Abdomen

On this page
🏗️ Abdominal Architecture: The Body's Engineering Marvel
The abdomen is where anatomy meets emergency, where subtle patterns reveal life-threatening pathology, and where your clinical reasoning must integrate multiple organ systems simultaneously. You'll master the architectural layers that protect vital structures, decode the functional dynamics of pain and peritonitis, build pattern recognition skills that distinguish surgical emergencies from medical mimics, and develop systematic approaches to diagnosis and treatment that work under pressure. This lesson transforms the abdomen from an intimidating black box into your most confident clinical domain.
📌 Remember: WALL - Walls (4 regions), Aorta (major vessel), Layers (fascial planes), Lumbar (posterior reference) - The abdomen's 4 walls (anterior, posterior, superior, inferior) create a protective cavity housing >20 organs with 3 distinct peritoneal relationships
The abdominal cavity spans from the diaphragm superiorly to the pelvic inlet inferiorly, encompassing approximately 5,000 cubic centimeters of space in adults. This volume accommodates organs with dramatically different functions, from the liver's 500+ metabolic processes to the kidneys' filtration of 180 liters daily. The cavity's organization follows precise anatomical principles that enable surgical access, diagnostic imaging interpretation, and clinical examination.
| Abdominal Region | Primary Contents | Clinical Access | Imaging Plane | Surgical Approach | Pathology Risk |
|---|---|---|---|---|---|
| Right Upper Quadrant | Liver, gallbladder, right kidney | Subcostal incision | Coronal/sagittal | Laparoscopic preferred | Biliary disease 85% |
| Left Upper Quadrant | Spleen, stomach, left kidney | Left subcostal | Axial/coronal | Open vs laparoscopic | Splenic trauma 60% |
| Right Lower Quadrant | Appendix, cecum, ovary | McBurney's point | Axial preferred | Laparoscopic standard | Appendicitis 7% lifetime |
| Left Lower Quadrant | Sigmoid, left ovary | Pfannenstiel | Sagittal/axial | Minimally invasive | Diverticulitis 50% >60yrs |
| Epigastrium | Pancreas, duodenum | Upper midline | Axial/coronal | Complex exposure | Pancreatitis 15% recurrence |
The abdominal wall's muscular architecture creates a dynamic pressure system capable of generating >200 mmHg during Valsalva maneuvers while maintaining baseline pressures of 5-7 mmHg. This pressure regulation system enables:
- Respiratory assistance - Abdominal muscles contribute 30% of expiratory force
- Postural stability - Core muscles provide 40% of spinal support
- Visceral protection - Muscular walls absorb >80% of blunt trauma energy
- Elimination assistance - Increased pressure facilitates defecation and urination
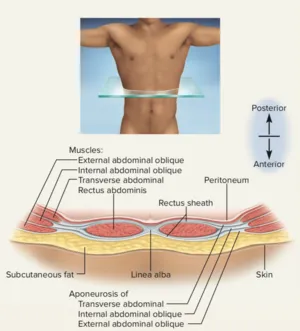
💡 Master This: Abdominal wall integrity depends on fascial continuity - the transversalis fascia forms the deepest layer, creating the critical barrier between abdominal contents and wall structures. Fascial defects account for >95% of hernia formations, making fascial anatomy essential for surgical repair success.
- Anterior Wall Components:
- Skin and subcutaneous tissue - Contains Camper's (fatty) and Scarpa's (membranous) fascial layers
- External oblique muscle - Fibers run inferomedially, forms inguinal ligament
- Internal oblique muscle - Fibers run superomedially, contributes to conjoint tendon
- Rectus abdominis - 8 tendinous intersections create "six-pack" appearance
- Pyramidalis muscle - Present in 80% of individuals, tenses linea alba
- Transversus abdominis - Deepest layer, fibers run horizontally
- Transversalis fascia - Critical surgical plane, continuous with iliac and pelvic fasciae
The retroperitoneal space contains structures of paramount clinical importance, organized into 3 distinct compartments. This potential space becomes actual during pathological processes, accommodating >2 liters of fluid or blood during hemorrhage or infection.
📌 Remember: GREAT - Gerota's fascia (renal), Retroperitoneal organs, Extraperitoneal space, Aorta and IVC, Three compartments - The retroperitoneum houses kidneys, ureters, aorta, IVC, pancreas, and portions of duodenum and colon in 3 fascial compartments
Understanding abdominal organization through systematic regional analysis reveals the architectural logic underlying clinical presentations, surgical approaches, and diagnostic strategies. This foundational knowledge enables prediction of pain referral patterns, infection spread routes, and optimal therapeutic interventions across all abdominal pathologies.
🏗️ Abdominal Architecture: The Body's Engineering Marvel
⚙️ Abdominal Dynamics: The Functional Powerhouse
The digestive coordination system exemplifies abdominal functional integration. Gastric emptying occurs at 1-4 mL/minute for liquids and 2-3 hours for solids, regulated by hormonal feedback involving >12 peptide hormones. Cholecystokinin (CCK) levels increase 5-10 fold postprandially, triggering gallbladder contraction and pancreatic enzyme release within 15-30 minutes.
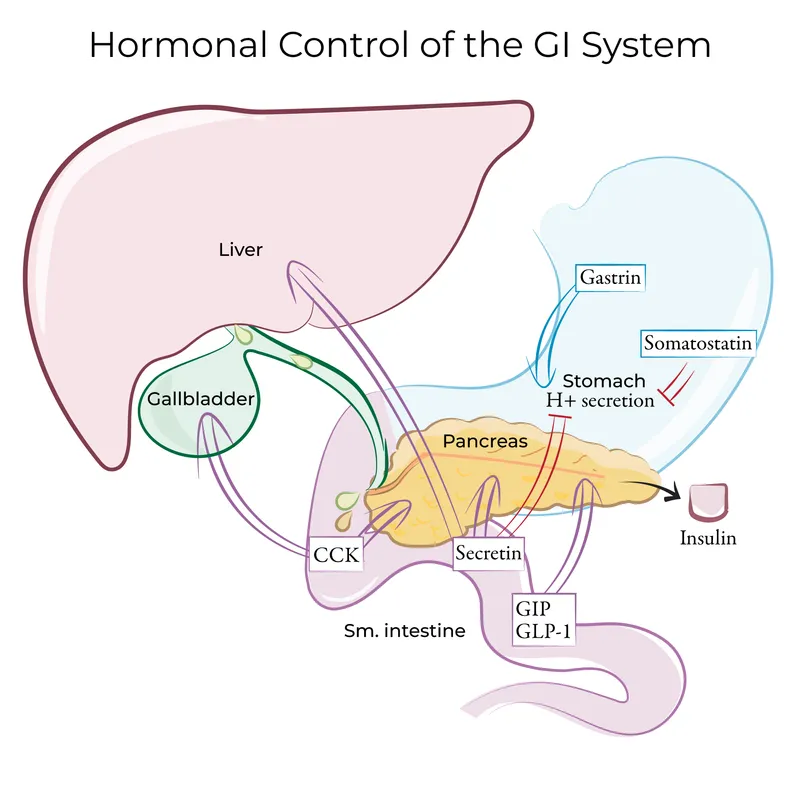
⭐ Clinical Pearl: Postprandial pain occurring 30-60 minutes after fatty meals suggests biliary pathology, while immediate postprandial pain indicates gastric or duodenal disease - timing reflects the physiological sequence of digestive coordination and identifies the anatomical source with >85% accuracy
| Digestive Phase | Duration | Primary Hormones | Organ Response | Flow Rates | Clinical Markers |
|---|---|---|---|---|---|
| Cephalic | 5-10 minutes | Acetylcholine, gastrin | Gastric acid ↑300% | 2-3 mL/min | Early satiety if impaired |
| Gastric | 2-4 hours | Gastrin, histamine | Pepsinogen activation | 1-4 mL/min | Epigastric pain patterns |
| Intestinal | 4-6 hours | CCK, secretin, GIP | Pancreatic enzymes ↑800% | 200-800 mL/hr | Malabsorption syndromes |
| Interdigestive | 90-120 minutes | Motilin, ghrelin | Migrating motor complexes | Baseline | Bacterial overgrowth risk |
- Hepatic Metabolic Zones:
- Zone 1 (Periportal) - Oxidative metabolism, gluconeogenesis, β-oxidation
- Oxygen concentration: 65-70 mmHg
- Primary functions: Glucose production, amino acid metabolism
- Zone 2 (Intermediate) - Mixed metabolism, drug biotransformation
- Transition zone with variable enzyme expression
- Zone 3 (Pericentral) - Glycolysis, lipogenesis, cytochrome P450
- Oxygen concentration: 30-35 mmHg
- Vulnerability: Hypoxic injury, drug toxicity
- Zone 1 (Periportal) - Oxidative metabolism, gluconeogenesis, β-oxidation
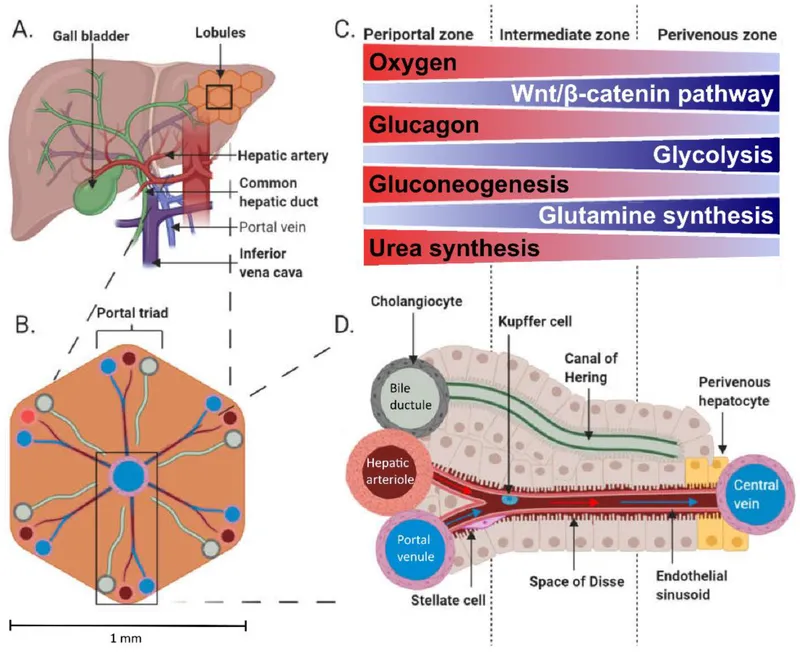
💡 Master This: Hepatic functional reserve explains why >75% liver destruction is required before clinical failure - the liver's regenerative capacity (2-3% daily turnover) and metabolic redundancy provide enormous functional buffer, making early hepatic disease difficult to detect through standard function tests
Renal-adrenal coordination maintains fluid-electrolyte homeostasis through integrated feedback systems. The kidneys filter 180 liters daily (120 mL/minute GFR) while reabsorbing >99% of filtered water and >95% of filtered sodium. Renin-angiotensin-aldosterone system (RAAS) activation occurs within minutes of volume depletion.
📌 Remember: RAAS - Renin (kidney), Angiotensin (lung conversion), Aldosterone (adrenal), Sodium retention - This system responds to volume loss within 5-10 minutes, increases blood pressure by 10-20 mmHg, and restores sodium balance within 24-48 hours
The splanchnic circulation coordinates organ perfusion with metabolic demands. Portal venous flow (1000-1200 mL/minute) carries nutrient-rich blood from intestines to liver, while hepatic arterial flow (300-400 mL/minute) provides oxygenated blood. This dual blood supply enables hepatic metabolic flexibility and functional redundancy.
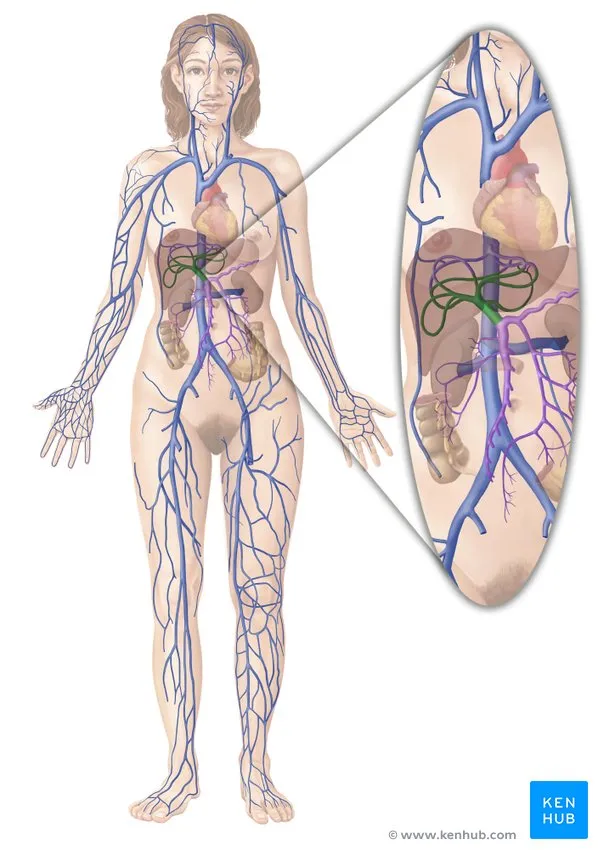
Understanding abdominal functional integration reveals how organ coordination creates physiological efficiency and explains clinical presentation patterns when these integrated systems fail. This mechanistic knowledge enables targeted therapeutic interventions and predictive clinical reasoning.
⚙️ Abdominal Dynamics: The Functional Powerhouse
🎯 Abdominal Pattern Recognition: Clinical Navigation System
⭐ Clinical Pearl: Pain migration patterns provide diagnostic specificity - appendicitis begins as periumbilical pain (visceral T10) then localizes to McBurney's point (somatic), while cholecystitis causes epigastric pain (visceral) radiating to right shoulder (referred C4) in >80% of cases
| Pain Pattern | Initial Location | Migration | Character | Associated Signs | Diagnostic Accuracy |
|---|---|---|---|---|---|
| Appendicitis | Periumbilical | RLQ (McBurney's) | Dull → Sharp | Fever, leukocytosis | 85-95% |
| Cholecystitis | Epigastric | RUQ + right shoulder | Colicky → constant | Murphy's sign 95% | 90-98% |
| Pancreatitis | Epigastric | Back radiation | Boring, constant | Lipase ↑3x normal | 95-100% |
| Bowel Obstruction | Periumbilical | Generalized | Cramping, intermittent | Distension, vomiting | 80-90% |
| Perforated Ulcer | Epigastric | Generalized | Sudden, severe | Rigid abdomen | >95% |
- Inspection Patterns:
- Abdominal contour - Scaphoid (malnutrition), distended (obstruction, ascites)
- Visible peristalsis - Small bowel obstruction in >60% of cases
- Skin changes - Cullen's sign (periumbilical ecchymosis) indicates retroperitoneal bleeding
- Grey Turner's sign - Flank ecchymosis suggests severe pancreatitis
- Spider angiomata - >5 suggests portal hypertension
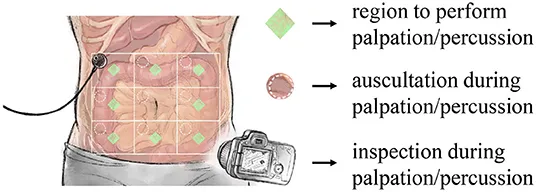
Auscultation patterns reveal functional status and pathological processes. Normal bowel sounds occur 5-35 times/minute with gurgling character. High-pitched tinkling suggests small bowel obstruction, while absent sounds indicate ileus or peritonitis. Bruits over epigastrium suggest mesenteric vascular disease in >70% of cases.
💡 Master This: Rebound tenderness indicates peritoneal irritation but lacks specificity - gentle percussion provides equivalent information with less patient discomfort and equal diagnostic accuracy. Rovsing's sign (RLQ pain with LLQ palpation) shows >80% sensitivity for appendicitis
Laboratory pattern recognition enhances diagnostic precision. White blood cell count elevation >12,000/μL with left shift (>10% bands) suggests bacterial infection with >85% sensitivity. Lipase elevation >3x normal indicates pancreatitis with >95% specificity, while alkaline phosphatase >2x normal suggests biliary obstruction.
- Inflammatory Markers:
- Leukocytosis (>12,000/μL) - Bacterial infection, tissue necrosis
- Left shift (>10% bands) - Acute bacterial process
- C-reactive protein (>50 mg/L) - Significant inflammation
- Procalcitonin (>0.5 ng/mL) - Bacterial sepsis vs viral
- Lactate (>2 mmol/L) - Tissue hypoperfusion, ischemia
Imaging pattern recognition provides anatomical correlation with clinical findings. Ultrasound offers real-time assessment with >95% accuracy for gallbladder pathology and >90% for appendicitis in experienced hands. CT scanning provides comprehensive evaluation with >98% accuracy for most abdominal pathology.
📌 Remember: FAST - Focused assessment, Acute pathology, Systematic approach, Time-sensitive - Emergency abdominal evaluation requires <15 minutes for initial assessment, <30 minutes for laboratory results, and <60 minutes for imaging in unstable patients
Age-related pattern modifications influence diagnostic considerations. Pediatric patients show atypical presentations in >40% of cases, while elderly patients demonstrate blunted inflammatory responses with normal white counts in >30% of serious infections. Pregnancy alters anatomical landmarks and laboratory normals.
Systematic pattern recognition transforms complex clinical presentations into manageable diagnostic algorithms, enabling rapid identification of life-threatening conditions while avoiding unnecessary interventions through evidence-based decision-making.
🎯 Abdominal Pattern Recognition: Clinical Navigation System
🔬 Abdominal Diagnostic Mastery: Systematic Discrimination
Differential diagnosis frameworks enable systematic discrimination between similar presentations. Right upper quadrant pain encompasses >15 potential diagnoses, each requiring specific diagnostic approaches and targeted interventions. Systematic comparison of clinical features, laboratory patterns, and imaging characteristics provides diagnostic precision exceeding 95% when applied methodically.
| RUQ Pain Etiology | Pain Character | Fever Pattern | Laboratory Hallmark | Imaging Finding | Diagnostic Accuracy |
|---|---|---|---|---|---|
| Acute Cholecystitis | Constant, severe | >38.5°C in 70% | Leukocytosis >12K | Wall thickening >4mm | 95-98% |
| Choledocholithiasis | Colicky, intermittent | Variable | Bilirubin >2mg/dL | Ductal dilation >7mm | 90-95% |
| Acute Hepatitis | Dull, constant | Low-grade | ALT >10x normal | Hepatomegaly | >99% |
| Hepatic Abscess | Throbbing, severe | >39°C spiking | WBC >15K, ↑ESR | Rim enhancement | 95-100% |
| Peptic Perforation | Sudden, severe | Variable | Leukocytosis | Free air | >95% |
- Appendicitis Diagnostic Criteria:
- Clinical factors (Alvarado Score components):
- Migration of pain - 1 point (periumbilical to RLQ)
- Anorexia - 1 point (present in >80%)
- Nausea/vomiting - 1 point (follows pain onset)
- RLQ tenderness - 2 points (McBurney's point)
- Rebound tenderness - 1 point (peritoneal irritation)
- Fever >37.3°C - 1 point (present in >60%)
- Leukocytosis >10K - 2 points (inflammatory response)
- Left shift >75% - 1 point (bacterial infection)
- Clinical factors (Alvarado Score components):
Pancreatitis severity discrimination determines management intensity and prognostic expectations. Mild pancreatitis (80% of cases) resolves with conservative management, while severe pancreatitis (20% of cases) carries >30% mortality risk. Early severity assessment within 48 hours guides appropriate care escalation.
⭐ Clinical Pearl: Lipase elevation >3x normal confirms pancreatitis with >95% specificity, but magnitude of elevation does NOT correlate with severity - clinical scoring systems (APACHE-II, Ranson's criteria) provide better prognostic accuracy than enzyme levels alone
| Pancreatitis Severity | Ranson's Criteria | APACHE-II Score | Organ Failure | Local Complications | Mortality Risk |
|---|---|---|---|---|---|
| Mild | <3 criteria | <8 points | None | None | <1% |
| Moderate | 3-4 criteria | 8-12 points | Transient <48hrs | Local fluid | 5-10% |
| Severe | >4 criteria | >12 points | Persistent >48hrs | Necrosis >30% | >30% |
- Obstruction Pattern Recognition:
- Small Bowel Mechanical:
- Vomiting - Early, bilious (within 2-4 hours)
- Distension - Minimal (upper abdomen)
- Pain - Cramping, periumbilical
- Imaging - Dilated loops >3cm, air-fluid levels
- Large Bowel Mechanical:
- Vomiting - Late, feculent (after 12-24 hours)
- Distension - Marked (entire abdomen)
- Pain - Lower abdominal, cramping
- Imaging - Cecal dilation >9cm, transition point
- Small Bowel Mechanical:
💡 Master This: Cecal diameter >9cm on CT imaging indicates impending perforation in large bowel obstruction - this finding mandates immediate surgical intervention as perforation risk exceeds 50% when cecal diameter reaches 12cm
Acute cholangitis discrimination from simple biliary colic requires recognition of Charcot's triad (fever, jaundice, RUQ pain) present in >70% of cases. Reynolds' pentad adds altered mental status and hypotension, indicating severe disease with >20% mortality risk without urgent intervention.
📌 Remember: CHARCOT - Cholangitis triad, Hyperbilirubinemia, Ascending infection, RUQ pain, Cholestasis, Obstruction, Temperature elevation - Charcot's triad occurs in 70% of acute cholangitis, while Reynolds' pentad indicates septic shock requiring emergency decompression
Systematic discrimination between similar abdominal presentations requires methodical comparison of clinical patterns, laboratory findings, and imaging characteristics. This evidence-based approach achieves diagnostic accuracy exceeding 95% while minimizing unnecessary testing and optimizing therapeutic timing.
🔬 Abdominal Diagnostic Mastery: Systematic Discrimination
⚖️ Abdominal Treatment Algorithms: Evidence-Based Intervention
Treatment algorithms transform complex clinical decisions into systematic protocols that improve consistency, reduce errors, and optimize outcomes. Evidence-based pathways incorporate clinical guidelines, outcome data, and resource considerations to guide intervention timing, technique selection, and monitoring strategies.
Acute appendicitis management follows evidence-based protocols that achieve >98% success rates with <2% complication rates. Laparoscopic appendectomy has become standard of care for uncomplicated appendicitis, offering reduced pain, shorter recovery, and lower infection rates compared to open techniques.
| Appendicitis Severity | Treatment Approach | Antibiotic Protocol | Surgical Timing | Success Rate | Complication Rate |
|---|---|---|---|---|---|
| Uncomplicated | Laparoscopic appendectomy | Single dose prophylaxis | <24 hours | >98% | <2% |
| Complicated | Open vs laparoscopic | 7-10 days therapy | Immediate | >95% | 5-10% |
| Perforated | Source control + antibiotics | 10-14 days | Immediate | >90% | 10-20% |
| Abscess | Drainage + antibiotics | 14-21 days | Delayed 6-8 weeks | >85% | 15-25% |

- Cholecystitis Management Protocol:
- Acute Cholecystitis (<72 hours):
- NPO status - Bowel rest, IV hydration
- Pain control - Opioids as needed, avoid anticholinergics
- Antibiotics - Ampicillin-sulbactam or ceftriaxone + metronidazole
- Early surgery - Laparoscopic cholecystectomy within 72 hours
- Delayed Presentation (>72 hours):
- Conservative management - Antibiotics, supportive care
- Interval cholecystectomy - 6-8 weeks after resolution
- Percutaneous drainage - High-risk patients, severe disease
- Acute Cholecystitis (<72 hours):
⭐ Clinical Pearl: Early laparoscopic cholecystectomy within 72 hours reduces total hospital stay by 3-5 days, decreases complications by >50%, and eliminates recurrence risk compared to delayed surgical approaches - timing is the critical success factor
Pancreatitis management follows severity-stratified protocols that optimize fluid resuscitation, pain control, and nutritional support. Aggressive fluid resuscitation with 250-500 mL/hour of crystalloid during the first 12-24 hours reduces organ failure risk by >40% and mortality by >30%.
💡 Master This: Enteral nutrition within 48 hours reduces infectious complications by >50% in severe pancreatitis compared to parenteral nutrition - the gut barrier function preservation through early feeding prevents bacterial translocation and systemic infection
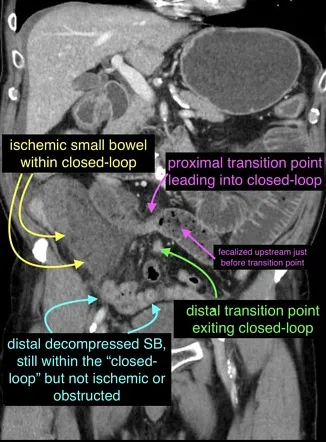
Bowel obstruction algorithms distinguish operative from non-operative candidates based on clinical factors and imaging findings. Small bowel obstruction resolves non-operatively in >80% of partial obstructions but requires surgery in >90% of complete obstructions with closed-loop configuration.
- Obstruction Management Decision Tree:
- Non-operative Candidates:
- Partial obstruction - Contrast passage on CT
- No peritoneal signs - Soft abdomen, no rebound
- Stable vital signs - No fever, normal WBC
- Previous surgery - Adhesive etiology likely
- Operative Indications:
- Complete obstruction - No contrast passage
- Closed-loop obstruction - Ischemia risk
- Peritoneal signs - Perforation concern
- Failed conservative management - >72 hours without resolution
- Non-operative Candidates:
Acute cholangitis requires emergency biliary decompression within 24-48 hours to prevent septic shock and multiorgan failure. ERCP with sphincterotomy achieves >95% success rates for stone extraction and drainage establishment. Percutaneous drainage serves as alternative when ERCP fails or is contraindicated.
📌 Remember: ERCP - Emergency decompression, Rapid intervention, Cholangitis treatment, Procedure of choice - ERCP within 24 hours reduces mortality from >20% to <5% in acute cholangitis by establishing drainage and removing obstructing stones
Evidence-based treatment algorithms provide systematic frameworks that standardize care, improve outcomes, and reduce variability in abdominal emergency management. These protocols integrate best evidence with clinical judgment to optimize patient outcomes across diverse presentations.
⚖️ Abdominal Treatment Algorithms: Evidence-Based Intervention
🌐 Abdominal Integration Networks: Multi-System Orchestration
Multi-system integration within the abdomen creates emergent properties that exceed individual organ capabilities. The gut-liver axis processes >90% of absorbed nutrients through coordinated metabolic pathways, while the enteric nervous system (>500 million neurons) functions as the "second brain", coordinating digestive processes independently of central nervous control.

Neuroendocrine integration coordinates abdominal function through >30 peptide hormones and multiple neural pathways. The gut-brain axis involves bidirectional communication through vagal, sympathetic, and hormonal pathways that influence mood, cognition, and systemic metabolism. Ghrelin and leptin regulate energy homeostasis, while GLP-1 and GIP coordinate glucose metabolism.
| Integration Network | Primary Mediators | Response Time | Physiological Effect | Clinical Relevance | Dysfunction Consequences |
|---|---|---|---|---|---|
| Gut-Brain Axis | Vagus nerve, serotonin | Seconds-minutes | Mood, appetite regulation | IBS, depression | Functional GI disorders |
| Gut-Liver Axis | Portal circulation | Minutes-hours | Metabolic processing | NAFLD, diabetes | Metabolic syndrome |
| Gut-Immune Axis | Cytokines, GALT | Hours-days | Immune surveillance | IBD, allergies | Autoimmune disease |
| Entero-Pancreatic | GLP-1, GIP, CCK | Minutes | Glucose homeostasis | Diabetes management | Hyperglycemia |
| Hepato-Renal | Albumin, toxins | Hours | Fluid balance | Hepatorenal syndrome | Kidney failure |
Metabolic integration networks coordinate energy homeostasis across multiple organ systems. Hepatic glucose production responds to pancreatic insulin and glucagon within minutes, while adipose tissue provides long-term energy storage and endocrine signaling through adipokines. Muscle tissue serves as glucose sink and amino acid reservoir.
- Metabolic Network Components:
- Liver (Central processor):
- Glucose homeostasis - Glycogenolysis, gluconeogenesis
- Lipid metabolism - Fatty acid synthesis, ketogenesis
- Protein synthesis - >50 plasma proteins
- Pancreas (Metabolic regulator):
- Insulin secretion - Glucose uptake, anabolic processes
- Glucagon release - Glucose production, catabolic processes
- Digestive enzymes - Nutrient breakdown
- Adipose tissue (Energy storage + endocrine):
- Leptin production - Satiety signaling
- Adiponectin release - Insulin sensitivity
- Free fatty acid mobilization
- Liver (Central processor):
Immune integration within the abdomen involves gut-associated lymphoid tissue (GALT), representing >70% of total immune system mass. Peyer's patches, mesenteric lymph nodes, and lamina propria create immune surveillance networks that distinguish pathogenic from commensal organisms while maintaining oral tolerance to dietary antigens.
💡 Master This: Intestinal barrier function depends on tight junction integrity maintained by zonulin, claudin, and occludin proteins - barrier dysfunction allows bacterial translocation, triggering systemic inflammation and contributing to sepsis, SIRS, and multiorgan failure in critically ill patients
Vascular integration networks coordinate perfusion with metabolic demands through autoregulation and neural control. Splanchnic circulation receives 25-30% of cardiac output during digestion, redistributed through sympathetic vasoconstriction during stress or exercise. Portal-systemic collaterals develop when portal pressure exceeds 12 mmHg.
Endocrine integration involves >15 abdominal hormone-producing tissues that coordinate local and systemic functions. Incretin hormones (GLP-1, GIP) coordinate postprandial glucose control, while ghrelin and peptide YY regulate appetite and gastric emptying. Somatostatin provides negative feedback across multiple systems.
- Abdominal Endocrine Networks:
- Pancreatic islets - Insulin, glucagon, somatostatin
- Enteroendocrine cells - GLP-1, GIP, CCK, secretin
- Gastric mucosa - Gastrin, ghrelin
- Duodenal mucosa - Secretin, CCK
- Ileal mucosa - GLP-1, peptide YY
📌 Remember: INTEGRATION - Immune surveillance, Neuroendocrine control, Tissue coordination, Energy metabolism, Gut-brain axis, Regulatory networks, Autoregulation, Transport systems, Inflammatory responses, Organ crosstalk, Nutrient processing - Abdominal integration involves >10 distinct networks coordinating physiological homeostasis
Understanding multi-system integration reveals how abdominal pathology creates systemic consequences and explains complex clinical presentations that span multiple organ systems. This network perspective guides comprehensive therapeutic approaches that address underlying integration failures rather than isolated organ dysfunction.
🌐 Abdominal Integration Networks: Multi-System Orchestration
🎯 Abdominal Mastery Arsenal: Clinical Command Center
Essential Clinical Thresholds form the foundation of rapid decision-making. These quantitative benchmarks enable immediate risk stratification, intervention timing, and outcome prediction across diverse abdominal presentations. Memorizing critical numbers transforms complex clinical scenarios into manageable decision points.
| Clinical Parameter | Normal Range | Mild Abnormal | Moderate Abnormal | Severe Abnormal | Critical Action |
|---|---|---|---|---|---|
| Lipase | <60 U/L | 60-180 U/L | 180-300 U/L | >300 U/L | Pancreatitis protocol |
| Bilirubin Total | <1.2 mg/dL | 1.2-2.0 mg/dL | 2.0-5.0 mg/dL | >5.0 mg/dL | Biliary obstruction |
| Lactate | <2 mmol/L | 2-4 mmol/L | 4-8 mmol/L | >8 mmol/L | Sepsis protocol |
| WBC Count | 4-11 K/μL | 11-15 K/μL | 15-20 K/μL | >20 K/μL | Infection workup |
| Cecal Diameter | <6 cm | 6-9 cm | 9-12 cm | >12 cm | Emergency surgery |
Rapid Assessment Protocols enable systematic evaluation within <10 minutes for stable patients and <5 minutes for unstable presentations. ABCDE approach (Airway, Breathing, Circulation, Disability, Exposure) provides primary survey, followed by focused abdominal assessment using standardized examination sequences.
- 5-Minute Abdominal Assessment:
- Minute 1 - Vital signs, general appearance, pain assessment
- Minute 2 - Inspection (distension, scars, masses)
- Minute 3 - Auscultation (bowel sounds, bruits)
- Minute 4 - Percussion (organ borders, fluid)
- Minute 5 - Palpation (tenderness, masses, organomegaly)
💡 Master This: Murphy's sign has >95% specificity for acute cholecystitis when properly performed - inspiratory arrest during RUQ palpation indicates gallbladder inflammation. False positives occur with hepatitis or right lower lobe pneumonia
Emergency Decision Algorithms provide systematic approaches to time-sensitive conditions. Acute abdomen evaluation follows structured pathways that prioritize life-threatening conditions while avoiding unnecessary delays in definitive management.
Diagnostic Mnemonics enhance pattern recognition and reduce diagnostic errors. Systematic memory aids ensure comprehensive differential consideration while preventing anchoring bias and premature closure.
📌 Remember: VINDICATE for abdominal pain differentials - Vascular (AAA, mesenteric ischemia), Infectious (appendicitis, diverticulitis), Neoplastic (bowel cancer), Degenerative (adhesions), Iatrogenic (post-surgical), Congenital (malrotation), Autoimmune (IBD), Traumatic (perforation), Endocrine (DKA) - covers >95% of abdominal pathology
Treatment Quick-Reference provides immediate access to evidence-based protocols for common abdominal emergencies. Standardized order sets reduce medication errors and ensure comprehensive care.
- Appendicitis Protocol:
- NPO status - Nothing by mouth
- IV access - 18-gauge or larger
- Pain control - Morphine 0.1mg/kg or hydromorphone 0.015mg/kg
- Antibiotics - Cefoxitin 2g IV or ceftriaxone 1g + metronidazole 500mg
- Laboratory - CBC, CMP, urinalysis, pregnancy test
- Imaging - CT abdomen/pelvis with IV contrast
Complication Recognition enables early intervention before irreversible damage occurs. Warning signs of deterioration require immediate escalation and aggressive management.
| Complication | Early Signs | Late Signs | Intervention Window | Mortality Risk |
|---|---|---|---|---|
| Bowel Perforation | Localized tenderness | Generalized peritonitis | <6 hours | <5% vs >20% |
| Septic Shock | Tachycardia, fever | Hypotension, oliguria | <3 hours | <10% vs >40% |
| Bowel Ischemia | Pain out of proportion | Bloody diarrhea | <6 hours | <15% vs >80% |
| Compartment Syndrome | Tense abdomen | Organ dysfunction | <2 hours | <20% vs >60% |
The Abdominal Mastery Arsenal transforms complex clinical scenarios into systematic approaches that optimize diagnostic accuracy, treatment timing, and patient outcomes through evidence-based protocols and rapid-access reference tools.
🎯 Abdominal Mastery Arsenal: Clinical Command Center
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for NEET-PG prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app




















