Back

On this page
🏗️ The Spinal Architecture: Engineering Marvel of Human Structure
Your back is simultaneously a weight-bearing column, a protective vault for your spinal cord, and a dynamic system enabling everything from delicate finger movements to explosive athletic power. This lesson guides you through the spine's architectural brilliance, the layered muscular networks that stabilize and mobilize it, the neural pathways that make precision control possible, and the vascular systems sustaining it all. You'll trace how this complexity emerges during development and then apply your understanding to diagnose herniated discs, spinal fractures, and nerve compression syndromes that you'll encounter throughout clinical practice.
📌 Remember: CLOTS for vertebral regions - Cervical (7), Lumbar (5), Thoracic (12), Sacral (5 fused). Total mobile segments: 24 vertebrae enabling spinal flexibility.
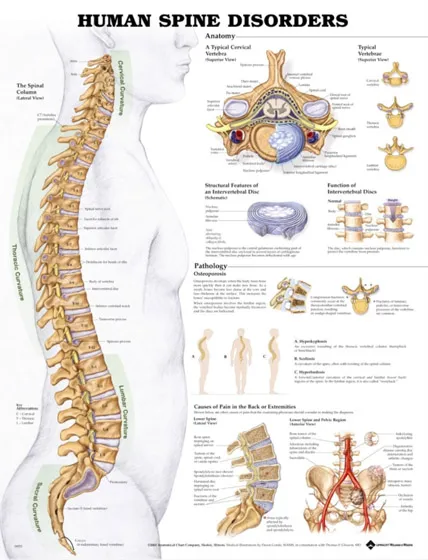
The vertebral column's four physiological curves create optimal load distribution: cervical lordosis (20-40°), thoracic kyphosis (20-45°), lumbar lordosis (40-60°), and sacral kyphosis (fixed). These curves transform the spine from a rigid pillar into a flexible shock-absorbing system capable of handling 3-5x body weight during normal activities.
-
Cervical Region (C1-C7)
- Atlas (C1): No vertebral body, supports 15-pound head weight
- Axis (C2): Odontoid process enables 50° rotation each direction
- C3-C7: Bifid spinous processes, transverse foramina for vertebral arteries
- Vertebral artery diameter: 3-4mm, critical for 20% of brain blood supply
- C7 (vertebra prominens): First palpable spinous process, surgical landmark
-
Thoracic Region (T1-T12)
- Costal facets for rib articulation: 24 ribs creating thoracic cage
- Spinous processes: Long, overlapping, angled 45-60° downward
- Vertebral canal diameter: 15-20mm (narrowest spinal region)
- T4-T9: Watershed zone with poorest vascular supply
- T10-T12: Transition to lumbar characteristics
| Region | Vertebrae | Curve Type | Angle Range | Key Features | Clinical Significance |
|---|---|---|---|---|---|
| Cervical | C1-C7 | Lordosis | 20-40° | Bifid processes, foramina | Vertebral artery, cord injury |
| Thoracic | T1-T12 | Kyphosis | 20-45° | Costal facets, long processes | Rib cage, respiratory function |
| Lumbar | L1-L5 | Lordosis | 40-60° | Large bodies, short processes | Weight bearing, disc herniation |
| Sacral | S1-S5 | Kyphosis | Fixed | Fused vertebrae | Pelvic articulation, childbirth |
| Coccygeal | Co1-Co4 | Variable | Flexible | Rudimentary segments | Tailbone trauma, sitting pain |
- Lumbar Region (L1-L5)
- Largest vertebral bodies: Support 60% of total body weight
- Spinous processes: Short, thick, horizontal orientation
- L4-L5 and L5-S1: 90% of disc herniations occur here
- L5-S1 disc: Largest intervertebral disc, 15mm average height
- Lumbar canal diameter: 25-30mm, accommodates cauda equina
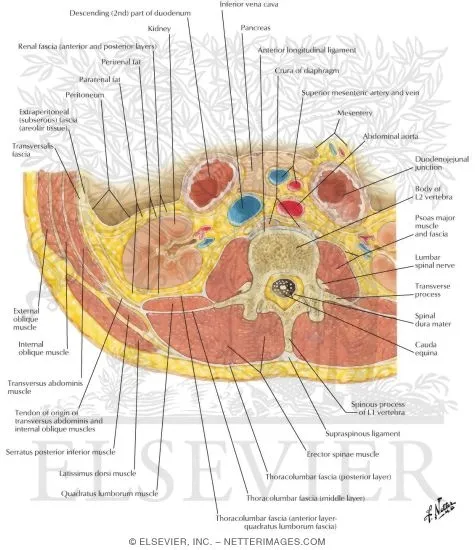
💡 Master This: Vertebral body size increases caudally to handle progressive weight loading. L5 vertebral body is 5x larger than C3, reflecting biomechanical demands. This size gradient predicts fracture patterns and surgical approach complexity.
The intervertebral disc structure enables 6 degrees of freedom movement while maintaining structural integrity. Nucleus pulposus (80% water in youth, 70% by age 70) acts as hydraulic shock absorber, while annulus fibrosus (15 concentric layers) provides tensile strength up to 500 pounds per square inch.
📌 Remember: DISC components - Disc height decreases with age, Innervation only in outer annulus, Sinuvertebral nerve supplies posterior disc, Center (nucleus) is avascular after age 20.
Understanding spinal architecture provides the foundation for recognizing how structural variations create clinical vulnerabilities, setting the stage for exploring the intricate muscular systems that animate this remarkable framework.
🏗️ The Spinal Architecture: Engineering Marvel of Human Structure
⚡ The Muscular Powerhouse: Back's Dynamic Control Network
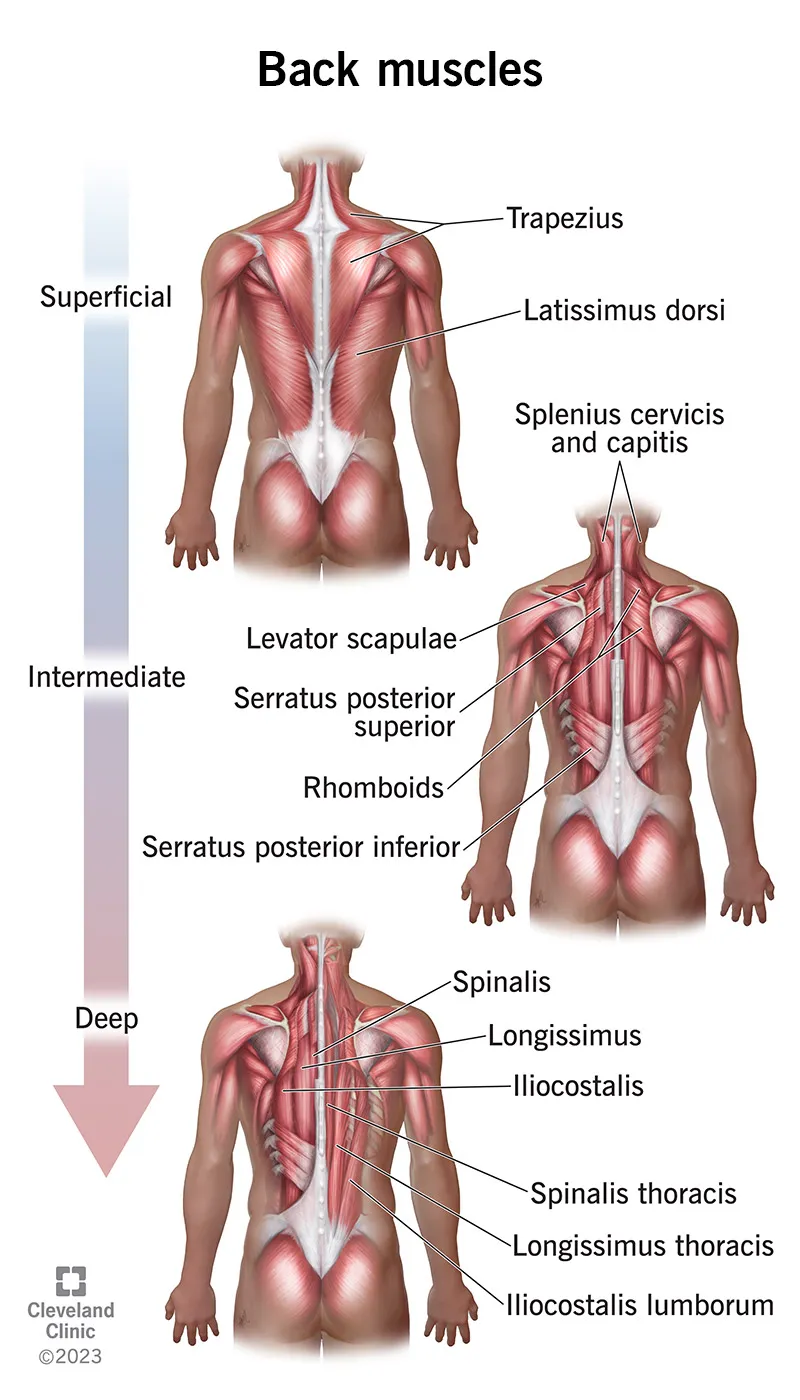
📌 Remember: SLIM for superficial back muscles - Serratus posterior, Latissimus dorsi, Intercostals (external), Muscles of scapula (trapezius, rhomboids). These muscles primarily move the upper extremity, not the spine itself.
-
Superficial Layer (Appendicular Muscles)
- Trapezius: 4 functional parts, innervated by cranial nerve XI
- Upper fibers: Elevate scapula 45°, support 15-pound head weight
- Middle fibers: Retract scapula, counteract forward head posture
- Lower fibers: Depress scapula, enable overhead reaching >120°
- Latissimus dorsi: Largest back muscle, 30cm width at base
- Adduction power: 60 pounds of force, critical for climbing/pulling
- "Swimmer's muscle": Generates 80% of freestyle stroke power
- Trapezius: 4 functional parts, innervated by cranial nerve XI
-
Intermediate Layer (Respiratory Muscles)
- Serratus posterior superior: Elevates ribs 2-5 during inspiration
- Serratus posterior inferior: Depresses ribs 9-12 during forced expiration
- Respiratory contribution: 15% of total ventilatory capacity
- Activation increases 300% during exercise-induced hyperpnea
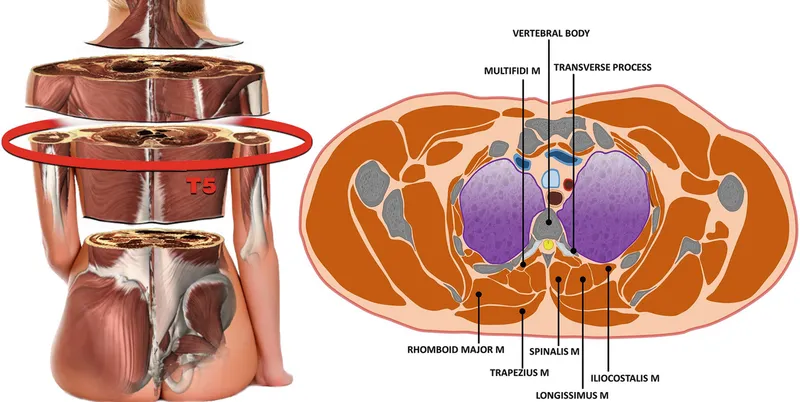
| Muscle Group | Primary Function | Innervation | Force Output | Clinical Significance |
|---|---|---|---|---|
| Trapezius | Scapular movement | CN XI, C3-C4 | 60 lbs | Torticollis, shoulder impingement |
| Latissimus dorsi | Arm adduction | Thoracodorsal (C6-C8) | 80 lbs | Climbing strength, surgical flaps |
| Erector spinae | Spinal extension | Posterior rami | 200 lbs | Low back pain, postural control |
| Multifidus | Segmental stability | Posterior rami | 40 lbs | Core stability, chronic pain |
| Suboccipital | Head positioning | C1 posterior ramus | 15 lbs | Tension headaches, vertigo |
- Deep Layer (True Back Muscles)
- Erector spinae: Three columns spanning entire spine
- Iliocostalis: Lateral column, rib attachments, 45° lateral flexion
- Longissimus: Middle column, transverse processes, primary extensor
- Spinalis: Medial column, spinous processes, fine-tuning control
- Transversospinales: Segmental stabilizers with proprioceptive function
- Multifidus: 2-4 segment span, core stability champion
- Rotatores: 1-2 segment span, proprioceptive sensors
- Semispinalis: 4-6 segment span, cervical extension specialist
- Erector spinae: Three columns spanning entire spine
💡 Master This: Deep back muscles are 80% Type I fibers (slow-twitch endurance), while superficial muscles are 60% Type II fibers (fast-twitch power). This fiber distribution explains why postural muscles fatigue slowly but movement muscles generate high force rapidly.
- Suboccipital Triangle (Precision Head Control)
- Four small muscles controlling atlantooccipital and atlantoaxial joints
- Rectus capitis posterior major/minor: 15° extension range
- Obliquus capitis superior/inferior: 45° rotation each direction
- Proprioceptive density: 36 muscle spindles per gram (highest in body)
- Tension headache correlation: 90% involve suboccipital muscle spasm
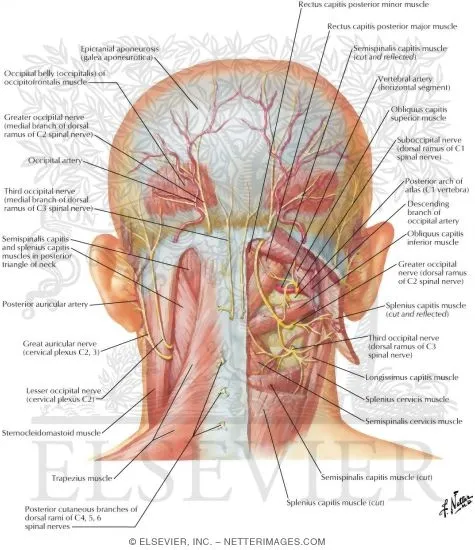
📌 Remember: RORO for suboccipital muscles - Rectus capitis posterior major, Obliquus capitis superior, Rectus capitis posterior minor, Obliquus capitis inferior. All innervated by C1 posterior ramus (suboccipital nerve).
The fascial system integrates muscular function through three primary layers: superficial fascia (skin attachment), thoracolumbar fascia (muscle compartmentalization), and deep cervical fascia (neurovascular protection). The thoracolumbar fascia alone provides 30% of spinal stability through its posterior, middle, and anterior layers.
⭐ Clinical Pearl: Thoracolumbar fascia tension increases 40% during lifting, creating hydraulic amplification of muscle force. Fascial restrictions reduce this amplification by 60%, explaining why manual therapy targeting fascia improves lifting capacity by 25% in chronic pain patients.
This muscular architecture creates the dynamic framework for spinal movement and stability, leading us to explore how the nervous system coordinates these complex muscular interactions through sophisticated neural control mechanisms.
⚡ The Muscular Powerhouse: Back's Dynamic Control Network
🧠 Neural Command Center: Back's Intelligent Control System
📌 Remember: DAMP for spinal nerve components - Dorsal root (sensory), Anterior root (motor), Mixed spinal nerve (both), Posterior and anterior rami (distribution branches). Each spinal nerve contains 8,000-12,000 individual nerve fibers.
-
Spinal Nerve Formation (Segmental Organization)
- Dorsal root: Sensory fibers from skin, joints, muscles
- Dorsal root ganglion: Contains 15,000-20,000 sensory cell bodies
- A-delta fibers: 2-5 m/s conduction, sharp pain sensation
- C-fibers: 0.5-2 m/s conduction, dull aching pain
- Ventral root: Motor fibers to skeletal muscles
- Alpha motor neurons: 50-120 m/s conduction, muscle contraction
- Gamma motor neurons: 10-50 m/s conduction, muscle spindle control
- Dorsal root: Sensory fibers from skin, joints, muscles
-
Posterior Rami (True Back Innervation)
- Medial branches: Supply deep back muscles and skin
- Lateral branches: Supply superficial muscles and lateral skin
- Segmental pattern: Each ramus supplies 2-3 vertebral levels
- Overlap zones: 50% sensory overlap between adjacent segments
| Nerve Type | Fiber Diameter | Conduction Speed | Function | Clinical Testing |
|---|---|---|---|---|
| A-alpha | 12-20 μm | 70-120 m/s | Motor, proprioception | Reflexes, position sense |
| A-beta | 5-12 μm | 30-70 m/s | Touch, vibration | Light touch, tuning fork |
| A-delta | 2-5 μm | 12-30 m/s | Sharp pain, cold | Pinprick, cold sensation |
| B-fibers | 1-3 μm | 3-15 m/s | Autonomic preganglionic | Heart rate, sweating |
| C-fibers | 0.4-1.2 μm | 0.5-2 m/s | Dull pain, warmth | Thermal pain threshold |
-
Autonomic Innervation (Sympathetic Control)
- Sympathetic chain: T1-L2 preganglionic neurons
- Gray rami communicantes: All spinal levels receive sympathetic fibers
- Vascular control: Smooth muscle in spinal arteries
- Vasoconstriction: Reduces spinal blood flow by 40% during stress
- Pain modulation: Sympathetic blocks reduce chronic pain by 60%
-
Reflex Circuits (Protective Mechanisms)
- Stretch reflexes: Monosynaptic pathways, 30-50ms response time
- Withdrawal reflexes: Polysynaptic pathways, 100-200ms response
- Crossed extensor reflexes: Bilateral coordination for balance
- Muscle spindle density: 4-7 per gram in deep back muscles
- Golgi tendon organs: 10-15 per muscle, monitor muscle tension
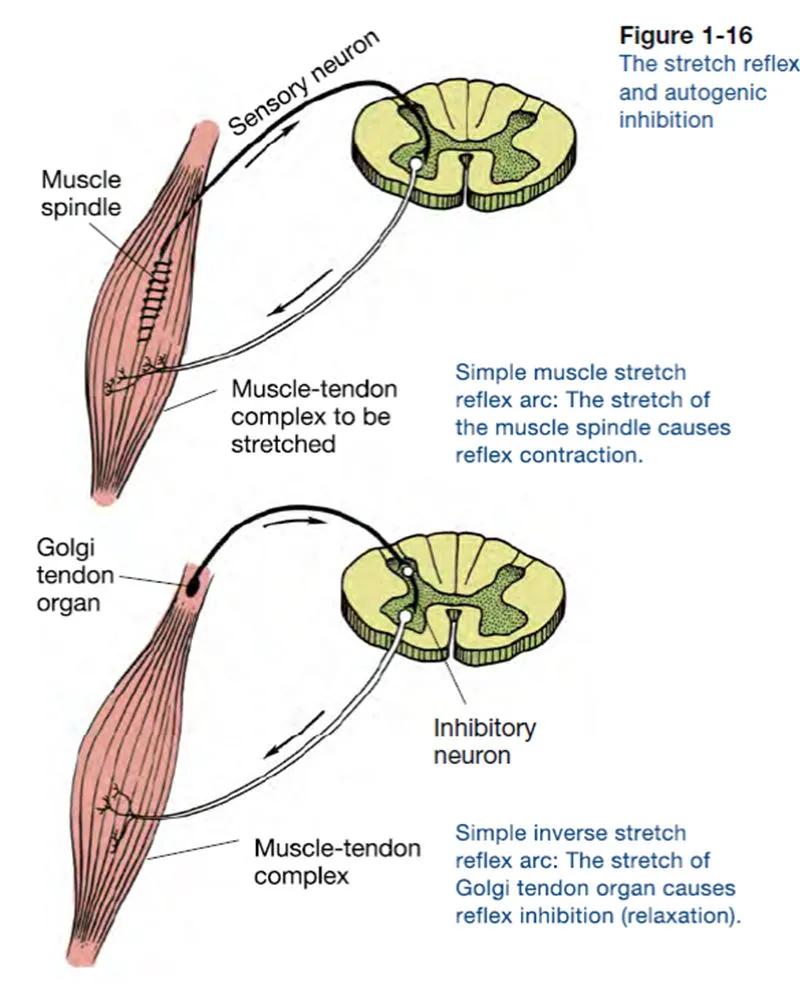
💡 Master This: Proprioceptive dysfunction occurs within 48 hours of spinal injury, reducing position sense accuracy by 40%. This explains why balance training is crucial for preventing re-injury - it restores proprioceptive acuity to within 85% of normal values.
- Pain Processing (Nociceptive Pathways)
- Nociceptors: Free nerve endings in muscles, ligaments, discs
- Substantia gelatinosa: Lamina II of dorsal horn, gate control mechanism
- Ascending tracts: Spinothalamic (pain/temperature), spinoreticular (arousal)
- Central sensitization: NMDA receptor upregulation increases pain 300%
- Descending inhibition: Serotonin/norepinephrine reduces pain by 50%
📌 Remember: PQRST for pain pathway - Peripheral nociceptor activation, Quality determined by fiber type, Relay in dorsal horn, Spinothalamic tract ascension, Thalamic processing and cortical perception.
The sinuvertebral nerve (recurrent meningeal nerve) provides critical innervation to posterior longitudinal ligament, outer annulus fibrosus, and dura mater. This mixed nerve (sympathetic + sensory) explains why disc pathology creates both local pain and autonomic symptoms like nausea and sweating.
⭐ Clinical Pearl: Sinuvertebral nerve compression during disc herniation activates sympathetic reflexes, causing muscle spasm in paraspinal muscles up to 3 levels above and below the lesion. This explains the regional muscle guarding pattern seen in acute disc injuries.
This neural control system provides the foundation for understanding how sensory input guides motor output, setting the stage for exploring the vascular networks that sustain this complex neurological machinery.
🧠 Neural Command Center: Back's Intelligent Control System
🩸 Vascular Highways: Back's Critical Supply Network
📌 Remember: VIAL for spinal arterial supply - Vertebral arteries (cervical), Intercostal arteries (thoracic), Artery of Adamkiewicz (critical thoracolumbar), Lumbar arteries (lower spine). The artery of Adamkiewicz supplies 60% of lower spinal cord blood flow.
-
Arterial Supply Architecture (Three-Tier System)
- Anterior spinal artery: Single vessel, supplies anterior 2/3 of cord
- Diameter: 0.2-0.8mm, most vulnerable to ischemia
- Perfusion pressure: 50-70 mmHg, critical threshold 40 mmHg
- Watershed zone: T4-T9, poorest collateral circulation
- Posterior spinal arteries: Paired vessels, supply posterior 1/3 of cord
- Diameter: 0.1-0.4mm, better collateral network
- Anastomotic connections: Every 2-3 segments
- Anterior spinal artery: Single vessel, supplies anterior 2/3 of cord
-
Regional Vascular Patterns (Segmental Organization)
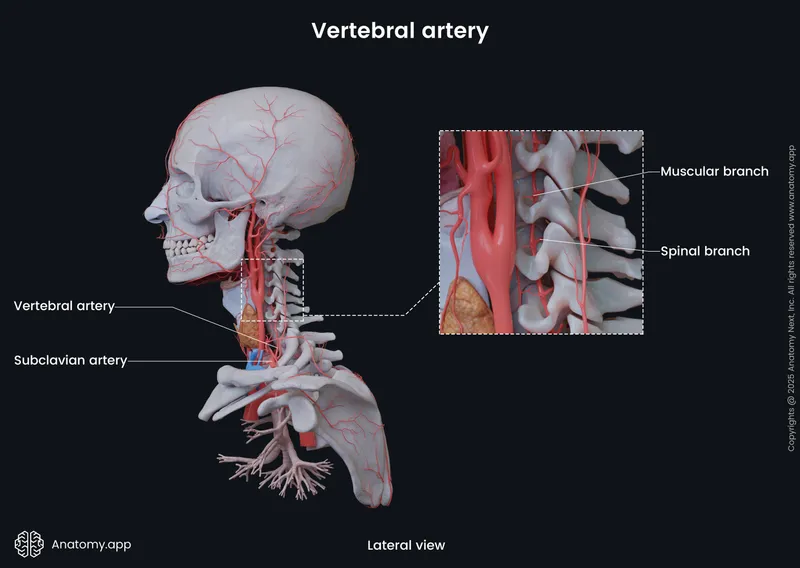
- Cervical region: Vertebral arteries provide 80% of blood supply
- Vertebral artery diameter: 3-4mm, 300ml/min flow rate
- Muscular branches: Supply deep cervical muscles
- Spinal branches: C1-C6 segmental supply
- Thoracic region: Intercostal arteries from aorta
- T1-T12: Paired segmental arteries, 10-15ml/min each
- Critical watershed: T4-T9, 50% reduced perfusion
- Cervical region: Vertebral arteries provide 80% of blood supply
| Vascular Territory | Primary Source | Flow Rate | Watershed Risk | Clinical Significance |
|---|---|---|---|---|
| Cervical (C1-C7) | Vertebral arteries | 300 ml/min | Low | Vertebrobasilar insufficiency |
| Upper thoracic (T1-T6) | Intercostal arteries | 80 ml/min | Moderate | Anterior cord syndrome |
| Lower thoracic (T7-T12) | Adamkiewicz artery | 120 ml/min | High | Paraplegia risk |
| Lumbar (L1-L5) | Lumbar arteries | 100 ml/min | Moderate | Cauda equina syndrome |
| Sacral (S1-S5) | Lateral sacral arteries | 60 ml/min | Low | Bowel/bladder function |
-
Venous Drainage (Valveless System)
- Internal vertebral venous plexus: Batson's plexus, valveless system
- Epidural space: Extensive venous network, low pressure system
- Bidirectional flow: Enables metastatic spread from pelvis/abdomen
- Pressure changes: Valsalva maneuver increases pressure 300%
- External vertebral venous plexus: Superficial drainage system
- Posterior external: Drains to azygos/hemiazygos systems
- Anterior external: Drains to caval system
- Internal vertebral venous plexus: Batson's plexus, valveless system
-
Microvascular Architecture (Tissue Level)
- Capillary density: 400-600 per mm² in gray matter
- Blood-brain barrier: Tight junctions, selective permeability
- Autoregulation: Maintains constant perfusion despite pressure changes
- Autoregulation range: 50-150 mmHg mean arterial pressure
- CO₂ reactivity: 4% flow change per mmHg CO₂ change
💡 Master This: Batson's venous plexus lacks valves, creating bidirectional flow that explains metastatic patterns. Prostate cancer spreads to lumbar spine in 90% of bone metastases because increased abdominal pressure reverses venous flow, carrying cancer cells retrograde to vertebral bodies.
- Vascular Pathophysiology (Clinical Correlations)
- Spinal cord ischemia: Anterior cord syndrome in 85% of cases
- Motor loss: Complete paralysis below lesion level
- Pain/temperature loss: Spinothalamic tract involvement
- Preserved: Posterior column function (position/vibration)
- Vascular malformations: AVMs cause progressive myelopathy
- Steal phenomenon: 50% reduction in normal cord perfusion
- Venous hypertension: Chronic ischemia and gliosis
- Spinal cord ischemia: Anterior cord syndrome in 85% of cases
📌 Remember: ASIA for anterior spinal artery syndrome - Anterior cord involvement, Spinothalamic tract loss, Ischemic motor paralysis, Anterior 2/3 of cord affected. Posterior columns (position/vibration) are spared because they receive posterior spinal artery supply.
⭐ Clinical Pearl: Spinal cord perfusion pressure = Mean arterial pressure - Cerebrospinal fluid pressure. Normal SCPP is 60-70 mmHg. Values <50 mmHg for >30 minutes cause irreversible ischemic damage to anterior horn cells.
This vascular architecture provides the metabolic foundation for spinal function, leading us to explore how developmental processes create these complex anatomical relationships and their clinical implications.
🩸 Vascular Highways: Back's Critical Supply Network
🧬 Developmental Blueprint: Spine's Embryonic Engineering
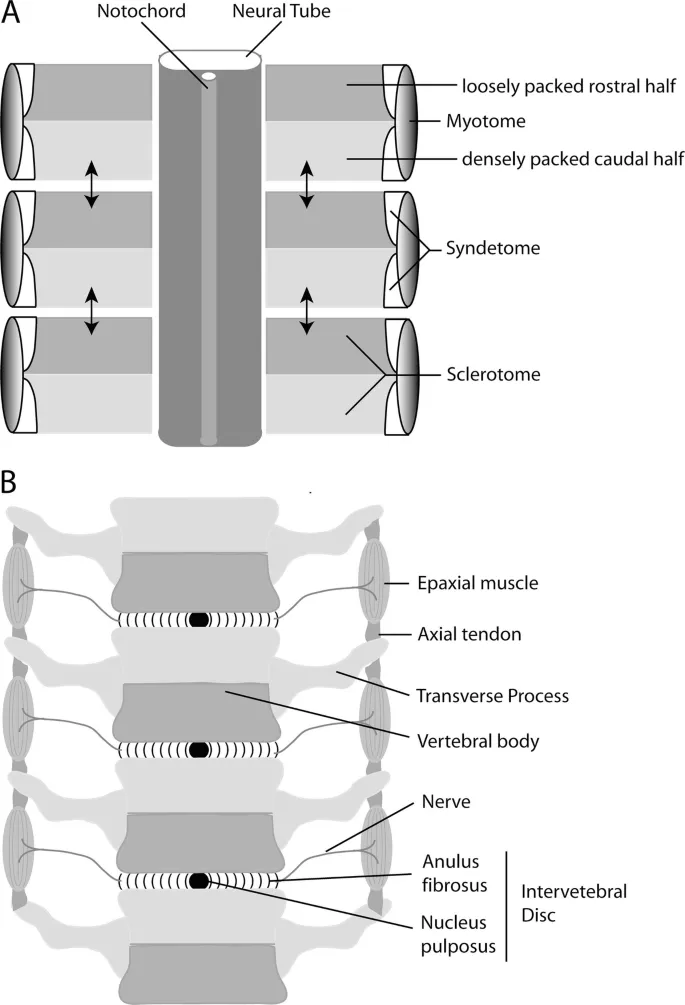
📌 Remember: SONIC for spinal development - Somites form segmental blocks, Osteoblasts from sclerotome, Notochord guides development, Intervertebral discs from resegmentation, Chondrocytes create cartilage template. Development occurs weeks 4-8 of gestation.
-
Early Development (Weeks 3-4)
- Notochord formation: Day 16-18, establishes axial organization
- Notochord length: 2.5mm at 4 weeks, guides neural tube formation
- Signaling molecules: Sonic hedgehog, BMP-4, Wnt proteins
- Regression pattern: Notochord persists as nucleus pulposus in discs
- Somite formation: Day 20-30, creates 42-44 somite pairs
- Somite rate: 3 pairs per day, cranial-to-caudal progression
- Sclerotome differentiation: Ventromedial somite portion
- Notochord formation: Day 16-18, establishes axial organization
-
Resegmentation Process (Weeks 4-5)
- Sclerotome splitting: Each somite divides into cranial and caudal halves
- Cranial half: Loose mesenchyme, forms intervertebral disc
- Caudal half: Dense mesenchyme, forms vertebral body
- Resegmentation: Cranial + caudal from adjacent somites = one vertebra
- Spinal nerve positioning: Intersegmental location enables mobility
- Sclerotome splitting: Each somite divides into cranial and caudal halves
| Developmental Stage | Timing | Key Events | Clinical Significance |
|---|---|---|---|
| Notochord formation | Week 3 | Axial organization | Neural tube defects |
| Somite formation | Week 4 | Segmental blocks | Vertebral number anomalies |
| Resegmentation | Week 5 | Vertebral boundaries | Spina bifida, block vertebrae |
| Chondrification | Week 6-8 | Cartilage template | Skeletal dysplasias |
| Primary ossification | Week 8-12 | Bone formation | Growth disturbances |
-
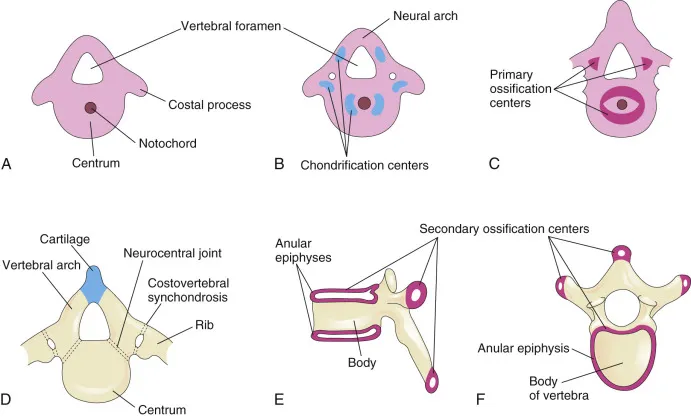
Chondrification (Weeks 6-8)
- Three primary centers: Body and two neural arches
- Vertebral body: Single center, appears week 6
- Neural arches: Paired centers, appear week 7-8
- Cartilage template: Hyaline cartilage, blueprint for bone formation
- Regional variations: Atlas has no body center, axis has odontoid center
- Three primary centers: Body and two neural arches
-
Ossification Patterns (Weeks 8-25)
- Primary ossification: 3 centers per vertebra (body + 2 arches)
- Cervical: Weeks 9-10, neural arches fuse by age 3
- Thoracic: Weeks 10-11, spinous processes fuse by age 5
- Lumbar: Weeks 11-12, laminae fuse by age 6
- Secondary ossification: 5 centers appear during puberty
- Vertebral endplates: Age 15-16, complete by age 25
- Spinous/transverse processes: Age 16-18, complete by age 25
- Primary ossification: 3 centers per vertebra (body + 2 arches)
💡 Master This: Primary curves (thoracic/sacral kyphosis) develop in utero from flexed fetal position. Secondary curves (cervical/lumbar lordosis) develop postnatally - cervical lordosis when infant lifts head (3-4 months), lumbar lordosis when child walks (12-18 months).
- Congenital Anomalies (Developmental Failures)
- Spina bifida: Neural arch fusion failure, 1 in 1,000 births
- Spina bifida occulta: L5-S1 most common, 10% of population
- Meningocele: Meningeal herniation, normal neural function
- Myelomeningocele: Cord herniation, neurological deficits
- Vertebral number anomalies: Somite formation errors
- Cervical ribs: C7 develops rib, 0.5% incidence
- Lumbarization: S1 becomes lumbar-like, 4% incidence
- Sacralization: L5 fuses to sacrum, 6% incidence
- Spina bifida: Neural arch fusion failure, 1 in 1,000 births
📌 Remember: VACTERL association includes vertebral anomalies - Vertebral defects, Anal atresia, Cardiac defects, Tracheoesophageal fistula, Esophageal atresia, Renal anomalies, Limb defects. Vertebral anomalies occur in 60% of VACTERL cases.
- Growth and Maturation (Birth to Adulthood)
- Vertebral height: Increases 300% from birth to skeletal maturity
- Disc height: 50% of adult height** achieved by age 8
- Spinal length: 60cm at birth, 70cm at age 18
- Growth velocity: Peak during pubertal growth spurt (age 11-14)
- Growth completion: Vertebral endplates fuse by age 25
⭐ Clinical Pearl: Adolescent idiopathic scoliosis develops during peak growth velocity when vertebral growth outpaces muscular development. Risser sign (iliac crest ossification) predicts remaining growth - Risser 0-2 indicates high progression risk, Risser 4-5 indicates growth completion.
Understanding developmental principles provides the foundation for recognizing how embryological processes influence adult pathology, setting the stage for exploring the clinical applications that transform this knowledge into diagnostic and therapeutic expertise.
🧬 Developmental Blueprint: Spine's Embryonic Engineering
🎯 Clinical Mastery Arsenal: Back Expertise in Action
📌 Remember: SPINE for systematic back examination - Standing posture assessment, Palpation of landmarks, Inspection for deformity, Neurological testing, Examination of movement patterns. Complete examination takes 8-10 minutes but yields 85% diagnostic accuracy.
| Clinical Tool | Application | Sensitivity | Specificity | Clinical Value |
|---|---|---|---|---|
| Straight leg raise | L4-S1 radiculopathy | 91% | 26% | High sensitivity, low specificity |
| Crossed SLR | Disc herniation | 29% | 88% | High specificity for large herniations |
| Spurling test | Cervical radiculopathy | 95% | 94% | Excellent for C-spine nerve compression |
| Slump test | Neural tension | 84% | 83% | Good for neurodynamic dysfunction |
| FABER test | SI joint pathology | 77% | 100% | Excellent specificity for SI problems |
- Red flag symptoms: <1% of back pain but 100% require immediate evaluation
- Cauda equina: Saddle anesthesia + bladder dysfunction
- Infection: Fever >38°C + elevated ESR >50
- Malignancy: Age >50 + night pain + weight loss >10 pounds
- Fracture: Age >70 + trauma + steroid use
- Neurological levels: Precise localization guides treatment
- L4: Knee extension weakness, patellar reflex loss
- L5: Dorsiflexion weakness, no reliable reflex
- S1: Plantarflexion weakness, Achilles reflex loss
- Diagnostic Imaging Guidelines (Evidence-Based Protocols)
- Plain radiographs: First-line for trauma, deformity, infection
- Sensitivity: 60% for fractures, 40% for infections
- Cost-effectiveness: $200 vs $2,000 for MRI
- MRI indications: Neurological deficits or red flag symptoms
- Disc herniation: 95% sensitivity, 72% specificity
- Spinal stenosis: 90% sensitivity, 76% specificity
- False positives: 30% of asymptomatic adults have disc abnormalities
- Plain radiographs: First-line for trauma, deformity, infection
⭐ Clinical Pearl: Yellow flags (psychosocial factors) predict chronic disability better than anatomical findings. Fear-avoidance beliefs, depression scores >14, and job dissatisfaction increase chronicity risk by 400%. Early cognitive-behavioral intervention reduces chronic pain by 50%.
-
Treatment Algorithms (Evidence-Based Protocols)
- Acute back pain (<6 weeks)
- First-line: NSAIDs + activity modification (not bed rest)
- Muscle relaxants: Short-term use (<2 weeks), limited evidence
- Return to activity: Gradual increase, avoid bed rest >2 days
- Chronic back pain (>12 weeks)
- Multimodal approach: Exercise + manual therapy + education
- Injection therapy: Epidural steroids for radiculopathy
- Surgery consideration: >6 months conservative failure + anatomical correlation
- Acute back pain (<6 weeks)
-
Surgical Indications (Precise Criteria)
- Absolute indications: Cauda equina, progressive neurological deficit
- Relative indications: Persistent radiculopathy + anatomical correlation
- Disc herniation: >6 weeks conservative failure + concordant imaging
- Spinal stenosis: Neurogenic claudication + central canal <10mm²
- Spondylolisthesis: >50% slip + neurological symptoms
💡 Master This: Surgical success correlates with patient selection, not surgical technique. Appropriate candidates achieve 85% satisfaction rates, while inappropriate candidates have 40% satisfaction regardless of technical excellence. Psychosocial screening is mandatory for optimal outcomes.
- Rapid Assessment Tools (Clinical Efficiency)
- Oswestry Disability Index: 10 questions, 2 minutes, predicts functional outcome
- Numeric Pain Rating Scale: 0-10 scale, 30 seconds, tracks treatment response
- STarT Back Tool: 9 questions, 1 minute, stratifies treatment approach
- Low risk: Self-management + education
- Medium risk: Physiotherapy + exercise
- High risk: Multidisciplinary + psychological support
📌 Remember: SOCRATES for pain assessment - Site, Onset, Character, Radiation, Associations, Time course, Exacerbating factors, Severity. Systematic pain assessment identifies 95% of serious pathology through history alone.
⭐ Clinical Pearl: Centralization phenomenon (pain moves from leg to back during McKenzie exercises) predicts 90% success with conservative treatment. Peripheralization (pain moves from back to leg) indicates poor prognosis and potential surgical candidacy.
🎯 Clinical Mastery Arsenal: Back Expertise in Action
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for NEET-PG prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app










