability to read) with agraphia (inability to write).
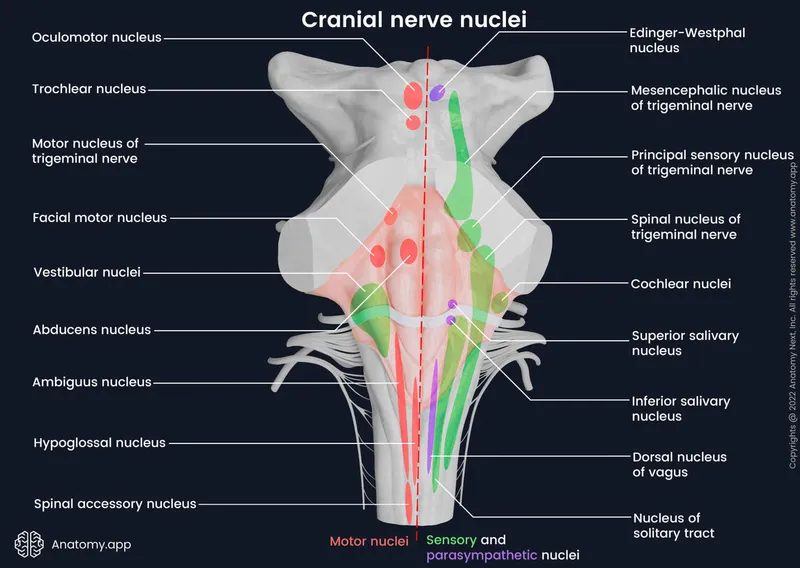
Brainstem & Cranial Nerves - Control Tower Tangle
- Components: Midbrain, Pons, Medulla Oblongata. Connects cerebrum to spinal cord.
- Cranial Nerves (CNs) by Region:
- Midbrain: CN III, IV
- Pons: CN V, VI, VII, VIII
- Medulla: CN IX, X, XI, XII
- Key Functions: Vital (respiration, cardiac, consciousness); sensory/motor relay; CN reflexes.
- 📌 CN Type Mnemonic: "Some Say Marry Money But My Brother Says Big Brains Matter More" (S=Sensory, M=Motor, B=Both).
⭐ Wallenberg Syndrome (Lateral Medullary Syndrome): PICA occlusion. Key signs: Ipsilateral Horner's syndrome, ataxia, facial pain/temp loss; Contralateral body pain/temp loss. Dysphagia & hoarseness (CN IX, X involvement).
Spinal Cord Lesions - Highway Code Broken
- Complete Transection: All modalities lost below. UMN signs below, LMN at level.
- Brown-Séquard (Hemicord):
- Ipsilateral: UMN paralysis, loss of proprioception and vibration. LMN signs at level.
- Contralateral: Loss of pain and temperature, starts 1-2 segments below.
- 📌 MVP (Motor, Vibration, Proprioception) same side; PT (Pain, Temp) opposite.
- Central Cord (Syringomyelia): "Cape-like" bilateral pain and temperature loss. Upper limbs > lower. Sacral sparing.
- Anterior Cord: Bilateral motor, pain and temperature loss. Dorsal columns (proprioception and vibration) spared. ASA occlusion.
- Posterior Cord: Loss of proprioception and vibration. Sensory ataxia. Tabes Dorsalis.

⭐ Brown-Séquard: Contralateral pain and temperature loss begins 1-2 segments below lesion due to spinothalamic tract decussation.
Neurovascular Events - Plumbing Predicaments
- Stroke Types:
- Ischemic (Clot): Occlusion (thrombotic/embolic); ~85% cases.
- Hemorrhagic (Bleed): Rupture; ~15% cases (ICH/SAH).
- Key Arterial Syndromes (Ischemic):
- ACA: Contralateral leg > arm weakness/sensory loss.
- MCA: Contralateral face/arm > leg weakness/sensory; aphasia (dom. Hemi) / neglect (non-dom. Hemi).
- PCA: Contralateral homonymous hemianopia; macular sparing common.
- Vertebrobasilar: Brainstem dysfunction (e.g., diplopia, vertigo, ataxia), cerebellar signs.
- Lacunar: Small penetrating arteries; pure motor or pure sensory stroke.
- Hemorrhagic Highlights:
- Intracerebral (ICH): Often due to hypertension.
- Subarachnoid (SAH): Typically aneurysmal; "worst headache of life".
⭐ The Middle Cerebral Artery (MCA) is the most frequently involved vessel in ischemic strokes.

High-Yield Points - ⚡ Biggest Takeaways
- Broca's area lesion (inferior frontal gyrus) causes expressive aphasia (broken speech).
- Wernicke's area lesion (superior temporal gyrus) causes receptive aphasia (fluent, meaningless speech).
- MCA stroke: most common; contralateral hemiplegia/sensory loss, aphasia (dominant hemisphere), neglect (non-dominant hemisphere).
- ACA stroke: contralateral leg > arm weakness/sensory loss; often with urinary incontinence.
- PCA stroke: contralateral homonymous hemianopia with macular sparing; visual agnosia.
- Wallenberg syndrome (PICA occlusion): ipsilateral facial sensory loss, contralateral body pain/temperature loss; dysphagia, Horner's syndrome.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

